COVID-19 pandemic
| COVID-19 pandemic | |||||||
|---|---|---|---|---|---|---|---|
 A nurse treats a COVID-19 patient in an intensive care unit aboard a US hospital ship in April 2020 | |||||||
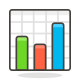
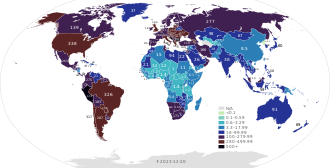 Confirmed deaths per 100,000 population
as of 9 May 2021 | |||||||
| |||||||
| Disease | Coronavirus disease 2019 (COVID-19) | ||||||
| Virus strain | Severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2) | ||||||
| Source | Likely via bats[1] | ||||||
| Location | Worldwide | ||||||
| Index case | Wuhan, Hubei, China 30°37′11″N 114°15′28″E / 30.61972°N 114.25778°E | ||||||
| Date | December 2019[2] – present (1 year, 6 months, 1 week and 5 days) | ||||||
| Confirmed cases | 175,668,875[3] | ||||||
| Suspected cases‡ | Possibly 10% of the global population, or 780 million people (WHO estimate as of early October 2020)[4] | ||||||
Deaths | 3,795,554[3] (reported) | ||||||
| ‡Suspected cases have not been confirmed by laboratory tests as being due to this strain, although some other strains may have been ruled out. | |||||||
The COVID-19 pandemic, also known as the coronavirus pandemic, is an ongoing global pandemic of coronavirus disease 2019 (COVID-19), which is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The virus was first identified in December 2019 in Wuhan, China. The World Health Organization declared a Public Health Emergency of International Concern regarding COVID-19 on 30 January 2020, and later declared a pandemic on 11 March 2020. As of 13 June 2021, more than 175 million cases have been confirmed, with more than 3.79 million confirmed deaths attributed to COVID-19, making it one of the deadliest pandemics in history.
The severity of COVID-19 symptoms is highly variable, ranging from unnoticeable to life-threatening. Severe illness is more likely in elderly COVID-19 patients, as well as those who have underlying medical conditions. COVID-19 transmits when people breathe in air contaminated by droplets and small airborne particles. The risk of breathing these in is highest when people are in close proximity, but they can be inhaled over longer distances, particularly indoors. Transmission can also occur if splashed or sprayed with contaminated fluids, in the eyes, nose or mouth, and, rarely, via contaminated surfaces. People remain contagious for up to 20 days, and can spread the virus even if they do not develop any symptoms.[5][6]
Recommended preventive measures include social distancing, wearing face masks in public, ventilation and air-filtering, hand washing, covering one's mouth when sneezing or coughing, disinfecting surfaces, and monitoring and self-isolation for people exposed or symptomatic. Several vaccines have been developed and widely distributed since December 2020. Current treatments focus on addressing symptoms, but work is underway to develop medications that inhibit the virus. Authorities worldwide have responded by implementing travel restrictions, lockdowns and quarantines, workplace hazard controls, and business closures. Numerous jurisdictions have also worked to increase testing capacity and trace contacts of the infected.[7]
The pandemic has resulted in significant global social and economic disruption, including the largest global recession since the Great Depression of the 1930s.[8] It has led to widespread supply shortages exacerbated by panic buying, agricultural disruption, and food shortages. However, there have also been decreased emissions of pollutants and greenhouse gases. Numerous educational institutions and public areas have been partially or fully closed, and many events have been cancelled or postponed. Misinformation has circulated through social media and mass media, and political tensions have been exacerbated. The pandemic has raised issues of racial and geographic discrimination, health equity, and the balance between public health imperatives and individual rights.
Epidemiology
| For country-level data, see: | |
 | |
Background
Although the exact origin of the virus is still unknown,[9] the first outbreak started in Wuhan, Hubei, China in late 2019. Many early cases of COVID-19 were linked to people who had visited the Huanan Seafood Wholesale Market in Wuhan,[10][11][12] but it is possible that human-to-human transmission was already happening before this.[13][14] On 11 February 2020, the World Health Organization (WHO) named the disease "COVID-19", which is short for coronavirus disease 2019.[15][16] The virus that caused the outbreak is known as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), a newly discovered virus closely related to bat coronaviruses,[17] pangolin coronaviruses,[18][19] and SARS-CoV.[20] The current scientific consensus is that the virus is most likely of zoonotic origin, from bats or another closely-related mammal.[21][22][23][13] Despite this, the subject has generated a significant amount of speculation and conspiracy theories,[24][14] which were amplified by rapidly growing online echo chambers.[25] Global geopolitical divisions, notably between the United States and China, have been heightened because of this issue.[26][27][28]
The earliest known person with symptoms was later discovered to have fallen ill on 1 December 2019, and that person did not have visible connections with the later wet market cluster.[29][30] However, an earlier case of infection could have occurred on 17 November.[31] Of the early cluster of cases reported that month, two-thirds were found to have a link with the market.[32][33][34] Molecular clock analysis suggests that the index case is likely to have been infected with the virus between mid-October and mid-November 2019.[35][36]
Cases
Official case counts refer to the number of people who have been tested for COVID-19 and whose test has been confirmed positive according to official protocols.[37][38] Many countries, early on, had official policies to not test those with only mild symptoms.[39][40] An analysis of the early phase of the outbreak up to 23 January estimated 86 per cent of COVID-19 infections had not been detected, and that these undocumented infections were the source for 79 per cent of documented cases.[41] Several other studies, using a variety of methods, have estimated that numbers of infections in many countries are likely to be considerably greater than the reported cases.[42][43]
On 9 April 2020, preliminary results found that 15 per cent of people tested in Gangelt, the centre of a major infection cluster in Germany, tested positive for antibodies.[44] Screening for COVID-19 in pregnant women in New York City, and blood donors in the Netherlands, has also found rates of positive antibody tests that may indicate more infections than reported.[45][46] Seroprevalence based estimates are conservative as some studies show that persons with mild symptoms do not have detectable antibodies.[47] Some results (such as the Gangelt study) have received substantial press coverage without first passing through peer review.[48]
An analysis in early 2020 of cases by age in China indicated that a relatively low proportion of cases occurred in individuals under 20.[49] It was not clear whether this was because young people were less likely to be infected, or less likely to develop serious symptoms and seek medical attention and be tested.[50] A retrospective cohort study in China found that children and adults were just as likely to be infected.[51]
Initial estimates of the basic reproduction number (R0) for COVID-19 in January were between 1.4 and 2.5,[52] but a subsequent analysis concluded that it may be about 5.7 (with a 95 per cent confidence interval of 3.8 to 8.9).[53] R0 can vary across populations and is not to be confused with the effective reproduction number (commonly just called R), which takes into account effects such as social distancing and herd immunity. By mid-May 2020, the effective R was close to or below 1.0 in many countries, meaning the spread of the disease in these areas at that time was stable or decreasing.[54]
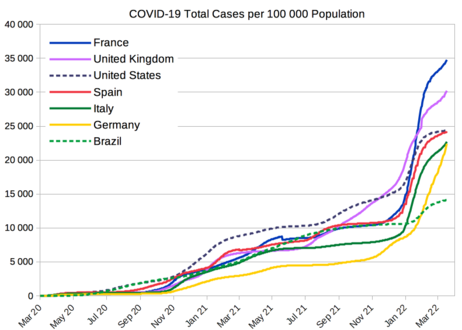
COVID-19 total cases per 100 000 population from selected countries[55]
COVID-19 active cases per 100 000 population from selected countries[55]
Deaths

