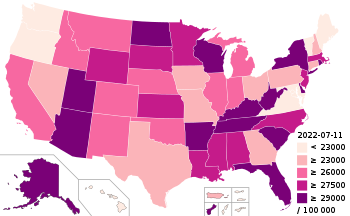
COVID-19 pandemic in the United States
| COVID-19 pandemic in the United States | |
|---|---|
COVID-19 cases per 100,000 people by state, as of May 1 | |
| Disease | COVID-19 |
| Virus strain | SARS-CoV-2 |
| Location | United States |
| First outbreak | Wuhan, Hubei, China[1] |
| Index case | Chicago, Illinois (earliest known arrival)[2] Everett, Washington (first case report)[3] |
| Arrival date | January 13, 2020[4] (1 year and 5 months ago) |
| Confirmed cases | |
| Suspected cases‡ | 114,621,082 (CDC estimate in March 2021)[7] |
| Recovered |
|
Deaths | |
| Fatality rate | |
| Government website | |
| coronavirus | |
| ‡Suspected cases have not been confirmed by laboratory tests as being due to this strain, although some other strains may have been ruled out. | |
The COVID-19 pandemic in the United States is part of the worldwide pandemic of coronavirus disease 2019 (COVID-19). More than 33.4 million confirmed cases have been reported since January 2020, resulting in more than 599,000 deaths, the most of any country, and the twentieth-highest per capita worldwide.[6][9] As many infections go undetected, the Centers for Disease Control estimates that as of March 2021, there have been a total 114.6 million infections in the United States.[7] The U.S. has about one-fifth of the world's confirmed cases and deaths. COVID-19 became the third-leading cause of death in the U.S. in 2020, behind heart disease and cancer.[10] U.S. life expectancy dropped from 78.8 years in 2019 to 77.8 years in the first half of 2020.[11]
On December 31, 2019, China announced the discovery of a cluster of pneumonia cases in Wuhan. The first American case was reported on January 20, and President Donald Trump declared the U.S. outbreak a public health emergency on January 31. Restrictions were placed on flights arriving from China,[12][13] but the initial U.S. response to the pandemic was otherwise slow, in terms of preparing the healthcare system, stopping other travel, and testing.[14][15][16][a] Meanwhile, Trump remained optimistic and was accused by his critics of underestimating the severity of the virus.
The first known American deaths occurred in February.[18][b] On March 6, 2020, Trump signed the Coronavirus Preparedness and Response Supplemental Appropriations Act, which provided $8.3 billion in emergency funding for federal agencies to respond to the outbreak.[19] On March 13, President Trump declared a national emergency.[20] In mid-March, the Trump administration started to purchase large quantities of medical equipment,[21] and in late March, it invoked the Defense Production Act of 1950 to direct industries to produce medical equipment.[22] By April 17, the federal government approved disaster declarations for all states and territories. By mid-April, cases had been confirmed in all fifty U.S. states, and by November in all inhabited U.S. territories.
A second rise in infections began in June 2020, following relaxed restrictions in several states, leading to daily cases surpassing 60,000.[23] A third rise in infections began around mid-October, leading to daily cases reaching over 100,000 by the end of the month.[24][25] A fourth rise in infections began around late March 2021 amidst the rise of a more easily transmissible new SARS-CoV-2 variant from the United Kingdom, just as COVID-19 vaccines began to be administered in the country, but stagnated before another major spike.[26][27] High levels of vaccine hesitancy in parts of the country have hampered vaccination efforts.
State and local responses to the outbreak have included mask mandates, prohibition and cancellation of large-scale gatherings (including festivals and sporting events), stay-at-home orders, and school closures.[28] Disproportionate numbers of cases have been observed among Black and Latino populations,[29][30][31] and there were reported incidents of xenophobia and racism against Asian Americans.[32] Clusters of infections and deaths have occurred in many areas.[c]
Timeline
December 2019 to February 2020
In late November 2019, coronavirus infections had first broken out in Wuhan, China.[35][36] China publicly reported the cluster on December 31, 2019.[3] On January 6, U.S. Health and Human Services offered to send China a team of Centers for Disease Control and Prevention (CDC) health experts to help contain the outbreak, but China ignored the offer.[37] The CDC said this refusal contributed to the U.S. and other countries getting a late start in identifying the danger and taking early action.[38][39]
After China confirmed that the cluster of infections was caused by a novel infectious coronavirus[3] on January 7, the CDC issued an official health advisory the following day.[40] The World Health Organization (WHO) warned on January 10 about the strong possibility of human-to-human transmission and urged precautions.[41] On January 20, the WHO and China both confirmed that human-to-human transmission had indeed occurred.[42] The CDC immediately activated its Emergency Operations Center (EOC) to respond to the outbreak in China.[43] Also, the first report of a COVID-19 case in the U.S. was reported.[3] After other cases were reported, on January 30, the WHO declared a Public Health Emergency of International Concern (PHEIC) – its highest level of alarm[44] – warning that "all countries should be prepared for containment."[45][46][e] The same day, the CDC confirmed the first person-to-person case in America.[48] The next day, the U.S. declared a public health emergency.[49] Although by that date there were only seven known cases in the U.S., the HHS and CDC reported that there was a likelihood of further cases appearing in the country.[49]
The Trump administration evacuated American nationals from Wuhan in late January; the evacuees were greeted by officials who did not wear protective gear because the Trump administration worried about "bad optics".[50] On February 2, the U.S. enacted travel restrictions to and from China.[13] On February 6, the earliest confirmed American death with COVID-19 (that of a 57-year-old woman) occurred in Santa Clara County, California. The CDC did not report its confirmation until April 21,[18] by which point nine other COVID-19 deaths had occurred in Santa Clara County.[51] The virus had been circulating undetected at least since early January and possibly as early as November.[52] On February 25, the CDC warned the American public for the first time to prepare for a local outbreak.[53][54] The next day "Patient Zero" (Manhattan attorney Lawrence Garbuz, then thought to be the first community-acquired case) became ill in New York City.[55][56][57]
In February, Vice President Mike Pence took over for Secretary Alex Azar as chair of the White House Coronavirus Task Force.[58]
March to April 2020

By March 11, the virus had spread to 110 countries, and the WHO officially declared a pandemic.[28] The CDC had already warned that large numbers of people needing hospital care could overload the healthcare system, which would lead to otherwise preventable deaths.[59][60] Dr. Anthony Fauci said the mortality from the coronavirus was 10 times higher than the common flu.[61]
By March 12, diagnosed cases of COVID-19 in the U.S. exceeded a thousand.[62] On March 16, the White House advised against any gatherings of more than ten people.[63] Three days later, the United States Department of State advised U.S. citizens to avoid all international travel.[64][dead link]
By the middle of March, all fifty states were able to perform tests with a doctor's approval, either from the CDC or from commercial labs. However, the number of available test kits remained limited, which meant the true number of people infected had to be estimated.[65] As cases began spreading throughout the nation, federal and state agencies began taking urgent steps to prepare for a surge of hospital patients. Among the actions was establishing additional places for patients in case hospitals became overwhelmed.[66] Manpower from the military and volunteer armies were called up to help construct the emergency facilities.[67][68]
Throughout March and early April, several state, city, and county governments imposed "stay at home" quarantines on their populations to stem the spread of the virus.[69] By March 27, the country had reported over 100,000 cases.[70] On April 2, at President Trump's direction, the Centers for Medicare & Medicaid Services (CMS) and CDC ordered additional preventive guidelines to the long-term care facility industry.[71] On April 11, the U.S. death toll became the highest in the world when the number of deaths reached 20,000, surpassing that of Italy.[72] On April 19, the CMS added new regulations requiring nursing homes to inform residents, their families and representatives, of COVID-19 cases in their facilities.[73] On April 28, the total number of confirmed cases across the country surpassed one million.[74]
May to August 2020
By May 27, less than four months after the pandemic reached the U.S., 100,000 Americans had died with COVID-19.[75] State economic reopenings and lack of widespread mask orders resulted in a sharp rise in cases across most of the continental U.S. outside of the Northeast.[76] A study conducted in May 2020 indicated that the true number of COVID-19 cases in the United States was much higher than the number of confirmed cases with some locations having 6–24 times higher infections, which was further confirmed by a later population-wide serosurvey.[77][78][79]
On July 6, the United States Department of State announced U.S. withdrawal from the World Health Organization effective July 6, 2021.[80] The U.S. passed five million COVID-19 cases by August 8.[81]
On July 10, the CDC adopted the Infection Fatality Ratio (IFR), "the number of individuals who die of the disease among all infected individuals (symptomatic and asymptomatic)", as a new metric for disease severity, replacing the Symptomatic Case Fatality Ratio and the Symptomatic Case Hospitalization Ratio. Per the CDC, the IFR "takes into account both symptomatic and asymptomatic cases, and may therefore be a more directly measurable parameter for disease severity for COVID-19".[82]
In July, U.S. PIRG and 150 health professionals sent a letter asking the federal government to "shut it down now, and start over".[83] In July and early August, requests multiplied, with a number of experts asking for lockdowns of "six to eight weeks"[84] that they believed would restore the country by October 1, in time to reopen schools and have an in-person election.[85]