Official deaths from COVID-19 generally refer to people who died after testing positive according to protocols. These counts may ignore deaths of people who die without having been tested.[56] Conversely, deaths of people who had underlying conditions may lead to over-counting.[57] Comparisons of statistics for deaths for all causes versus the seasonal average indicate excess mortality in many countries.[58][59] This may include deaths due to strained healthcare systems and bans on elective surgery.[60] The first confirmed death was in Wuhan on 9 January 2020.[61] The first reported death outside of China occurred on 1 February in the Philippines,[62] and the first reported death outside Asia was in the United States on 6 February.[63]
More than 95 per cent of the people who contract COVID-19 recover. Otherwise, the time between symptoms onset and death usually ranges from 6 to 41 days, typically about 14 days.[64] As of 13 June 2021, more than 3.79 million[3] deaths have been attributed to COVID-19. People at the greatest risk of mortality from COVID-19 tend to be those with underlying conditions, such as those with a weakened immune system, serious heart or lung problems, severe obesity, or the elderly (including individuals age 65 years or older).[65][66]
Multiple measures are used to quantify mortality.[67] These numbers vary by region and over time, influenced by testing volume, healthcare system quality, treatment options, government response,[68][69][70] time since the initial outbreak, and population characteristics, such as age, sex, and overall health.[71] Countries like Belgium include deaths from suspected cases of COVID-19, regardless of whether the person was tested, resulting in higher numbers compared to countries that include only test-confirmed cases.[72]
The death-to-case ratio reflects the number of deaths attributed to COVID-19 divided by the number of diagnosed cases within a given time interval. Based on Johns Hopkins University statistics, the global death-to-case ratio is 2.2 percent (3,795,554 deaths for 175,668,875 cases) as of 13 June 2021.[3] The number varies by region.[73]
COVID-19 deaths per 100 000 population from selected countries[55]
The official death counts have been criticised for underreporting the actual death toll, because comparisons of death rates before and during the pandemic show an increase in deaths that is not explained by COVID-19 deaths alone.[74] Using such data, estimates of the true number of deaths from COVID-19 worldwide have included a range from 7 to 13 million by The Economist, as well as over 9 million by the Institute for Health Metrics and Evaluation.[74][75]
Reporting
On 24 March 2020, the Centers for Disease Control and Prevention (CDC) of the United States, indicated the WHO had provided two codes for COVID-19: U07.1 when confirmed by laboratory testing and U07.2 for clinically or epidemiological diagnosis where laboratory confirmation is inconclusive or not available.[76][77] The CDC noted that "Because laboratory test results are not typically reported on death certificates in the U.S., [the National Center for Health Statistics (NCHS)] is not planning to implement U07.2 for mortality statistics" and that U07.1 would be used "If the death certificate reports terms such as 'probable COVID-19' or 'likely COVID-19'." The CDC also noted "It Is not likely that NCHS will follow up on these cases" and while the "underlying cause depends upon what and where conditions are reported on the death certificate, ... the rules for coding and selection of the ... cause of death are expected to result in COVID–19 being the underlying cause more often than not."[76]
On 16 April 2020, the WHO, in its formal publication of the two codes, U07.1 and U07.2, "recognized that in many countries detail as to the laboratory confirmation... will not be reported [and] recommended, for mortality purposes only, to code COVID-19 provisionally to code U07.1 unless it is stated as 'probable' or 'suspected'."[78][79] It was also noted that the WHO "does not distinguish" between infection by SARS-CoV-2 and COVID-19.[80]
Infection fatality ratio (IFR)
| Coronavirus |
|---|
 |
A crucial metric in assessing the severity of a disease is the infection fatality ratio (IFR), which is the cumulative number of deaths attributed to the disease divided by the cumulative number of infected individuals (including asymptomatic and undiagnosed infections) as measured or estimated as of a specific date.[81][82][83] Epidemiologists frequently refer to this metric as the 'infection fatality rate' to clarify that it is expressed in percentage points (not as a decimal).[84][85][86] Other published studies refer to this metric as the 'infection fatality risk'.[87][88]
In November 2020, a review article in Nature reported estimates of population-weighted IFRs for a number of countries, excluding deaths in elderly care facilities, and found a median range of 0.24% to 1.49%.[89]
In December 2020, a systematic review and meta-analysis published in the European Journal of Epidemiology estimated that population-weighted IFR was 0.5% to 1% in some countries (France, Netherlands, New Zealand, and Portugal), 1% to 2% in several other countries (Australia, England, Lithuania, and Spain), and about 2.5% in Italy; these estimates included fatalities in elderly care facilities.[90] This study also found that most of the differences in IFR across locations reflected corresponding differences in the age composition of the population and the age-specific pattern of infection rates, due to very low IFRs for children and younger adults (e.g., 0.002% at age 10 and 0.01% at age 25) and progressively higher IFRs for older adults (0.4% at age 55, 1.4% at age 65, 4.6% at age 75, and 15% at age 85).[90] These results were also highlighted in a December 2020 report issued by the World Health Organization.[91]
| Age group | IFR |
|---|---|
| 0–34 | 0.004% |
| 35–44 | 0.068% |
| 45–54 | 0.23% |
| 55–64 | 0.75% |
| 65–74 | 2.5% |
| 75–84 | 8.5% |
| 85 + | 28.3% |
An analysis of those IFR rates indicates that COVID-19 is hazardous not only for the elderly but also for middle-aged adults, for whom a fatal COVID-19 infection is two orders of magnitude more likely than the annualised risk of a fatal automobile accident and far more dangerous than seasonal influenza.[90]
Case fatality ratio (CFR)
Another metric in assessing death rate is the case fatality ratio (CFR),[a] which is deaths attributed to disease divided by individuals diagnosed to-date. This metric can be misleading because of the delay between symptom onset and death and because testing focuses on individuals with symptoms (and particularly on those manifesting more severe symptoms).[80] On 4 August, WHO indicated "at this early stage of the pandemic, most estimates of fatality ratios have been based on cases detected through surveillance and calculated using crude methods, giving rise to widely variable estimates of CFR by country – from less than 0.1% to over 25%."[82]
Disease
Signs and symptoms
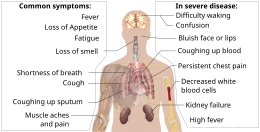
Symptoms of COVID-19 are variable, ranging from mild symptoms to severe illness.[92][93] Common symptoms include headache,[94] loss of smell[95] and taste,[96] nasal congestion and runny nose, cough, muscle pain, sore throat, fever,[97] diarrhea, and breathing difficulties.[98] People with the same infection may have different symptoms, and their symptoms may change over time. Three common clusters of symptoms have been identified: one respiratory symptom cluster with cough, sputum, shortness of breath, and fever; a musculoskeletal symptom cluster with muscle and joint pain, headache, and fatigue; a cluster of digestive symptoms with abdominal pain, vomiting, and diarrhea.[98] In people without prior ear, nose, and throat disorders, loss of taste combined with loss of smell is associated with COVID-19.[99]
Of people who show symptoms, 81% develop only mild to moderate symptoms (up to mild pneumonia), while 14% develop severe symptoms (dyspnea, hypoxia, or more than 50% lung involvement on imaging) and 5% of patients suffer critical symptoms (respiratory failure, shock, or multiorgan dysfunction).[100] At least a third of the people who are infected with the virus do not develop noticeable symptoms at any point in time.[101][102][103][104] These asymptomatic carriers tend not to get tested and can spread the disease.[104][105][106][107] Other infected people will develop symptoms later, called "pre-symptomatic", or have very mild symptoms and can also spread the virus.[107]
As is common with infections, there is a delay between the moment a person first becomes infected and the appearance of the first symptoms. The median delay for COVID-19 is four to five days.[108] Most symptomatic people experience symptoms within two to seven days after exposure, and almost all will experience at least one symptom within 12 days.[108][109]
Most people recover from the acute phase of the disease. However, some people continue to experience a range of effects for months after recovery—named long COVID—and damage to organs has been observed. Multi-year studies are underway to further investigate the long-term effects of the disease.[110]Transmission
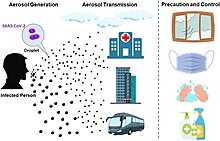
The disease is mainly transmitted via the respiratory route when people inhale droplets and particles that infected people release as they breathe, talk, cough, sneeze, or sing. Infected people are more likely to transmit COVID-19 the longer and closer they interact with others. Infection can occur over longer distances, particularly indoors.
Infectivity begins as early as three days before symptoms appear; it is at its highest once they manifest. It declines after the first week, but infected people remain contagious for up to 20 days, and can spread the disease even if they remain asymptomatic.
The size of the infectious particles range from aerosols that remain suspended in the air for long periods of time to larger droplets that remain airborne or fall to the ground. The variety in size has redefined the traditional understanding of how respiratory viruses transmit. The largest droplets of respiratory fluid do not travel far, and can be inhaled or land on mucous membranes on the eyes, nose, or mouth to infect. Aerosols are highest in concentration when people are in close proximity, which leads to easier viral transmission when people are physically close, but airborne transmission can occur at longer distances, mainly in locations that are poorly ventilated; in those conditions small particles can remain suspended in the air for minutes to hours.
The number of people generally infected by one infected person varies; with only 10 to 20% of people responsible for the diseases spread. In September 2020 it was estimated that on average one infected person will infect two or three other people. It often spreads in clusters, where infections can be traced back to an index case or geographical location. In some cases, superspreading events occur, where many people are infected by one person.Cause

SARS‑CoV‑2 belongs to the broad family of viruses known as coronaviruses.[111] It is a positive-sense single-stranded RNA (+ssRNA) virus, with a single linear RNA segment. Coronaviruses infect humans, other mammals, and avian species, including livestock and companion animals.[112] Human coronaviruses are capable of causing illnesses ranging from the common cold to more severe diseases such as Middle East respiratory syndrome (MERS, fatality rate ~34%). SARS-CoV-2 is the seventh known coronavirus to infect people, after 229E, NL63, OC43, HKU1, MERS-CoV, and the original SARS-CoV.[113]
Viral genetic sequence data can provide critical information about whether viruses separated by time and space are likely to be epidemiologically linked.[114] With a sufficient number of sequenced genomes, it is possible to reconstruct a phylogenetic tree of the mutation history of a family of viruses. By 12 January 2020, five genomes of SARS‑CoV‑2 had been isolated from Wuhan and reported by the Chinese Center for Disease Control and Prevention (CCDC) and other institutions;[115][116] the number of genomes increased to 42 by 30 January 2020.[117] A phylogenetic analysis of those samples showed they were "highly related with at most seven mutations relative to a common ancestor", implying that the first human infection occurred in November or December 2019.[117] As of 7 May 2020,[update] 4,690 SARS‑CoV‑2 genomes sampled on six continents were publicly available.[118][clarification needed]Diagnosis
Prevention

Preventive measures to reduce the chances of infection include getting vaccinated, staying at home, wearing a mask in public, avoiding crowded places, keeping distance from others, ventilating indoor spaces, managing potential exposure durations,[132] washing hands with soap and water often and for at least twenty seconds, practising good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands.[133][134]
Those diagnosed with COVID-19 or who believe they may be infected are advised by the CDC to stay home except to get medical care, call ahead before visiting a healthcare provider, wear a face mask before entering the healthcare provider's office and when in any room or vehicle with another person, cover coughs and sneezes with a tissue, regularly wash hands with soap and water and avoid sharing personal household items.[135][136]Vaccines