In August, over 400,000 people attended the 80th Sturgis Motorcycle Rally in Sturgis, South Dakota, and from there, at least 300 people in more than 20 states were infected.[86] The CDC followed up with a report on the associated 51 confirmed primary event-associated cases, 21 secondary cases, and five tertiary cases in the neighboring state of Minnesota, where one attendee died of COVID-19.[87]
September to December 2020
On September 22, the U.S. passed 200,000 deaths, according to data from Johns Hopkins University.[88] In early October, an unprecedented series of high-profile U.S. political figures and staffers announced they had tested positive for COVID-19.[89][90] On October 2, Trump announced on Twitter that both he and the First Lady had tested positive for the coronavirus and would immediately quarantine.[91][90] Trump was given an experimental Regeneron product with two monoclonal antibodies[92][f] and taken to Walter Reed National Military Medical Center,[94] where he was given remdesivir and dexamethasone.[95]
USA Today studied the aftermath of presidential election campaigning, recognizing that causation was impossible to determine. Among their findings, cases increased 35 percent compared to 14 percent for the state after a Trump rally in Beltrami County, Minnesota. One case was traced to a Joe Biden rally in Duluth.[96]
On November 9, President-elect Biden's transition team announced his COVID-19 Advisory Board.[97] On the same day, the total number of cases had surpassed ten million[98] while the total had risen by over a million in the ten days prior, averaging 102,300 new cases per day.[99] Pfizer also announced that its COVID-19 vaccine may be up to ninety percent effective.[100][101] In November, the Trump administration reached an agreement with a number of retail outlets, including pharmacies and supermarkets, to make the COVID-19 vaccine free once available.[102]
In spite of recommendations by the government not to travel, more than two million people flew on airlines during the Thanksgiving period.[103] On December 8, the U.S. passed fifteen million cases, with about one out of every 22 Americans having tested positive since the pandemic began.[104] By December 12, TSA employees across U.S. airports had a 38 percent increase in COVID-19 infections.[105] On December 14, the U.S. passed 300,000 deaths, representing an average of more than 961 deaths per day since the first known death on February 6. More than 50,000 deaths were reported in the past month, with an average of 2,403 daily deaths occurring in the past week.[106]
On December 24, following concerns over a probably more easily transmissible new SARS-CoV-2 variant from the United Kingdom (B.1.1.7), the CDC announced testing requirements for American passengers traveling from the UK, to be administered within 72 hours, starting on December 28.[107][108] On December 29, the U.S. reported the first case of this variant in Colorado. The patient had no travel history, leading the CDC to state, "Given the small fraction of US infections that have been sequenced, the variant could already be in the United States without having been detected."[109]
January to April 2021
On January 1, 2021, the U.S. had twenty million cases, representing an increase of more than a million over the past week and ten million in less than two months.[110][111] On January 6, the CDC announced that it had found at least 52 confirmed cases of the B.1.1.7 variant, and it also stressed that there could already be more cases in the country.[112] In the following days, more cases of the variant were reported in other states, leading former CDC director Tom Frieden to express his concerns that the U.S. will soon face "close to a worst-case scenario".[113] It was believed the variant had been present in the U.S. since October.[114]
On January 19, the U.S. passed 400,000 deaths, just five weeks after the country passed 300,000 deaths.[115] On January 22, the U.S. passed 25 million cases, with one of every 13 Americans testing positive for COVID-19.[116] On January 25, the U.S. reported its first case of a new SARS-CoV-2 variant from Brazil (P.1) in Minnesota.[117] Three days later, on January 28, the country reported its first two cases of a new, possibly vaccine-resistant SARS-CoV-2 variant from South Africa (B.1.351) in South Carolina.[118] On February 22, the U.S. passed 500,000 deaths, just five weeks after the country passed 400,000 deaths.[119] By March 5, more than 2,750 cases of COVID-19 variants were detected in 47 states; Washington, D.C.; and Puerto Rico.[120]
In the first prime time address of his presidency on March 11, Biden announced his plan to push states to make vaccines available to all adults by May 1, with the aim of making small gatherings possible by July 4.[121] On March 24, the U.S. passed thirty million cases, just as a number of states began to expand the eligibility age for COVID-19 vaccines.[122] Experts began warning against public relaxation of COVID-19 mitigation measures as vaccines continue to be administered, with one, CDC director Rochelle Walensky, warning of a new rise in cases.[123]
By March 27, more than 8,000 cases of the B.1.1.7 variant were reported across 51 jurisdictions.[123] By April 1, the number increased to more than 11,000, with cases mostly being reported in Florida and Michigan.[124] By April 7, the B.1.1.7 variant had become the dominant COVID-19 strain in the U.S.[27] On April 12, the U.S. reported its first cases of a new "double mutant" SARS-CoV-2 variant from India (B.1.617) in California.[125] By April 25, the country's seven-day average of new infections was reported to be decreasing, but concerns were raised about drops in vaccine demand in certain parts of the U.S., which were attributed to vaccine hesitancy.[126][127][128] On April 29, the CDC estimated that roughly 35% of the U.S. population had been infected with the virus as of March 2021, about four times higher than the official reported numbers.[129]
May 2021
On May 4, Biden announced a new goal of having 70 percent of all adults in the U.S. receive at least one COVID-19 vaccine shot by July 4, along with steps to vaccinate teenagers and more inaccessible populations.[130] On May 6, a study by the Institute for Health Metrics and Evaluation estimated that the true COVID-19 death toll in the U.S. was more than 900,000 people.[131] On May 9, Dr. Fauci confirmed that the U.S. death toll was likely undercounted.[132]
On May 13, the CDC changed their guidance and stated that fully vaccinated individuals do not need to wear masks in most situations.[133] Some states ended their mask mandates shortly after, while others maintained the mandate. The CDC was criticized for confusion resulting from the announcement as it did not remove existing state and local mandates. The guidance did not remove the federal mask mandate on public transportation.[134]
Responses
On January 28, the CDC updated its China travel recommendations to level 3, its highest alert.[37] On February 8, the WHO's director-general announced that a team of international experts had been assembled to travel to China and he hoped officials from the CDC would also be part of that mission.[135][136] In late January, Boeing announced a donation of 250,000 medical masks to help address China's supply shortages.[137] On February 7, The State Department said it had facilitated the transportation of nearly eighteen tons of medical supplies to China, including masks, gowns, gauze, respirators, and other vital materials.[138] On the same day, U.S. Secretary of State Pompeo announced a $100 million pledge to China and other countries to assist with their fights against the virus.[139]
Contact tracing is a tool to control transmission rates during the reopening process. Some states like Texas and Arizona opted to proceed with reopening without adequate contact tracing programs in place. Health experts have expressed concerns about training and hiring enough personnel to reduce transmission. Privacy concerns have prevented measures such as those imposed in South Korea where authorities used cellphone tracking and credit card details to locate and test thousands of nightclub patrons when new cases began emerging.[140] Funding for contact tracing is thought to be insufficient, and even better-funded states have faced challenges getting in touch with contacts. Congress has allocated $631 million for state and local health surveillance programs, but the Johns Hopkins Center for Health Security estimates that $3.6 billion will be needed. The cost rises with the number of infections, and contact tracing is easier to implement when the infection count is lower. Health officials are also worried that low-income communities will fall further behind in contact tracing efforts which "may also be hobbled by long-standing distrust among minorities of public health officials".[141] As of July 1, only four states are using contact tracing apps as part of their state-level strategies to control transmission. The apps document digital encounters between smartphones, so the users will automatically be notified if someone they had contact with has tested positive. Public health officials in California claim that most of the functionality could be duplicated by using text, chat, email, and phone communications.[142]
In the United States, remdesivir is indicated for use in adults and adolescents (aged twelve years and older with body weight at least 40 kilograms (88 lb)) for the treatment of COVID‑19 requiring hospitalization.[143] The FDA issued an emergency use authorization (EUA) for the combination of baricitinib with remdesivir, for the treatment of suspected or laboratory confirmed COVID-19 in hospitalized people two years of age or older requiring supplemental oxygen, invasive mechanical ventilation, or extracorporeal membrane oxygenation (ECMO).[144] In early March, President Trump directed the FDA to test certain medications to discover if they had the potential to treat COVID-19 patients.[145] Among those were chloroquine and hydroxychloroquine, which have been successfully used to treat malaria for over fifty years. A small test in France by researcher Didier Raoult had given positive results, although the study was criticized for design flaws, small sample size, and the fact that it was published before peer review.[146] On March 28, the FDA issued an Emergency Use Authorization (EUA) which allowed certain hospitalized COVID-19 patients to be treated with hydroxychloroquine or chloroquine.[147][145][148][149] On June 15, the FDA revoked the EUA for hydroxychloroquine and chloroquine as potential treatments for COVID-19, saying the available evidence showed "no benefit for decreasing the likelihood of death or speeding recovery".[150] However, Trump continued to promote the use of hydroxychloroquine for COVID-19 by late July.[151]