In Phase III trials, several COVID‑19 vaccines have demonstrated efficacy as high as 95% in preventing symptomatic COVID‑19 infections. As of April 2021[update], 16 vaccines are authorized by at least one national regulatory authority for public use: two RNA vaccines (Pfizer–BioNTech and Moderna), seven conventional inactivated vaccines (BBIBP-CorV, CoronaVac, Covaxin, WIBP-CorV, CoviVac, Minhai-Kangtai and QazVac), five viral vector vaccines (Sputnik Light, Sputnik V, Oxford–AstraZeneca, Convidecia, and Johnson & Johnson), and two protein subunit vaccines (EpiVacCorona and RBD-Dimer).[137][failed verification] In total, as of March 2021[update], 308 vaccine candidates are in various stages of development, with 73 in clinical research, including 24 in Phase I trials, 33 in Phase I–II trials, and 16 in Phase III development.[137]
Many countries have implemented phased distribution plans that prioritize those at highest risk of complications, such as the elderly, and those at high risk of exposure and transmission, such as healthcare workers.[138] Single dose interim use is under consideration in order to extend vaccination to as many people as possible until vaccine availability improves.[139][140][141][142]On 21 December 2020, the European Union approved the Pfizer BioNTech vaccine. Vaccinations began to be administered on 27 December 2020. The Moderna vaccine was authorised on 6 January 2021 and the AstraZeneca vaccine was authorised on 29 January 2021.[143]
On 4 February 2020, US Secretary of Health and Human Services Alex Azar published a notice of declaration under the Public Readiness and Emergency Preparedness Act for medical countermeasures against COVID-19, covering "any vaccine, used to treat, diagnose, cure, prevent, or mitigate COVID-19, or the transmission of SARS-CoV-2 or a virus mutating therefrom", and stating that the declaration precludes "liability claims alleging negligence by a manufacturer in creating a vaccine, or negligence by a health care provider in prescribing the wrong dose, absent willful misconduct".[144] The declaration is effective in the United States through 1 October 2024.[145] On 8 December it was reported that the AstraZeneca vaccine is about 70% effective, according to a study.[146]
Treatment
There is no specific, effective treatment or cure for coronavirus disease 2019 (COVID-19), the disease caused by the SARS-CoV-2 virus.[147][148] Thus, the cornerstone of management of COVID-19 is supportive care, which includes treatment to relieve symptoms, fluid therapy, oxygen support and prone positioning as needed, and medications or devices to support other affected vital organs.[149][150][151]
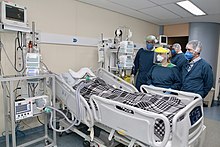
Most cases of COVID-19 are mild. In these, supportive care includes medication such as paracetamol or NSAIDs to relieve symptoms (fever,[152] body aches, cough), proper intake of fluids, rest, and nasal breathing.[153][148][154][155] Good personal hygiene and a healthy diet are also recommended.[156] The U.S. Centers for Disease Control and Prevention (CDC) recommend that those who suspect they are carrying the virus isolate themselves at home and wear a face mask.[157]
People with more severe cases may need treatment in hospital. In those with low oxygen levels, use of the glucocorticoid dexamethasone is strongly recommended, as it can reduce the risk of death.[158][159][160] Noninvasive ventilation and, ultimately, admission to an intensive care unit for mechanical ventilation may be required to support breathing.[161] Extracorporeal membrane oxygenation (ECMO) has been used to address the issue of respiratory failure, but its benefits are still under consideration.[162][163]
Several experimental treatments are being actively studied in clinical trials.[147] Others were thought to be promising early in the pandemic, such as hydroxychloroquine and lopinavir/ritonavir, but later research found them to be ineffective or even harmful.[147][164][165] Despite ongoing research, there is still not enough high-quality evidence to recommend so-called early treatment.[164][165] Nevertheless, in the United States, two monoclonal antibody-based therapies are available for early use in cases thought to be at high risk of progression to severe disease.[165] The antiviral remdesivir is available in the U.S., Canada, Australia, and several other countries, with varying restrictions; however, it is not recommended for people needing mechanical ventilation, and is discouraged altogether by the World Health Organization (WHO),[166] due to limited evidence of its efficacy.[147]
Variants
Several variants of SARS-CoV-2 have emerged that are spreading globally. The most currently prevalent, all of which share the more infectious D614G mutation, are:[167][168]
- B.1.1.7, first detected in the UK, which has spread to over 120 countries
- P.1, first detected in Brazil, which has spread to more than 50 countries
- B.1.351, first detected in South Africa, which has spread to over 80 countries
Prognosis

Mitigation
Speed and scale are key to mitigation, due to the fat-tailed nature of pandemic risk and the exponential growth of COVID-19 infections.[175] For mitigation to be effective, (a) chains of transmission must be broken as quickly as possible through screening and containment, (b) health care must be available to provide for the needs of those infected, and (c) contingencies must be in place to allow for effective rollout of (a) and (b).
Screening, containment and mitigation


Strategies in the control of an outbreak are screening, containment (or suppression), and mitigation. Screening is done with a device such as a thermometer to detect the elevated body temperature associated with fevers caused by the infection.[179] Containment is undertaken in the early stages of the outbreak and aims to trace and isolate those infected as well as introduce other measures to stop the disease from spreading. When it is no longer possible to contain the disease, efforts then move to the mitigation stage: measures are taken to slow the spread and mitigate its effects on the healthcare system and society. A combination of both containment and mitigation measures may be undertaken at the same time.[180] Suppression requires more extreme measures so as to reverse the pandemic by reducing the basic reproduction number to less than 1.[181]
Part of managing an infectious disease outbreak is trying to delay and decrease the epidemic peak, known as flattening the epidemic curve.[176] This decreases the risk of health services being overwhelmed and provides more time for vaccines and treatments to be developed.[176] Non-pharmaceutical interventions that may manage the outbreak include personal preventive measures such as hand hygiene, wearing face masks, and self-quarantine; community measures aimed at physical distancing such as closing schools and cancelling mass gathering events; community engagement to encourage acceptance and participation in such interventions; as well as environmental measures such surface cleaning.[182] Some measures, particularly those that focus on cleaning surfaces rather than preventing airborne transmission, have been criticised as hygiene theatre.[183]
More drastic actions aimed at containing the outbreak were taken in China once the severity of the outbreak became apparent, such as quarantining entire cities and imposing strict travel bans.[184] Other countries also adopted a variety of measures aimed at limiting the spread of the virus. South Korea introduced mass screening and localised quarantines and issued alerts on the movements of infected individuals. Singapore provided financial support for those infected who quarantined themselves and imposed large fines for those who failed to do so. Taiwan increased face mask production and penalised the hoarding of medical supplies.[185]
Simulations for Great Britain and the United States show that mitigation (slowing but not stopping epidemic spread) and suppression (reversing epidemic growth) have major challenges. Optimal mitigation policies might reduce peak healthcare demand by two-thirds and deaths by half, but still result in hundreds of thousands of deaths and overwhelmed health systems. Suppression can be preferred but needs to be maintained for as long as the virus is circulating in the human population (or until a vaccine becomes available), as transmission otherwise quickly rebounds when measures are relaxed. Long-term intervention to suppress the pandemic has considerable social and economic costs.[181]
Contact tracing
Contact tracing is an important method for health authorities to determine the source of infection and to prevent further transmission.[186] The use of location data from mobile phones by governments for this purpose has prompted privacy concerns, with Amnesty International and more than a hundred other organisations issuing a statement calling for limits on this kind of surveillance.[187]
Several mobile apps have been implemented or proposed for voluntary use, and as of 7 April 2020 more than a dozen expert groups were working on privacy-friendly solutions such as using Bluetooth to log a user's proximity to other cellphones.[187] (Users are alerted if they have been near someone who subsequently tests positive.)[187]
On 10 April 2020, Google and Apple jointly announced an initiative for privacy-preserving contact tracing based on Bluetooth technology and cryptography.[188][189] The system is intended to allow governments to create official privacy-preserving coronavirus tracking apps, with the eventual goal of integration of this functionality directly into the iOS and Android mobile platforms.[190] In Europe and in the U.S., Palantir Technologies is also providing COVID-19 tracking services.[191]
Health care

Increasing capacity and adapting healthcare for the needs of COVID-19 patients is described by the WHO as a fundamental outbreak response measure.[192] The ECDC and the European regional office of the WHO have issued guidelines for hospitals and primary healthcare services for shifting of resources at multiple levels, including focusing laboratory services towards COVID-19 testing, cancelling elective procedures whenever possible, separating and isolating COVID-19 positive patients, and increasing intensive care capabilities by training personnel and increasing the number of available ventilators and beds.[192][193] In addition, in an attempt to maintain physical distancing, and to protect both patients and clinicians, in some areas non-emergency healthcare services are being provided virtually.[194][195][196]
Due to capacity limitations in the standard supply chains, some manufacturers are 3D printing healthcare material such as nasal swabs and ventilator parts.[197][198] In one example, when an Italian hospital urgently required a ventilator valve, and the supplier was unable to deliver in the timescale required, a local startup received legal threats due to alleged patent infringement after reverse-engineering and printing the required hundred valves overnight.[199][200][201] On 23 April 2020, NASA reported building, in 37 days, a ventilator which is currently undergoing further testing. NASA is seeking fast-track approval.[202][203]
History
2019

Based on the retrospective analysis, starting from December 2019, the number of COVID-19 cases in Hubei gradually increased, reaching 60 by 20 December and at least 266 by 31 December.[204]
On 24 December 2019, Wuhan Central Hospital sent a bronchoalveolar lavage fluid (BAL) sample from an unresolved clinical case to sequencing company Vision Medicals.[citation needed] On 27 and 28 December, Vision Medicals informed the Wuhan Central Hospital and the Chinese CDC of the results of the test, showing a new coronavirus.[205][206] A pneumonia cluster of unknown cause was observed on 26 December and treated by the doctor Zhang Jixian in Hubei Provincial Hospital, who informed the Wuhan Jianghan CDC on 27 December.[207]
On 30 December 2019, a test report addressed to Wuhan Central Hospital, from company CapitalBio Medlab, stated that there was an erroneous positive result for SARS, causing a group of doctors at Wuhan Central Hospital to alert their colleagues and relevant hospital authorities of the result. Eight of those doctors, including Li Wenliang (who was also punished on 3 January),[208] were later admonished by the police for spreading false rumours; and another doctor, Ai Fen, was reprimanded by her superiors for raising the alarm.[209] That evening, the Wuhan Municipal Health Commission issued a notice to various medical institutions about "the treatment of pneumonia of unknown cause".[210] The next day, the Wuhan Municipal Health Commission made the first public announcement of a pneumonia outbreak of unknown cause, confirming 27 cases[211][212][213]—enough to trigger an investigation.[214]
The following day, on 31 December, the WHO office in China was informed of cases of pneumonia of unknown cause in Wuhan.[215][211] An investigation was launched at the start of January 2020.[214]
According to official Chinese sources, the early cases were mostly linked to the Huanan Seafood Wholesale Market, which also sold live animals.[216] However, in May 2020, George Gao, the director of the Chinese Center for Disease Control and Prevention, said animal samples collected from the seafood market had tested negative for the virus, indicating the market was not the source of the initial outbreak.[217] In March 2021, the WHO published their report on the potential zoonotic source of the virus. The WHO concluded that human spillover via an intermediate animal host was the most likely explanation, with direct spillover from bats next most likely and introduction through the food supply chain as another possible explanation.[218][12]
2020

From 31 December 2019 to 3 January 2020, a total of 44 cases of "pneumonia of unknown causes" were reported to WHO by the Chinese authorities.
On 11 January, WHO received further information from the Chinese National Health Commission that the outbreak is associated with exposures in one seafood market in Wuhan, and that the Chinese authorities had identified a new type of coronavirus, which was isolated on 7 January.[215]
During the early stages of the outbreak, the number of cases doubled approximately every seven and a half days.[219] In early and mid-January, the virus spread to other Chinese provinces, helped by the Chinese New Year migration and Wuhan being a transport hub and major rail interchange.[220] On 10 January, the SARS-CoV-2 genetic sequence data was shared through GISAID.[221] On 20 January, China reported nearly 140 new cases in one day, including two people in Beijing and one in Shenzhen.[222] A retrospective official study published in March found that 6,174 people had already developed symptoms by 20 January (most of them would be diagnosed later)[223] and more may have been infected.[224] A report in The Lancet on 24 January indicated human transmission, strongly recommended personal protective equipment for health workers, and said testing for the virus was essential due to its "pandemic potential".[32][225] On 31 January The Lancet would publish the first modelling study explicitly warning of inevitable "independent self-sustaining outbreaks in major cities globally" and calling for "large-scale public health interventions."[226]
On 30 January, with 7,818 confirmed cases across 19 countries, the WHO declared the COVID-19 outbreak a Public Health Emergency of International Concern (PHEIC),[227][228] and then a pandemic on 11 March 2020[229][230] as Italy, Iran, South Korea, and Japan reported increasing numbers of cases.