From early 2020, more than 70 companies worldwide (with five or six operating primarily in the U.S.) began vaccine research.[152][153] In preparation for large-scale production, Congress set aside more than $3.5 billion for this purpose as part of the CARES Act.[154][153] On November 20, 2020, the Pfizer–BioNTech partnership submitted a request for emergency use authorization for its vaccine to the Food and Drug Administration (FDA),[155][156] which was granted on December 11.[157][158] On December 18, 2020, the FDA granted the Moderna vaccine emergency use authorization,[159][160] which Moderna had requested on November 30, 2020.[161][162] Starting on December 14, 2020, the first doses of COVID-19 vaccine were administered.[163]
Polling showed a significant partisan divide regarding the outbreak.[164] In February, similar numbers of Democrats and Republicans believed COVID-19 was "a real threat": 70% and 72%, respectively. By mid-March, 76% of Democrats viewed COVID-19 as "a real threat", while only 40% of Republicans agreed.[165] In mid-March, various polls found Democrats were more likely than Republicans to believe "the worst was yet to come" (79–40%), to believe their lives would change in a major way due to the outbreak (56–26%),[166] and to take certain precautions against the virus (83–53%).[167] The CDC was the most trusted source of information about the outbreak (85%), followed by the WHO (77%), state and local government officials (70–71%), the news media (47%), and President Trump (46%).[167] A May 2020 poll concluded that 54% of people in the U.S. felt the federal government was doing a poor job in stopping the spread of COVID-19 in the country. 57% felt the federal government was not doing enough to address the limited availability of COVID-19 testing. 58% felt the federal government was not doing enough to prevent a second wave of COVID-19 cases later in 2020.[168] In September 2020, Pew Research Center found that the global image of the United States had suffered in many foreign nations. In some nations, the United States' favorability rating had reached a record low since Pew began collecting this data nearly twenty years ago. Across thirteen different nations, a median of fifteen percent of respondents rated the U.S. response to the pandemic positively.[169]
Impacts
Economic
The pandemic, along with the resultant stock market crash and other impacts, led a recession in the United States following the economic cycle peak in February 2020.[170] The economy contracted 4.8 percent from January through March 2020,[171] and the unemployment rate rose to 14.7 percent in April.[172] The total healthcare costs of treating the epidemic could be anywhere from $34 billion to $251 billion according to analysis presented by The New York Times.[173] A study by economists Austan Goolsbee and Chad Syverson indicated that most economic impact due to consumer behavior changes was prior to mandated lockdowns.[174] During the second quarter of 2020, the U.S. economy suffered its largest drop on record, with GDP falling at an annualized rate of 32.9 percent. As of June 2020, the U.S. economy was over ten percent smaller than it was in December 2019.[175]

In September, Bain & Company reported on the tumultuous changes in consumer behavior before and during the COVID-19 pandemic. Potentially permanently, they found acceleration towards e-commerce, online primary healthcare, livestreamed gym workouts, and moviegoing via subscription television. Concurrent searches for both low-cost and premium products, and a shift to safety over sustainability, occurred alongside rescinded bans and taxes on single-use plastics, and losses of three to seven years of gains in out-of-home foodservice.[176] OpenTable estimated in May that 25 percent of American restaurants would close their doors permanently.[177]
The economic impact and mass unemployment caused by the COVID-19 pandemic has raised fears of a mass eviction crisis,[178][179][180][181] with an analysis by the Aspen Institute indicating 30–40 million are at risk for eviction by the end of 2020.[182][183] According to a report by Yelp, about sixty percent of U.S. businesses that have closed since the start of the pandemic will stay shut permanently.[184]
| Variable | Feb | Mar | Apr | May | June | July | Aug | Sep | Oct | Nov |
|---|---|---|---|---|---|---|---|---|---|---|
| Jobs, level (000s)[185] | 152,463 | 151,090 | 130,303 | 133,002 | 137,802 | 139,582 | 140,914 | 141,720 | 142,373 | 142,629 |
| Jobs, monthly change (000s)[185] | 251 | −1,373 | −20,787 | 2,699 | 4,800 | 1,780 | 1,371 | 661 | 653 | 256 |
| Unemployment rate %[186] | 3.5% | 4.4% | 14.7% | 13.3% | 11.1% | 10.2% | 8.4% | 7.9% | 6.9% | 6.7% |
| Number unemployed (millions)[187] | 5.8 | 7.1 | 23.1 | 21.0 | 17.8 | 16.3 | 13.6 | 12.6 | 11.1 | 10.7 |
| Employment to population ratio %, age 25–54[188] | 80.5% | 79.6% | 69.7% | 71.4% | 73.5% | 73.8% | 75.3% | 75.0% | 76.0% | 76.0% |
| Inflation rate % (CPI-All)[189] | 2.3% | 1.5% | 0.4% | 0.2% | 0.7% | 1.0% | TBD | TBD | TBD | TBD |
| Stock market S&P 500 (avg. level)[190] | 3,277 | 2,652 | 2,762 | 2,920 | 3,105 | 3,230 | 3,392 | 3,380 | 3,270 | 3,694 |
| Debt held by public ($ trillion)[191] | 17.4 | 17.7 | 19.1 | 19.9 | 20.5 | 20.6 | 20.8 | 21.0 | 21.2 | 21.3 |
Rural communities
In May, daily infection and death rates were still higher per capita in densely populated cities and suburbs but were increasing faster in rural counties. Of the 25 counties with the highest per capita case rates in May, 20 had a meatpacking plant or prison where the virus was able to spread unchecked.[192] By July, rural communities with populations less than 50,000 had some of the highest rates of new daily cases per capita. Factors contributing to the spread of COVID-19 in these communities are high rates of obesity,[193][dubious ] the relatively high numbers of elderly residents, immigrant laborers with shared living conditions and meat-processing plants.[194]
Social
The pandemic has had far-reaching consequences beyond the disease itself and efforts to contain it, including political, cultural, and social implications.
From the earliest days of the pandemic, there were reported incidents of xenophobia and racism against Asian Americans.[32] During the first year, an ad-hoc organization called Stop AAPI Hate received 3,795 reports of racism against Asian Americans and Pacific Islanders.[195]
Disproportionate numbers of cases have been observed among Black and Latino populations.[29][30][31] Of four studies published in September 2020, three found clear disparities due to race and the fourth found slightly better survival rates for Hispanics and Blacks.[196] As of September 15, 2020, Blacks had COVID-19 mortality rates more than twice as high as the rate for Whites and Asians, who have the lowest rates.[197] CNN reported in May 2020 that the Navajo Nation had the highest rate of infection in the United States.[198] Additionally, a study published by the New England Journal of Medicine in July 2020 revealed that the effect of stress and weathering on minority groups decreases their stamina against COVID.[199]
From 2019 to the first half of 2020, in the United States the life expectancy of a white person decreased 0.8 years; a Hispanic person, 1.9 years; and a Black person, 2.7 years.[11] The COVID Tracking Project[200] published data revealing that people of color were contracting and dying from COVID-19 at higher rates than Whites. An NPR analysis of April–September 2020 data from the COVID Tracking Project found that Black people's share of COVID-19 deaths across the United States was 1.5 times greater (in some states 2.5 times greater) than their share of the U.S. population. Similarly, Hispanics and Latinos were disproportionately infected in 45 states and had a disproportionate share of the deaths in 19 states. Native American and Alaskan Native cases and deaths were disproportionally high in at least 21 states and, in some, as much as five times more than average. White non-Hispanics died at a lower rate than their share of the population in 36 states and D.C.[201]
By April 2020, closed schools affected more than 55 million students.[202]
Elections
The pandemic prompted calls from voting rights groups and some Democratic Party leaders to expand mail-in voting, while Republican leaders generally opposed the change. Some states were unable to agree on changes, resulting in lawsuits. Responding to Democratic proposals for nationwide mail-in voting as part of a coronavirus relief law, President Trump said, "you'd never have a Republican elected in this country again" despite evidence the change would not favor any particular group.[203] Trump called mail-in voting "corrupt" and said voters should be required to show up in person, even though, as reporters pointed out, he had himself voted by mail in the last Florida primary.[204] Though mail-in vote fraud is slightly higher than in-person voter fraud, both instances are rare, and mail-in voting can be made more secure by disallowing third parties to collect ballots and providing free drop-off locations or prepaid postage.[205]
High COVID-19 fatalities at the state and county level correlated with a drop in expressed support for the election of Republicans, including the reelection of President Trump, according to a study published in Science Advances that compared opinions in January–February 2020 with opinions in June 2020.[206]
Preparations made after previous outbreaks
The United States has experienced pandemics and epidemics throughout its history, including the 1918 Spanish flu, the 1957 Asian flu, and the 1968 Hong Kong flu pandemics.[207][208][209] In the most recent pandemic prior to COVID-19, the 2009 swine flu pandemic took the lives of more than 12,000 Americans and hospitalized another 270,000 over the course of approximately a year.[207]
According to the Global Health Security Index, an American-British assessment which ranks the health security capabilities in 195 countries, the U.S. was the "most prepared" nation in 2020.[210][211]
Statistics
See also
- COVID Tracking Project
- COVID-19 pandemic by country and territory
- COVID-19 pandemic in North America
- Misinformation related to the COVID-19 pandemic
- Statistics of the COVID-19 pandemic in the United States
- United States House Select Subcommittee on the Coronavirus Crisis
- United States influenza statistics by flu season
Notes
- ^ A lack of mass testing obscured the extent of the outbreak.[17]
- ^ The earliest deaths were not known to be caused by COVID-19 until April.