On 31 January, Italy had its first confirmed cases, two tourists from China.[231] On 19 March, Italy overtook China as the country with the most reported deaths.[232] By 26 March, the United States had overtaken China and Italy with the highest number of confirmed cases in the world.[233] Research on SARS-CoV-2 genomes indicates the majority of COVID-19 cases in New York came from European travellers, rather than directly from China or any other Asian country.[234] Retesting of prior samples found a person in France who had the virus on 27 December 2019[235][236] and a person in the United States who died from the disease on 6 February 2020.[237]
On 11 June, after 55 days without a locally transmitted case being officially reported,[238] the city of Beijing reported a single COVID-19 case, followed by two more cases on 12 June.[239] As of 15 June 2020, 79 cases were officially confirmed.[240] Most of these patients went to Xinfadi Wholesale Market.[238][241]
On 29 June, WHO warned that the spread of the virus was still accelerating as countries reopened their economies, despite many countries having made progress in slowing down the spread.[242]
On 15 July, one COVID-19 case was officially reported in Dalian in more than three months. The patient did not travel outside the city in the 14 days before developing symptoms, nor did he have contact with people from "areas of attention."[243]
In October, the WHO stated, at a special meeting of WHO leaders, that one in ten people around the world may have been infected with COVID-19. At the time, that translated to 780 million people being infected, while only 35 million infections had been confirmed.[244]
In early November, Denmark reported on an outbreak of a unique mutated variant being transmitted to humans from minks in its North Jutland Region. All twelve human cases of the mutated variant were identified in September 2020. The WHO released a report saying the variant "had a combination of mutations or changes that have not been previously observed."[245] In response, Prime Minister Mette Frederiksen ordered for the country – the world's largest producer of mink fur – to cull its mink population by as many as 17 million.[246]
On 9 November, Pfizer released their trial results for a candidate vaccine, showing that it is 90% effective against the virus.[247] Later that day, Novavax entered an FDA Fast Track application for their vaccine.[248] Virologist and U.S. National Institute of Allergy and Infectious Diseases director Anthony Fauci indicated that the Pfizer vaccine targets the spike protein used to infect cells by the virus. Some issues left to be answered are how long the vaccine offers protection, and if it offers the same level of protection to all ages. Initial doses will likely go to healthcare workers on the front lines.[249]
On 9 November 2020 the United States surpassed 10 million confirmed cases of COVID-19, making it the country with the most cases worldwide by a large margin.[250]
It was reported on 27 November, that a publication released by the Centers for Disease Control and Prevention indicated that the current numbers of viral infection are via confirmed laboratory test only. However, the true number could be about eight times the reported number; the report further indicated that the true number of virus infected cases could be around 100 million in the U.S.[251][252]
On 14 December, Public Health England reported a new variant had been discovered in the South East of England, predominantly in Kent. The variant, named Variant of Concern 202012/01, showed changes to the spike protein which could make the virus more infectious. As of 13 December, there were 1,108 cases identified.[253] Many countries halted all flights from the UK;[254] France-bound Eurotunnel service was suspended and ferries carrying passengers and accompanied freight were cancelled as the French border closed to people on 20 December.[255]
2021
On 2 January, VOC-202012/01, a variant of SARS-CoV-2 first discovered in the UK, had been identified in 33 countries around the world, including Pakistan, South Korea, Switzerland, Taiwan, Norway, Italy, Japan, Lebanon, India, Canada, Denmark, France, Germany, Iceland, and China.[256]
On 6 January, the P.1 variant was first identified in Japanese travellers who had just returned from Brazil.[257]
On 12 January, it was reported that a team of scientists from the World Health Organization would arrive in Wuhan on the 14th of the month; this is to ascertain the origin of SARS-CoV-2 and determine what were the intermediate hosts between the original reservoir and humans.[258] On the following day, two of the WHO members were barred from entering China because, according to the country, antibodies for the virus were detected in both.[259]
On 29 January, it was reported that the Novavax vaccine was only 49% effective against the 501.V2 variant in a clinical trial in South Africa.[260][261] The China COVID-19 vaccine CoronaVac indicated 50.4% effectivity in a Brazil clinical trial.[262]
On 12 March, it was reported that several countries including Thailand, Denmark, Bulgaria, Norway, and Iceland had stopped using the Oxford-AstraZeneca COVID-19 vaccine due to what was being called severe blood clotting problems, a Cerebral venous sinus thrombosis (CVST). Additionally, Austria halted the use of one batch of the aforementioned vaccine as well.[263] On 20 March, the WHO and European Medicines Agency found no link between thrombus (a blood clot of clinical importance), leading several European countries to resume administering the AstraZeneca vaccine.[264]
On 29 March, it was reported that the U.S. government was planning to introduce COVID-19 vaccination 'passports' to allow those who have been vaccinated the ability to board aeroplanes, cruise ships as well as other activities.[265]
As of 13 June 2021, more than 175 million cases have been reported worldwide due to COVID-19; more than 3.79 million have died.[3]
National responses

Due to the pandemic in Europe, many countries in the Schengen Area have restricted free movement and set up border controls.[266] National reactions have included containment measures such as quarantines and curfews (known as stay-at-home orders, shelter-in-place orders, or lockdowns).[267] The WHO's recommendation on curfews and lockdowns is that they should be short-term measures to reorganise, regroup, rebalance resources, and protect health workers who are exhausted. To achieve a balance between restrictions and normal life, the long-term responses to the pandemic should consist of strict personal hygiene, effective contact tracing, and isolating when ill.[268]
By 26 March 2020, 1.7 billion people worldwide were under some form of lockdown,[269] which increased to 3.9 billion people by the first week of April—more than half the world's population.[270][271]
By late April 2020, around 300 million people were under lockdown in nations of Europe, including but not limited to Italy, Spain, France, and the United Kingdom, while around 200 million people were under lockdown in Latin America.[272] Nearly 300 million people, or about 90 per cent of the population, were under some form of lockdown in the United States,[273] around 100 million people in the Philippines,[272] about 59 million people in South Africa,[274] and 1.3 billion people have been under lockdown in India.[275][276]
Asia
As of 30 April 2020,[update][277] cases have been reported in all Asian countries except for Turkmenistan and North Korea, although these countries likely also have cases.[278][279] Despite being the first area of the world hit by the outbreak, the early wide-scale response of some Asian states, particularly Bhutan,[280] Singapore,[281][282] Taiwan[283] and Vietnam[284] has allowed them to fare comparatively well. China is criticised for initially minimising the severity of the outbreak, but the delayed wide-scale response has largely contained the disease since March 2020.[285][286][287][288]
In Japan, the pandemic has been believed to have caused direct side effects in regards to mental health. According to the report by the country's National Police Agency, suicides had increased to 2,153 in October. Experts also state that the pandemic has worsened mental health issues due to lockdowns and isolation from family members, among other issues.[289]
China
As of 14 July 2020, there are 83,545 cases confirmed in China— excluding 114 asymptomatic cases, 62 of which were imported, under medical observation; asymptomatic cases have not been reported prior to 31 March 2020—with 4,634 deaths and 78,509 recoveries,[290] meaning there are only 402 cases. Hubei has the most cases, followed by Xinjiang.[291] By March 2020, COVID-19 infections have largely been put under control in China,[285] with minor outbreaks since.[292] It was reported on 25 November, that some 1 million people in the country of China have been vaccinated according to China's state council; the vaccines against COVID-19 come from Sinopharm which makes two and one produced by Sinovac.[293]
India