- ^ Examples of areas in which clusters have occurred include urban areas, nursing homes, long-term care facilities, group homes for the intellectually disabled,[33] detention centers (including prisons), meatpacking plants, churches, and navy ships.[34]
- ^ This chart only includes lab-confirmed cases and deaths. Not all states report recoveries. Data for the current day may be incomplete.
- ^ The editorial board for The Wall Street Journal suggested the world may have been "better prepared" had the PHEIC been declared a week sooner, when the virus had spread to other countries.[47]
- ^ In a news release, Sean Conley, physician to President Trump, incorrectly identified Regeneron's monoclonal antibody product as polyclonal.[93]
References
- ^ Sheikh, Knvul; Rabin, Roni Caryn (March 10, 2020). "The Coronavirus: What Scientists Have Learned So Far". The New York Times. Retrieved March 24, 2020.
- ^ "Coronavirus: the first three months as it happened". Nature. April 22, 2020. doi:10.1038/d41586-020-00154-w. PMID 32152592. S2CID 212652777.
- ^ a b c d Holshue, Michelle L.; DeBolt, Chas; Lindquist, Scott; Lofy, Kathy H.; Wiesman, John; Bruce, Hollianne; Spitters, Christopher; Ericson, Keith; Wilkerson, Sara; Tural, Ahmet; Diaz, George; Cohn, Amanda; Fox, LeAnne; Patel, Anita; Gerber, Susan I.; Kim, Lindsay; Tong, Suxiang; Lu, Xiaoyan; Lindstrom, Steve; Pallansch, Mark A.; Weldon, William C.; Biggs, Holly M.; Uyeki, Timothy M.; Pillai, Satish K. (March 5, 2020). "First Case of 2019 Novel Coronavirus in the United States". New England Journal of Medicine. 382 (10): 929–936. doi:10.1056/NEJMoa2001191. PMC 7092802. PMID 32004427.
- ^ "Second Travel-related Case of 2019 Novel Coronavirus Detected in United States". Centers for Disease Control and Prevention.
Second Travel-related Case of 2019 Novel Coronavirus Detected in United States: The patient returned to the U.S. from Wuhan on January 13, 2020
- ^ a b "Coronavirus Disease 2019 (COVID-19): Cases in U.S." Centers for Disease Control and Prevention. Updated, one day after other sources.
- ^ a b c "Coronavirus COVID-19 (2019-nCoV)" (ArcGIS). Johns Hopkins CSSE. Frequently updated.
- ^ a b "Estimated COVID-19 Infections, Symptomatic Illnesses, and Hospitalizations—United States CDC estimates that from February 2020–March 2021". Centers for Disease Control. April 14, 2021. Retrieved May 12, 2021.
- ^ "U.S. recovered COVID-19 cases". Worldometer. Frequently updated.
- ^ "Mortality Analyses". Johns Hopkins University. Retrieved December 17, 2020.
- ^ Stobbe, Mike (December 21, 2020). "US deaths in 2020 top 3 million, by far most ever counted". Associated Press. Retrieved December 22, 2020.
- ^ a b Marchione, Marilynn (February 18, 2021). "U.S. Life Expectancy Drops A Year In Pandemic, Most Since WWII". HuffPost. Retrieved February 18, 2021.
- ^ Aubrey, Allison (January 31, 2020). "Trump Declares Coronavirus A Public Health Emergency And Restricts Travel From China". NPR. Retrieved March 18, 2020.
'Foreign nationals other than immediate family of U.S. citizens and permanent residents who have traveled in China in the last 14 days will be denied entry into United States,' Azar said.
- ^ a b Robertson, Lori (April 15, 2020). "Trump's Snowballing China Travel Claim". FactCheck.org. Retrieved April 29, 2020.
... effective February 2.
- ^ Lemire, Jonathan; Miller, Zeke; Colvin, Jill; Alonso-Zaldivar, Ricardo (April 12, 2020). "Signs missed and steps slowed in Trump's pandemic response". Associated Press. Retrieved April 28, 2020.
- ^ Pilkington, Ed; McCarthy, Tom (March 28, 2020). "The missing six weeks: how Trump failed the biggest test of his life". The Guardian. ISSN 0261-3077. Retrieved March 28, 2020.
- ^ Ollstein, Alice Miranda (April 14, 2020). "Trump halts funding to World Health Organization". Politico. ISSN 2381-1595. Wikidata Q104180080. Retrieved April 28, 2020.
- ^ Whoriskey, Peter; Satija, Neena (March 16, 2020). "How U.S. coronavirus testing stalled: Flawed tests, red tape and resistance to using the millions of tests produced by the WHO". The Washington Post. Retrieved March 18, 2020.
- ^ a b Moon, Sarah (April 24, 2020). "A seemingly healthy woman's sudden death is now the first known US coronavirus-related fatality". CNN. Retrieved May 25, 2020.
- ^ "Trump signs emergency coronavirus package, injecting $8.3 billion into efforts to fight the outbreak". Business Insider. March 6, 2020.
- ^ Liptak, Kevin (March 13, 2020). "Trump declares national emergency – and denies responsibility for coronavirus testing failures". CNN. Retrieved April 18, 2020.
- ^ Biesecker, Michael (April 7, 2020). "US 'wasted' months before preparing for coronavirus pandemic". Associated Press. Retrieved April 24, 2020.
- ^ Watson, Kathryn (March 27, 2020). "Trump invokes Defense Production Act to require GM to produce ventilators". CBS News. Retrieved April 24, 2020.
- ^ Winfield Cunningham, Paige; Firozi, Paulina. "The Health 202: The Trump administration is eyeing a new testing strategy for coronavirus, Anthony Fauci says". The Washington Post.
- ^ "COVID-19 Cases Are Skyrocketing, But Deaths Are Flat – So Far. These 5 Charts Explain Why". Time. Retrieved February 25, 2021.
- ^ Maan, Anurag (October 31, 2020). "U.S. reports world record of more than 100,000 COVID-19 cases in single day". Reuters. Retrieved February 25, 2021.
- ^ Wilson, Reid (March 30, 2021). "COVID-19's fourth wave is hitting the US hard". The Hill. Retrieved March 30, 2021.
- ^ a b Haslett, Cheyenne (April 7, 2021). "UK variant has become most dominant COVID strain in US, CDC says". ABC News. Retrieved April 11, 2021.
- ^ a b Deb, Sopan; Cacciola, Scott; Stein, Marc (March 11, 2020). "Sports Leagues Bar Fans and Cancel Games Amid Coronavirus Outbreak". The New York Times. ISSN 0362-4331. Retrieved March 12, 2020.
- ^ a b Godoy, Maria (May 30, 2020). "What Do Coronavirus Racial Disparities Look Like State By State?". NPR.
- ^ a b Karson, Kendall; Scanlan, Quinn (May 22, 2020). "Black Americans and Latinos nearly 3 times as likely to know someone who died of COVID-19: Poll". ABC News.
- ^ a b "States tracking COVID-19 race and ethnicity data". American Medical Association. July 28, 2020. Retrieved July 31, 2020.
- ^ a b Tavernise, Sabrina; Oppel Jr, Richard A. (March 23, 2020). "Spit On, Yelled At, Attacked: Chinese-Americans Fear for Their Safety". The New York Times. Retrieved March 23, 2020.
- ^ "COVID-19 Infections And Deaths Are Higher Among Those With Intellectual Disabilities". NPR.
- ^ "U.S. Navy Policies Battling COVID-19 Rely Heavily On Isolation". NPR.
- ^ Margolin, Josh; Meek, James Gordon (April 8, 2020). "Intelligence report warned of coronavirus crisis as early as November: Sources". ABC News. Retrieved December 6, 2020.
- ^ Diaz, Jaclyn (December 1, 2020). "Coronavirus Was In U.S. Weeks Earlier Than Previously Known, Study Says". NPR. Retrieved December 1, 2020.
- ^ a b Farber, Madeline (January 28, 2020). "China spurned CDC offer to send a team to help contain coronavirus: US Health Secretary". Fox News.
- ^ "The Trump administration was slow to recognize coronavirus threat from Europe, CDC director admits". CNN. July 28, 2020.
- ^ "Coronavirus in Context: CDC Director Discusses Next Steps in the War Against COVID". WebMD. August 12, 2020.
- ^ "Outbreak of Pneumonia of Unknown Etiology (PUE) in Wuhan, China". CDC. January 8, 2020.
- ^ Beaumont, Peter; Borger, Julian (April 9, 2020). "WHO warned of transmission risk in January, despite Trump claims". The Guardian. Retrieved April 17, 2020.
- ^ Kuo, Lily (January 21, 2020). "China confirms human-to-human transmission of coronavirus". The Guardian. Retrieved April 19, 2020.
- ^ "CDC Emergency Operations Center Activations". CDC. January 20, 2020.
- ^ "Timeline: WHO's COVID-19 response". World Health Organization. Retrieved September 11, 2020.
- ^ Boseley, Sarah (January 30, 2020). "WHO declares coronavirus a global health emergency". The Guardian. Retrieved March 30, 2020.
- ^ Kennedy, Merrit (January 30, 2020). "WHO Declares Coronavirus Outbreak A Global Health Emergency". NPR. Retrieved April 19, 2020.
- ^ "World Health Coronavirus Disinformation". The Wall Street Journal. April 5, 2020. Archived from the original on April 9, 2020. Retrieved April 29, 2020.
- ^ Wayland, Michael (January 30, 2020). "Trump says coronavirus outbreak is 'all under control' and a 'very small problem' in US". CNBC (NBCUniversal). Retrieved September 11, 2020.
- ^ a b "US declares public health emergency from coronavirus". The Boston Globe. February 1, 2020.
- ^ Diamond, Dan (January 28, 2021). "U.S. handling of American evacuees from Wuhan increased coronavirus risks, watchdog finds". The Washington Post. Archived from the original on February 7, 2021. Retrieved February 9, 2021.
- ^ Debolt, David (April 25, 2020). "29 people had flu-like symptoms when they died in Santa Clara County. Nine tested positive for coronavirus". The Mercury News. Retrieved December 30, 2020.
- ^ Melinek, Judy (May 1, 2020). "When Did COVID-19 Arrive and Could We Have Spotted It Earlier?". MedPage Today. Retrieved May 7, 2020.
- ^ Taylor, Marisa (March 23, 2020). "Exclusive: U.S. axed CDC expert job in China months before virus outbreak". Reuters. Retrieved March 24, 2020.
- ^ Anne Schuchat (May 1, 2020). "Public Health Response to the Initiation and Spread of Pandemic COVID-19 in the United States, February 24 – April 21, 2020". MMWR. Morbidity and Mortality Weekly Report. 69 (18): 551–556. doi:10.15585/mmwr.mm6918e2. PMC 7737947. PMID 32379733.
- ^ https://nysba.org/lawrence-garbuz-new-yorks-first-known-covid-19-case-reveals-what-he-learned-about-attorney-well-being-from-the-virus/
- ^ https://www.wsj.com/articles/covid-19s-patient-zero-what-life-is-like-for-the-new-york-lawyer-11614686401
- ^ https://www.nbcnews.com/news/us-news/new-york-area-s-patient-zero-says-coronavirus-wasn-t-n1204231
- ^ Santucci J (February 27, 2020). "What we know about the White House coronavirus task force now that Mike Pence is in charge". USA Today. Retrieved November 26, 2020.
- ^ "Coronavirus Disease 2019 (COVID-19) Situation Summary". Centers for Disease Control and Prevention. March 7, 2020. Retrieved March 7, 2020.
- ^ "Coronavirus Has Become a Pandemic, W.H.O. Says". The New York Times. March 11, 2020.
- ^ "Dr. Anthony Fauci addresses COVID-19 mortality rate". C-SPAN. March 11, 2020. Retrieved September 30, 2020.
- ^ Taylor, Adam; Armus, Teo (March 11, 2020). "Live updates: As U.S. coronavirus cases top 1,000, mixed signs of recovery in China, South Korea". The Washington Post. Retrieved March 11, 2020.
- ^ Liptak, Kevin (March 16, 2020). "White House advises public to avoid groups of more than 10, asks people to stay away from bars and restaurants". CNN. Retrieved March 18, 2020.
- ^ "Global Level 4 Health Advisory – Do Not Travel". travel.state.gov.
- ^ "The 4 Key Reasons the U.S. Is So Behind on Coronavirus Testing". The Atlantic. March 15, 2020.
- ^ "They were supposed to build stages for Coachella. Now they're building coronavirus triage tents". Los Angeles Times. March 30, 2020.
- ^ "Field hospitals built around the globe as coronavirus pandemic spreads". ABC News. April 4, 2020.
- ^ "Connecticut National Guard Sets Up Temporary Hospitals Amid Coronavirus Pandemic". WVIT. April 1, 2020.
- ^ Norwood, Candace (April 3, 2020). "Most states have issued stay-at-home orders, but enforcement varies widely". PBS. Retrieved April 9, 2020.
- ^ Chan, Christine; Shumaker, Lisa; Maler, Sandra (March 28, 2020). "Confirmed coronavirus cases in U.S. reach 100,000: Reuters tally". Reuters. Retrieved March 28, 2020.
- ^ "Trump wants masks on all nursing home workers, temperature checks for all, and separate COVID-19 units". McKnight's Long-term Care News. April 3, 2020.
- ^ "U.S. coronavirus deaths top 20,000, highest in world exceeding Italy: Reuters tally". Reuters. April 11, 2020. Retrieved May 1, 2020.
- ^ "Trump Administration Announces New Nursing Homes COVID-19 Transparency Effort". Centers for Medicare & Medicaid Services. April 19, 2020.
- ^ Steve Almasy; Christina Maxouris; Nicole Chavez. "US coronavirus cases surpass 1 million and the death toll is greater than US losses in Vietnam War". CNN. Retrieved April 29, 2020.
- ^ Marc Fisher (May 27, 2020). "U.S. coronavirus death toll surpasses 100,000, exposing nation's vulnerabilities". The Washington Post. Retrieved July 23, 2020.
- ^ Antonia Noori Farzan; et al. (June 11, 2020). "U.S. surpasses 2 million coronavirus cases". The Washington Post. Retrieved July 23, 2020.
- ^ Andrew Joseph (July 21, 2020). "Actual Covid-19 case count could be 6 to 24 times higher than official estimates, CDC study shows". statnews. Stat. Retrieved January 26, 2021.
- ^ Havers, Fiona P.; Reed, Carrie; Lim, Travis; Montgomery, Joel M.; et al. (December 1, 2020). "Seroprevalence of Antibodies to SARS-CoV-2 in 10 Sites in the United States, March 23-May 12, 2020". JAMA Internal Medicine. 180 (12): 1576. doi:10.1001/jamainternmed.2020.4130. ISSN 2168-6106. PMID 32692365.
- ^ DeVille, Taylor. "Almost 17 million U.S. coronavirus cases were not detected during first half of 2020, study led by UMBC graduate finds". The Baltimore Sun. Retrieved March 19, 2021.
- ^ "Briefing on the U.S. Government's Next Steps With Regard to Withdrawal From the World Health Organization". US Department of State. September 2, 2020. Retrieved November 26, 2020.
- ^ Craft, Diane (August 8, 2020). "U.S. sets record as coronavirus cases top 5 million". Reuters. Retrieved September 25, 2020.
- ^ "COVID-19 Pandemic Planning Scenarios" (PDF). CDC. July 10, 2020. Retrieved September 29, 2020.
- ^ Durkee, Alison (July 24, 2020). "Medical Experts Tell Government: 'Shut It Down Now, And Start Over'". Forbes (Forbes Media). Retrieved July 25, 2020.
- ^ Editorial Board (August 8, 2020). "America Could Control the Pandemic by October. Let's Get to It". The New York Times. Retrieved August 8, 2020.
- ^ Rivers C, Martin E, Watson C, Schoch-Spana M, Cicero A, Inglesby T (2020). "Resetting Our Response: Changes Needed in the US Approach to COVID-19". Baltimore, MD: Johns Hopkins Center for Health Security. and Benito, Marcelino (July 23, 2020). "Back to normal by October? Dr. Hotez sends the White House a national, unified coronavirus plan". KHOU-TV. and Osterholm, Michael T.; Kashkari, Neel (August 7, 2020). "Here's How to Crush the Virus Until Vaccines Arrive". The New York Times. and Slavitt, Andy (August 4, 2020). "Joe Biden is the national reset we need on COVID-19, but he's more than 75,000 lives away". USA Today. and Branswell, Helen (August 10, 2020). "Winter is coming: Why America's window of opportunity to beat back Covid-19 is closing". STAT. Retrieved August 11, 2020.
- ^ Walker, Mark; Healy, Jack (November 6, 2020). "A Motorcycle Rally in a Pandemic? 'We Kind of Knew What Was Going to Happen'". The New York Times. Retrieved November 7, 2020.
- ^ Firestone MJ, Wienkes H, Garfin J, et al. (November 20, 2020). "COVID-19 Outbreak Associated with a 10-Day Motorcycle Rally in a Neighboring State – Minnesota, August–September 2020". MMWR Morb Mortal Wkly Rep. CDC (U.S. Department of Health and Human Services). 69 (47): 1771–1776. doi:10.15585/mmwr.mm6947e1. PMC 8022865. PMID 33237891. S2CID 227176504.
- ^ Bill Chappell (September 22, 2020). "'Enormous And Tragic': U.S. Has Lost More Than 200,000 People To COVID-19". NPR. Retrieved September 22, 2020.
- ^ Haberman, Maggie; Shear, Michael D. (October 1, 2020). "Trump Says He'll Begin 'Quarantine Process' After Hope Hicks Tests Positive for Coronavirus". The New York Times. ISSN 0362-4331. Retrieved October 3, 2020.
- ^ a b Moreno, J. Edward (October 2, 2020). "White House wanted to keep Hope Hicks's positive COVID-19 test private: report". The Hill. Retrieved October 3, 2020.