The first case of COVID-19 in India was reported on 30 January 2020. India ordered a nationwide lockdown for the entire population starting 24 March 2020,[294] with a phased unlock beginning 1 June 2020. Six cities account for around half of all reported cases in the country—Mumbai, Delhi, Ahmedabad, Chennai, Pune and Kolkata.[295] On 10 June 2020, India's recoveries exceeded active cases for the first time.[296]
On 30 August 2020, India surpassed the US record for the most cases in a single day, with more than 78,000 cases,[297] and set a new record on 16 September 2020, with almost 98,000 cases reported that day.[298] As of 30 August 2020, India's case fatality rate is relatively low at 2.3%, against the global 4.7%.[299][needs update]
As of September 2020, India had the largest number of confirmed cases in Asia;[300] and the second-highest number of confirmed cases in the world,[301] behind the United States,[302] with the number of total confirmed cases breaching the 100,000 mark on 19 May 2020,[303] 1,000,000 on 16 July 2020,[304] and 5,000,000 confirmed cases on 16 September 2020.[305]
On 19 December 2020, India crossed the total number of 10,000,000 confirmed cases but with a slow pace.[306]
The Indian Ministry of Science initiated a mathematical simulation of the pandemic, the so-called "Indian Supermodel", which correctly predicted the decrease of active cases starting in September 2020.[307][5][308][309][310]
A second wave hit India in April 2021, placing healthcare services under severe strain.[311] By late April, the government was reporting over 300,000 new infections and 2,000 deaths per day, with concerns of undercounting.[312]
Iran

Iran reported its first confirmed cases of SARS-CoV-2 infections on 19 February 2020 in Qom, where, according to the Ministry of Health and Medical Education, two people had died that day.[314][315] Early measures announced by the government included the cancellation of concerts and other cultural events,[316] sporting events,[317] Friday prayers,[318] and closures of universities, higher education institutions, and schools.[319] Iran allocated 5 trillion rials (equivalent to US$120,000,000) to combat the virus.[320] President Hassan Rouhani said on 26 February 2020 there were no plans to quarantine areas affected by the outbreak, and only individuals would be quarantined.[321] Plans to limit travel between cities were announced in March 2020,[322] although heavy traffic between cities ahead of the Persian New Year Nowruz continued.[323] Shia shrines in Qom remained open to pilgrims until 16 March.[324][325]
Iran became a centre of the spread of the virus after China in February 2020.[326][327] More than ten countries had traced their cases back to Iran by 28 February, indicating the outbreak may have been more severe than the 388 cases reported by the Iranian government by that date.[327][328] The Iranian Parliament was shut down, with 23 of its 290 members reported to have had tested positive for the virus on 3 March 2020.[329] On 15 March 2020, the Iranian government reported a hundred deaths in a single day, the most recorded in the country since the outbreak began.[330] At least twelve sitting or former Iranian politicians and government officials had died from the disease by 17 March 2020.[331] By 23 March 2020, Iran was experiencing fifty new cases every hour and one new death every ten minutes due to COVID-19.[332] According to a WHO official, there may be five times more cases in Iran than what is being reported. It is also suggested that U.S. sanctions on Iran may be affecting the country's financial ability to respond to the viral outbreak.[333]
On 20 April 2020, Iran reopened shopping malls and other shopping areas across the country.[334] After reaching a low in new cases in early May, a new peak was reported on 4 June 2020, raising fear of a second wave.[335] On 18 July 2020, President Rouhani estimated that 25 million Iranians had already become infected, which is considerably higher than the official count.[336] Leaked data suggest that 42,000 people had died with COVID-19 symptoms by 20 July 2020, nearly tripling the 14,405 officially reported by that date.[337]
South Korea
COVID-19 was confirmed to have spread to South Korea on 20 January 2020 from China. The nation's health agency reported a significant increase in confirmed cases on 20 February,[338] largely attributed to a gathering in Daegu of the Shincheonji Church of Jesus.[338][339] Shincheonji devotees visiting Daegu from Wuhan were suspected to be the origin of the outbreak.[340][341] By 22 February[update], among 9,336 followers of the church, 1,261 or about 13 per cent reported symptoms.[342] South Korea declared the highest level of alert on 23 February 2020.[343] On 29 February, more than 3,150 confirmed cases were reported.[344] All South Korean military bases were quarantined after tests showed three soldiers had the virus.[340] Airline schedules were also changed.[345][346]
South Korea introduced what was considered the largest and best-organised programme in the world to screen the population for the virus, isolate any infected people, and trace and quarantine those who contacted them.[347][348] Screening methods included mandatory self-reporting of symptoms by new international arrivals through mobile application,[349] drive-through testing for the virus with the results available the next day,[350] and increasing testing capability to allow up to 20,000 people to be tested every day.[351] Despite some early criticisms of President Moon Jae-in's response to the crisis,[352] South Korea's programme is considered a success in controlling the outbreak without quarantining entire cities.[347][353][354]
On 23 March, it was reported that South Korea had the lowest one-day case total in four weeks.[351] On 29 March, it was reported that beginning 1 April all new overseas arrivals will be quarantined for two weeks.[355] Per media reports on 1 April, South Korea has received requests for virus testing assistance from 121 different countries.[356] Persistent local groups of infections in the greater Seoul area continued to be found, which led to Korea's CDC director saying in June that the country had entered the second wave of infections,[357] although a WHO official disagreed with that assessment.[358]
Europe
By 13 March 2020, when the number of reported new cases of COVID-19 became greater than those in China, the World Health Organization (WHO) began to consider Europe the active centre of the COVID-19 pandemic.[359][360] By 22 May 2020, the WHO said the epicenter had shifted to South America.[361]
By 17 March 2020, all countries within Europe had a confirmed case of COVID-19, with Montenegro being the last European country to report at least one case.[362] At least one death has been reported in all European countries, apart from the Vatican City.
By 18 March 2020, more than 250 million people were in lockdown in Europe.[363]
On 24 May 2020, 68 days since its first recorded case, Montenegro became the first COVID-free country in Europe,[364][365] but this situation lasted only 44 days before a newly imported case was identified there.[366] European countries with the highest number of confirmed COVID-19 cases are Russia, the United Kingdom, France, Spain, and Italy.[367]On 21 August, it was reported the COVID-19 cases were climbing among younger individuals across Europe.[368] On 21 November, it was reported by the Voice of America that Europe is the worst hit area by the COVID-19 virus, with numbers exceeding 15 million cases.[369]
France
Although it was originally thought the pandemic reached France on 24 January 2020, when the first COVID-19 case in Europe was confirmed in Bordeaux, it was later discovered that a person near Paris had tested positive for the virus on 27 December 2019 after retesting old samples.[235][236] A key event in the spread of the disease in the country was the annual assembly of the Christian Open Door Church between 17 and 24 February in Mulhouse, which was attended by about 2,500 people, at least half of whom are believed to have contracted the virus.[370][371]
On 13 March, Prime Minister Édouard Philippe ordered the closure of all non-essential public places,[372] and on 16 March, French President Emmanuel Macron announced mandatory home confinement, a policy which was extended at least until 11 May.[373][374][375] As of 14 September[update], France has reported more than 402,000 confirmed cases, 30,000 deaths, and 90,000 recoveries,[376] ranking fourth in number of confirmed cases.[377] In April, there were riots in some Paris suburbs.[378] On 18 May, it was reported that schools in France had to close again after reopening, due to COVID-19 case flare-ups.[379]
On 12 November, it was reported that France had become the worst-hit country by the COVID-19 pandemic, in all of Europe, in the process surpassing Russia. The new total of confirmed cases was more than 1.8 million and counting; additionally it was indicated by the French government that the current national lockdown would remain in place.[380]
Italy