- ^ Dawsey, Josh; Itkowitz, Colby. "Trump says he and first lady have tested positive for coronavirus". The Washington Post. ISSN 0190-8286. Retrieved October 2, 2020.
- ^ Manke, Kara (October 6, 2020). "Trump's COVID-19 treatments suggest severe illness, UC Berkeley expert says". UC Berkeley News. Retrieved October 7, 2020.
- ^ "Memorandum From Trump's Doctor on COVID-19 Treatment". US News & World Report. Associated Press. October 2, 2020. Retrieved October 8, 2020. and Cohen, Jon (October 5, 2020). "Update: Here's what is known about Trump's COVID-19 treatment". Science (American Association for the Advancement of Science). Retrieved October 8, 2020.
- ^ Liptak, Kevin (October 3, 2020). "Trump taken to Walter Reed medical center and will be hospitalized 'for the next few days'". CNN. Retrieved February 24, 2021.
- ^ Eunjung Cha, Ariana and Amy Goldstein (October 5, 2020). "Prospect of Trump's early hospital discharge mystifies doctors". The Washington Post. Retrieved October 5, 2020.
- ^ Mansfield, Erin; Salman, Josh; Voyles Pulver, Dinah (October 22, 2020). "Trump's campaign made stops nationwide. Coronavirus cases surged in his wake in at least five places". USA Today. Retrieved October 26, 2020.
- ^ Facher, Lev (November 9, 2020). "Biden transition team unveils members of Covid-19 task force". Stat. Retrieved November 9, 2020.
- ^ Wang, Christine (November 9, 2020). "U.S. coronavirus cases cross 10 million as outbreaks spike across the nation". CNBC. Retrieved November 9, 2020.
- ^ "10 Million People Have Tested Positive for Coronavirus in the United States". Time. Retrieved November 9, 2020.
- ^ "Pfizer says COVID-19 vaccine is looking 90% effective". Associated Press. November 9, 2020. Retrieved November 9, 2020.
- ^ Thomas, Katie; Gelles, David; Zimmer, Carl (November 9, 2020). "Pfizer's Early Data Shows Vaccine Is More Than 90% Effective". The New York Times. ISSN 0362-4331. Retrieved November 9, 2020.
- ^ Alonso-Zalidivar, Ricardo (November 12, 2020). "Feds announce COVID-19 vaccine agreement with drug stores". Associated Press. Retrieved November 18, 2020.
- ^ O'Brien, Matt (November 23, 2020). "Many Americans flying for Thanksgiving despite CDC pleas". The Republican. Archived from the original on February 6, 2021. Retrieved November 27, 2020.
- ^ Bacon, John; Aspegren, Elinor; Hauck, Grace (December 8, 2020). "Coronavirus updates: Joe Biden pledges to deliver 100M doses in 100 days; US reaches 15M infections; Ohio-State Michigan football game off". USA Today. Retrieved December 8, 2020.
- ^ Kelleher, Suzanne Rowan. "TSA Is Seeing An Alarming Post-Thanksgiving Covid-19 Spike". Forbes. Retrieved January 5, 2021.
- ^ Yan, Holly (December 14, 2020). "Covid-19 now kills more than 1 American every minute. And the rate keeps accelerating as the death toll tops 300,000". CNN. Retrieved December 14, 2020.
- ^ Murphy, Mike (December 24, 2020). "U.S. to require all air passengers arriving from U.K. to test negative for COVID-19". MarketWatch. Retrieved December 24, 2020.
- ^ Tufekci, Zeynep (December 31, 2020). "The Mutated Virus Is a Ticking Time Bomb". The Atlantic. Retrieved January 5, 2021.
- ^ "US reports its first known case of new UK Covid variant". The Guardian. December 29, 2020. Retrieved December 30, 2020.
- ^ Cohen, Li (January 1, 2021). "U.S. surpasses 20 million cases of coronavirus on first day of 2021". CBS News. Retrieved January 1, 2021.
- ^ Lim, David (January 1, 2021). "U.S. coronavirus cases eclipse 20 million". Politico. Retrieved January 1, 2021.
- ^ Nedelman, Michael (January 6, 2021). "CDC has found more than 50 US cases of coronavirus variant first identified in UK". CNN. Retrieved January 7, 2021.
- ^ Reimann, Nicholas (January 8, 2021). "'Close To A Worst-Case Scenario' – Former CDC Director Issues 'Horrifying' Outlook For New Covid Strain". Forbes. Retrieved January 12, 2021.
- ^ Geddes, Linda; Holpuch, Amanda (January 1, 2021). "New coronavirus variant may have been in US since October". The Guardian. Retrieved February 4, 2021.
- ^ Stone, Will (January 19, 2021). "As Death Rate Accelerates, U.S. Records 400,000 Lives Lost To The Coronavirus". NPR. Retrieved January 23, 2021.
- ^ Tompkins, Lucy (January 22, 2021). "U.S. coronavirus cases top 25 million". The New York Times. Retrieved January 23, 2021.
- ^ Achenbach, Joel (January 25, 2021). "First U.S. case of highly transmissible Brazil coronavirus variant identified in Minnesota". The Washington Post. USA. Retrieved January 26, 2021.
- ^ Chappell, Bill (January 28, 2021). "South Carolina Reports 1st Known U.S. Cases Of Variant From South Africa". NPR. Retrieved January 28, 2021.
- ^ Huang, Pien (February 22, 2021). "'A Loss To The Whole Society': U.S. COVID-19 Death Toll Reaches 500,000". NPR. Retrieved February 23, 2021.
- ^ Yeung, Jessie; McKeehan, Brett. "More than 2,750 cases of coronavirus variants reported in the US". CNN. Retrieved March 5, 2021.
- ^ Sullivan, Sean. "Biden directs states to make all adults eligible for vaccine by May 1". The Washington Post. ISSN 0190-8286. Retrieved March 12, 2021.
- ^ Maan, Anurag (March 24, 2021). "U.S. COVID-19 cases top 30 million as states race to vaccinate". Reuters. Retrieved March 24, 2021.
- ^ a b Cullinane, Susannah (March 27, 2021). "Record Covid-19 vaccinations don't mean it's time to relax, officials say". Cnn.com. Retrieved March 27, 2021.
- ^ Maxouris, Christina; Yan, Holly (April 1, 2021). "More than 11,000 cases of a troubling variant reported in the US. These states have the highest numbers". Cnn.com. Retrieved April 2, 2021.
- ^ Haseltine, William A. (April 12, 2021). "An Indian SARS-CoV-2 Variant Lands In California. More Danger Ahead?". Forbes. USA. Retrieved April 20, 2021.
- ^ Maxouris, Christina (April 25, 2021). "Some parts of the US are more vulnerable to another hit by coronavirus. Here's why". CNN. Retrieved April 25, 2021.
- ^ Maxouris, Christina (April 18, 2021). "Covid-19 vaccine demand is slowing in parts of the US. Now an uphill battle starts to get more shots into arms". CNN. Retrieved April 25, 2021.
- ^ Savidge, Martin; Barajas, Angela; Waldrop, Theresa (April 23, 2021). "Vaccine hesitancy in Hinds County, Mississippi, is a story shared elsewhere". CNN. Retrieved April 25, 2021.
- ^ Nedelman, Michael (April 29, 2021). "More than a third of the US has been infected with Covid-19, CDC estimates". CNN. Retrieved April 29, 2021.
- ^ Groppe, Maureen (May 4, 2021). "Biden's new goal: 70% of adults at least partially vaccinated by July 4". USA Today. Retrieved May 4, 2021.
- ^ Sullivan, Becky (May 6, 2021). "New Study Estimates More Than 900,000 People Have Died Of COVID-19 In U.S." NPR. Retrieved May 11, 2021.
- ^ Bowden, John (May 9, 2021). "Fauci: 'No doubt' US has undercounted COVID-19 deaths". The Hill. Retrieved May 11, 2021.
- ^ Jr, Berkeley Lovelace (May 13, 2021). "CDC says fully vaccinated people don't need to wear face masks indoors or outdoors in most settings". CNBC. Retrieved May 26, 2021.
- ^ Bursztynsky, Jessica (May 16, 2021). "CDC director defends telling fully vaccinated they can go without masks amid confusion in states, cities". CNBC. Retrieved May 26, 2021.
- ^ Bobby Allyn (February 8, 2020). "China's Coronavirus Death Toll Surpasses SARS Pandemic". NPR. Retrieved August 12, 2020.
- ^ "C.D.C. and W.H.O. Offers to Help China Have Been Ignored for Weeks". The New York Times. February 7, 2020.
- ^ "Boeing donating 250,000 medical masks to battle coronavirus in China". KOMO-TV. January 29, 2020.
- ^ "The United States Announces Assistance To Combat the Novel Coronavirus". U.S. Dept. of State. February 7, 2020.
- ^ Guzman J (February 7, 2020). "US pledges $100 million to help fight coronavirus in China". The Hill. Retrieved April 11, 2020.
- ^ "Contact tracing may help avoid another lockdown. Can it work in the U.S.?". May 29, 2020.
- ^ Cunningham, Paige Winfield (June 15, 2020). "Analysis | The Health 202: U.S. isn't ready for the contact tracing it needs to stem the coronavirus". The Washington Post.
- ^ "New Contact Tracing Apps Need Access To Users' Private Data To Control Spread Of COVID-19". KPIX-TV. July 1, 2020. Retrieved July 7, 2020.
- ^ Commissioner, Office of the (October 22, 2020). "FDA Approves First Treatment for COVID-19". Food and Drug Administration. Retrieved December 1, 2020.
- ^ "Coronavirus (COVID-19) Update: FDA Authorizes Drug Combination for Treatment of COVID-19". Food and Drug Administration. November 23, 2020. Retrieved December 1, 2020.
- ^ a b "U.S. Moves to Expand Array of Drug Therapies Deployed Against Coronavirus". The Wall Street Journal. March 19, 2020.
- ^ Braun, Elisa (March 30, 2020). "In France, controversial doctor stirs coronavirus debate". Politico. Retrieved September 2, 2020.
- ^ "Coronavirus (COVID-19) Update: Daily Roundup March 30, 2020". Food and Drug Administration. March 30, 2020. Retrieved September 2, 2020.
- ^ Koppock, Kristen (March 13, 2020). "FDA Announces Two Drugs Given 'Compassionate Use' Status in Treating COVID-19". Pharmacy Times. Retrieved April 25, 2020.
- ^ Wise, Justin (March 30, 2020). "FDA issues emergency-use authorization for anti-malaria drugs amid coronavirus outbreak". The Hill. Retrieved March 30, 2020.
- ^ Research, Center for Drug Evaluation and (June 26, 2020). "FDA cautions against use of hydroxychloroquine or chloroquine for COVID-19 outside of the hospital setting or a clinical trial due to risk of heart rhythm problems". FDA – via www.fda.gov.
- ^ Gittleson, Ben; Phelps, Jordyn; Cathey, Libby (July 28, 2020). "Trump doubles down on defense of hydroxychloroquine to treat COVID-19 despite efficacy concerns". ABC News. Retrieved September 2, 2020.
- ^ "COVID-19 (coronavirus) vaccine: Get the facts". Mayo Clinic. April 22, 2020.
- ^ a b Gottlieb, Scott (April 26, 2020). "America Needs to Win the Coronavirus Vaccine Race". The Wall Street Journal.
- ^ "Guide to the Cares Act". United States Senate Committee on Small Business and Entrepreneurship. Retrieved August 15, 2020.
- ^ "Pfizer and BioNTech to Submit Emergency Use Authorization Request Today to the U.S. FDA for COVID-19 Vaccine". Pfizer (Press release). November 20, 2020. Retrieved November 20, 2020.
- ^ Park A (November 20, 2020). "Exclusive: Pfizer CEO Discusses Submitting the First COVID-19 Vaccine Clearance Request to the FDA". Time. Retrieved November 20, 2020.
- ^ "FDA Takes Key Action in Fight Against COVID-19 By Issuing Emergency Use Authorization for First COVID-19 Vaccine" (Press release). U.S. Food and Drug Administration (FDA). December 11, 2020. Retrieved December 11, 2020.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ Oliver SE, Gargano JW, Marin M, Wallace M, Curran KG, Chamberland M, et al. (December 2020). "The Advisory Committee on Immunization Practices' Interim Recommendation for Use of Pfizer–BioNTech COVID-19 Vaccine – United States, December 2020" (PDF). MMWR Morb Mortal Wkly Rep. 69 (50): 1922–1924. doi:10.15585/mmwr.mm6950e2. PMC 7745957. PMID 33332292.
- ^ "FDA Takes Additional Action in Fight Against COVID-19 By Issuing Emergency Use Authorization for Second COVID-19 Vaccine". U.S. Food and Drug Administration (FDA) (Press release). Retrieved December 18, 2020.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ Oliver SE, Gargano JW, Marin M, Wallace M, Curran KG, Chamberland M, et al. (December 2020). "The Advisory Committee on Immunization Practices' Interim Recommendation for Use of Moderna COVID-19 Vaccine – United States, December 2020" (PDF). MMWR. Morbidity and Mortality Weekly Report. 69 (5152): 1653–1656. doi:10.15585/mmwr.mm695152e1. PMID 33382675. S2CID 229945697.
- ^ "Moderna Applies for Emergency F.D.A. Approval for Its Coronavirus Vaccine". The New York Times. November 30, 2020. Retrieved November 30, 2020.
- ^ "Moderna Announces Primary Efficacy Analysis in Phase 3 COVE Study for Its COVID-19 Vaccine Candidate and Filing Today with U.S. FDA for Emergency Use Authorization". Moderna, Inc. (Press release). November 30, 2020. Retrieved November 30, 2020.
- ^ Pereira, Ivan (December 14, 2020). "US administers 1st doses of Pfizer coronavirus vaccine". ABC News. Retrieved March 6, 2021.
- ^ Aleem, Zeeshan (March 15, 2020). "A new poll shows a startling partisan divide on the dangers of the coronavirus". Vox.
- ^ Allyn, Bobby; Sprunt, Barbara (March 17, 2020). "Poll: As Coronavirus Spreads, Fewer Americans See Pandemic As A Real Threat". NPR. Retrieved March 25, 2020.
- ^ Murray, Mark (March 15, 2020). "Sixty percent believe worst is yet to come for the U.S. in coronavirus pandemic; Public attitudes about the coronavirus response are split along partisan lines in a new NBC News/Wall Street Journal poll". NBC News.
- ^ a b Weissmann, Jordan (March 17, 2020). "Democrats Are Being Much, Much More Careful About the Coronavirus Than Republicans". Slate.
- ^ Agiesta, Jennifer (May 12, 2020). "CNN Poll: Negative ratings for government handling of coronavirus persist". CNN. Retrieved May 13, 2020.
- ^ Wike, Richard; Fetterolf, Janell; Mordecai, Mara (September 15, 2020). "U.S. Image Plummets Internationally as Most Say Country Has Handled Coronavirus Badly". Pew Research Center. Retrieved September 26, 2020.
- ^ "Determination of the February 2020 Peak in US Economic Activity". June 8, 2020 – via NBER.org.
- ^ Long, Heather (April 29, 2020). "U.S. economy shrank 4.8 percent in first quarter, the biggest decline since the Great Recession". The Washington Post. Retrieved April 29, 2020.
- ^ Long, Heather (May 8, 2020). "U.S. unemployment rate soars to 14.7 percent, the worst since the Depression era". The Washington Post. Retrieved May 8, 2020.
- ^ Abelson, Reed (March 28, 2020). "Coronavirus May Add Billions to the Nation's Health Care Bill". The New York Times. Retrieved April 1, 2020.
- ^ Goolsbee, Austan (2021). "Fear, Lockdown, and Diversion: Comparing Drivers of Pandemic Economic Decline 2020". Journal of Public Economics. Becker Friedman Institute for Research in Economics. 193: 104311. doi:10.1016/j.jpubeco.2020.104311. PMC 7687454. PMID 33262548. Retrieved June 23, 2020.
- ^ Tapee, Annekan (July 31, 2020). "US economy posts its worst drop on record". CNN. Retrieved August 19, 2020.
- ^ Faelli F, Rovit S, Apps C, Johns L (September 23, 2020). "Shaping the Consumer of the Future". Bain & Company. Retrieved October 3, 2020.
- ^ Rummler, Orion (May 14, 2020). "OpenTable forecasts 25% of U.S. restaurants to shutter permanently". Axios Media. Retrieved October 4, 2020.
- ^ "43 million Americans at risk of eviction as relief programs and moratorium expire: "It's a nightmare"". CBS News. July 31, 2020.
- ^ "32% of Americans had outstanding housing payments at the beginning of August". CNBC. August 6, 2020.
- ^ "'A Homeless Pandemic' Looms As 30 Million Are At Risk Of Eviction". NPR. August 10, 2020.
- ^ Ivanova, Irina (November 27, 2020). "Nearly 19 million Americans could lose their homes when eviction limits expire Dec. 31". CBS News. Retrieved December 7, 2020.
- ^ "As Stimulus Talks Stalemate, New Report Finds 40 Million Americans Could Be At Risk Of Eviction". Forbes. August 7, 2020.
- ^ "Millions of Americans at risk of eviction after moratorium expired". Fox Business. August 12, 2020.
- ^ "Yelp data shows 60% of business closures due to the coronavirus pandemic are now permanent". CNBC. September 16, 2020.
- ^ a b U.S. Bureau of Labor Statistics (January 1, 1939). "All Employees: Total Nonfarm Payrolls". FRED, Federal Reserve Bank of St. Louis. Retrieved June 4, 2019.
- ^ U.S. Bureau of Labor Statistics (January 1, 1948). "Civilian Unemployment Rate". FRED, Federal Reserve Bank of St. Louis. Retrieved June 4, 2019.
- ^ U.S. Bureau of Labor Statistics (January 1, 1948). "Unemployment level". FRED, Federal Reserve Bank of St. Louis. Retrieved June 20, 2020.
- ^ U.S. Bureau of Labor Statistics (January 1, 1948). "Employment-Population Ration 25-54 Yrs". FRED, Federal Reserve Bank of St. Louis. Retrieved June 22, 2020.
- ^ U.S. Bureau of Labor Statistics (January 1, 1947). "Consumer Price Index for All Urban Consumers: All Items". FRED, Federal Reserve Bank of St. Louis. Retrieved June 4, 2019.
- ^ "S&P 500". fred.stlouisfed.org. June 3, 2019. Retrieved June 4, 2019.
- ^ "The Debt to the Penny and Who Holds It". treasury.gov. June 10, 2021. Retrieved June 10, 2021.
- ^ "A deadly 'checkerboard': Covid-19's new surge across rural America". The Washington Post. May 24, 2020. Retrieved December 17, 2020.
- ^ "Obesity, Race/Ethnicity, and COVID-19 – Overweight & Obesity". Centers for Disease Control and Prevention. October 28, 2020.
- ^ "Coronavirus Is Coming for Rural America". July 13, 2020 – via www.bloomberg.com.
- ^ Fang, Marina (March 16, 2021). "There Have Been Nearly 4,000 Incidents Of Anti-Asian Racism In The Last Year". HuffPost. Retrieved March 16, 2021.
- ^ Van Beusekom, Mary (September 25, 2020). "Studies spotlight COVID racial health disparities, similarities". CIDRAP – Center for Infectious Disease Research and Policy, University of Minnesota. Retrieved September 27, 2020.
- ^ "The color of coronavirus: COVID-19 deaths by race and ethnicity in the U.S." APM Research Lab: American Public Media. Retrieved September 28, 2020.
- ^ Hollie Silverman; Konstantin Toropin; Sara Sidner; Leslie Perrot. "Navajo Nation surpasses New York state for the highest Covid-19 infection rate in the US". CNN. Retrieved May 28, 2020.
- ^ Chowkwanyun, Merlin; Reed, Adolph L. (July 16, 2020). "Racial Health Disparities and Covid-19 – Caution and Context". New England Journal of Medicine. 383 (3): 201–203. doi:10.1056/NEJMp2012910. ISSN 0028-4793. PMID 32374952. S2CID 218534431.
- ^ "The COVID Racial Data Tracker". The COVID Tracking Project (The Atlantic Monthly Group). Retrieved September 28, 2020.
- ^ Wood, Daniel (September 23, 2020). "As Pandemic Deaths Add Up, Racial Disparities Persist – And In Some Cases Worsen". NPR. Retrieved September 27, 2020.
- ^ "Map: Coronavirus and School Closures". Education Week. Editorial Projects in Education. Retrieved April 23, 2020.
- ^ Panetta, Grace (March 30, 2020). "Trump baselessly claimed that expanding voting access would lead to a Republican never being elected in America again". Business Insider.
- ^ Samuels, Brett (April 7, 2020). "Trump defends his mail-in ballot after calling vote-by-mail 'corrupt'". The Hill. Archived from the original on February 26, 2021.
- ^ Parks, Miles (April 7, 2020). "Fact Check: Is Mail Ballot Fraud As Rampant As President Trump Says It Is?". NPR.
- ^ Warshaw, Christopher; Vavreck, Lynn; Baxter-King, Ryan (October 1, 2020). "Fatalities from COVID-19 are reducing Americans' support for Republicans at every level of federal office". Science Advances. 6 (44): eabd8564. doi:10.1126/sciadv.abd8564. ISSN 2375-2548. PMC 7608793. PMID 33127688.
- ^ a b Miguel, Ken (February 28, 2020). "Here's a look at some of history's worst pandemics that have killed millions". KGO-TV. Retrieved March 22, 2020.
- ^ Lileks, James (March 18, 2020). "How the news media played down the pandemics of yore, from Spanish flu to Swine flu". Star Tribune. Retrieved March 22, 2020.
- ^ Brown, Jeremy (March 3, 2020). "The Coronavirus Is No 1918 Pandemic". The Atlantic. Retrieved March 22, 2020.
- ^ "These are the countries best prepared for health emergencies". World Economic Forum. February 12, 2020.
- ^ Maizland, Lindsay; Nayeem, Thamine; Kumar, Anu (March 24, 2020). "What a Global Health Survey Found Months Before the Coronavirus Pandemic". Council on Foreign Relations.
External links
| Wikimedia Commons has media related to COVID-19 pandemic in the United States. |
| Wikiquote has quotations related to: COVID-19 pandemic in the United States |
| Scholia has a topic profile for COVID-19 pandemic in the United States. |
- U.S. Centers for Disease Control and Prevention
- The Covid Tracking Project
- Maps and Case Count
- Coverage of federal response
- Historical data
- Social-distancing visualization from Norway
- Real-time estimates and history per state
- Where people are going
- Facts from the WHO
- Interactive chart depicting spread and the role of undetected outbreaks
- Mutation tracker
Information
Article COVID-19 pandemic in the United States in English Wikipedia took following places in local popularity ranking:
- 8 place in 2020-05-03
- 13 place in 2020-05-05
- 12 place in 2020-05-06
- 13 place in 2020-05-07
- 12 place in 2020-05-08
- 15 place in 2020-05-09
- 15 place in 2020-05-10
- 14 place in 2020-05-11
- 10 place in 2020-05-12
- 8 place in 2020-05-13
- 15 place in 2020-05-14
- 11 place in 2020-05-15
- 12 place in 2020-05-16
- 21 place in 2020-05-17
- 22 place in 2020-05-18
- 16 place in 2020-05-19
- 14 place in 2020-05-20
- 16 place in 2020-05-21
- 13 place in 2020-05-22
- 20 place in 2020-05-23
- 15 place in 2020-05-24
- 17 place in 2020-05-25
- 15 place in 2020-05-26
- 25 place in 2020-05-27
- 30 place in 2020-05-29
- 33 place in 2020-06-12
- 34 place in 2020-06-13
- 35 place in 2020-06-14
- 28 place in 2020-06-15
- 22 place in 2020-06-16
- 27 place in 2020-06-17
- 36 place in 2020-06-18
- 32 place in 2020-06-19
- 28 place in 2020-06-20
- 26 place in 2020-06-21
- 16 place in 2020-06-22
- 22 place in 2020-06-23
- 17 place in 2020-06-24
- 13 place in 2020-06-25
- 14 place in 2020-06-26
- 17 place in 2020-06-27
- 22 place in 2020-06-28
- 16 place in 2020-06-29
- 18 place in 2020-06-30
- 19 place in 2020-07-01
- 15 place in 2020-07-02
- 22 place in 2020-07-03
- 34 place in 2020-07-04
- 33 place in 2020-07-05
- 25 place in 2020-07-06
- 25 place in 2020-07-07
- 16 place in 2020-07-08
- 16 place in 2020-07-09
- 19 place in 2020-07-10
- 26 place in 2020-07-11
- 24 place in 2020-07-12
- 23 place in 2020-07-13
- 30 place in 2020-07-14
- 19 place in 2020-07-15
- 18 place in 2020-07-16
- 14 place in 2020-07-17
- 24 place in 2020-07-18
- 25 place in 2020-07-19
- 23 place in 2020-07-20
- 25 place in 2020-07-21
- 13 place in 2020-07-22
- 22 place in 2020-07-23
- 22 place in 2020-07-24
- 34 place in 2020-07-25
- 37 place in 2020-07-26
- 25 place in 2020-07-27
- 18 place in 2020-07-28
- 26 place in 2020-07-29
- 25 place in 2020-07-30
- 26 place in 2020-07-31
- 33 place in 2020-08-01
- 33 place in 2020-08-02
- 22 place in 2020-08-03
- 38 place in 2020-08-04
- 46 place in 2020-08-05
- 43 place in 2020-08-06
- 34 place in 2020-08-07
- 32 place in 2020-08-08
- 39 place in 2020-08-09
- 38 place in 2020-08-10
- 45 place in 2020-08-11
- 60 place in 2020-08-12
- 53 place in 2020-08-13
- 60 place in 2020-08-14
- 74 place in 2020-08-15
- 69 place in 2020-08-16
- 47 place in 2020-08-17
- 64 place in 2020-08-18
- 80 place in 2020-08-19
- 71 place in 2020-08-20
- 64 place in 2020-08-21
- 67 place in 2020-08-22
- 100 place in 2020-08-23
- 90 place in 2020-08-24
- 72 place in 2020-08-25
- 83 place in 2020-08-26
- 86 place in 2020-08-27
- 85 place in 2020-08-28
- 98 place in 2020-08-29
- 90 place in 2020-08-30
- 82 place in 2020-08-31
- 85 place in 2020-09-01
- 80 place in 2020-09-02
- 77 place in 2020-09-03
- 74 place in 2020-09-04
- 94 place in 2020-09-06
- 84 place in 2020-09-07
- 75 place in 2020-09-08
- 84 place in 2020-09-09
- 80 place in 2020-09-10
- 91 place in 2020-09-11
- 96 place in 2020-09-13
- 83 place in 2020-09-14
- 97 place in 2020-09-15
- 95 place in 2020-09-16
- 92 place in 2020-09-17
- 96 place in 2020-09-18
- 97 place in 2020-10-03
About the page
Presented content of the Wikipedia article was extracted in 2021-06-13 based on https://en.wikipedia.org/?curid=63136490