The outbreak was confirmed to have spread to Italy on 31 January 2020, when two Chinese tourists tested positive for SARS-CoV-2 in Rome.[231] Cases began to rise sharply, which prompted the Italian government to suspend all flights to and from China and declare a state of emergency.[381] An unassociated cluster of COVID-19 cases was later detected, starting with 16 confirmed cases in Lombardy on 21 February 2020.[382]
On 22 February 2020, the Council of Ministers announced a new decree-law to contain the outbreak, including quarantining more than 50,000 people from eleven different municipalities in northern Italy.[383] Prime Minister Giuseppe Conte said, "In the outbreak areas, entry and exit will not be provided. Suspension of work activities and sports events has already been ordered in those areas."[384][385]
On 4 March 2020, the Italian government ordered the full closure of all schools and universities nationwide as Italy reached a hundred deaths. All major sporting events were to be held behind closed doors until April,[386] but on 9 March, all sport was suspended completely for at least one month.[387] On 11 March 2020, Prime Minister Conte ordered stoppage of nearly all commercial activity except supermarkets and pharmacies.[388][389]
On 6 March 2020, the Italian College of Anaesthesia, Analgesia, Resuscitation and Intensive Care (SIAARTI) published medical ethics recommendations regarding triage protocols.[390][391][392] On 19 March 2020, Italy overtook China as the country with the most COVID-19-related deaths in the world after reporting 3,405 fatalities from the pandemic.[393][394] On 22 March 2020, it was reported that Russia had sent nine military planes with medical equipment to Italy.[395] As of 28 March[update], there were 3,532,057 confirmed cases, 107,933 deaths, and 2,850,889 recoveries in Italy, with a large number of those cases occurring in the Lombardy region.[3] A CNN report indicated that the combination of Italy's large elderly population and inability to test all who have the virus to date may be contributing to the high fatality rate.[396] On 19 April 2020, it was reported that the country had its lowest deaths at 433 in seven days and some businesses were asking for a loosening of restrictions after six weeks of lockdown.[397] On 13 October 2020, the Italian government again issued restrictive rules to contain a rise in infections.[398]
On 11 November, it was reported that Silvestro Scotti, president of the Italian Federation of General Practitioners indicated that all of Italy should come under restrictions due to the spread of COVID-19. A couple of days prior Filippo Anelli, president of the National Federation of Doctor's Guilds (FNOMCEO) asked for a complete lockdown of the peninsular nation due to the pandemic.[399] On the 10th, a day before, Italy surpassed 1 million confirmed COVID-19 cases.[400] On 23 November, it was reported that the second wave of the virus has caused some hospitals in Italy to stop accepting patients.[401]
Spain

The virus was first confirmed to have spread to Spain on 31 January 2020, when a German tourist tested positive for SARS-CoV-2 in La Gomera, Canary Islands.[402] Post-hoc genetic analysis has shown that at least 15 strains of the virus had been imported, and community transmission began by mid-February.[403] By 13 March, cases had been confirmed in all 50 provinces of the country.
A lockdown was imposed on 14 March 2020.[404] On 29 March, it was announced that, beginning the following day, all non-essential workers were ordered to remain at home for the next 14 days.[405] By late March, the Community of Madrid has recorded the most cases and deaths in the country. Medical professionals and those who live in retirement homes have experienced especially high infection rates.[406] On 25 March, the official death toll in Spain surpassed that of mainland China.[407] On 2 April, 950 people died of the virus in a 24-hour period—at the time, the most by any country in a single day.[408] On 17 May, the daily death toll announced by the Spanish government fell below 100 for the first time,[409] and 1 June was the first day without deaths by COVID-19.[410] The state of alarm ended on 21 June.[411] However, the number of cases increased again in July in a number of cities including Barcelona, Zaragoza and Madrid, which led to reimposition of some restrictions but no national lockdown.[412][413][414][415]
Studies have suggested that the number of infections and deaths may have been underestimated due to lack of testing and reporting, and many people with only mild or no symptoms were not tested.[416][417] Reports in May suggested that, based on a sample of more than 63,000 people, the number of infections may be ten times higher than the number of confirmed cases by that date, and Madrid and several provinces of Castilla–La Mancha and Castile and León were the most affected areas with a percentage of infection greater than 10%.[418][419] There may also be as many as 15,815 more deaths according to the Spanish Ministry of Health monitoring system on daily excess mortality (Sistema de Monitorización de la Mortalidad Diaria – MoMo).[420] On 6 July 2020, the results of a Government of Spain nationwide seroprevalence study showed that about two million people, or 5.2% of the population, could have been infected during the pandemic.[421][422] Spain was the second country in Europe (behind Russia) to record half a million cases.[423] On 21 October, Spain passed 1 million COVID-19 cases, with 1,005,295 infections and 34,366 deaths reported, a third of which occurred in Madrid.[424]Sweden
Sweden differed from most other European countries in that it mostly remained open.[425] Per the Swedish Constitution, the Public Health Agency of Sweden has autonomy which prevents political interference and the agency's policy favoured forgoing a lockdown. The Swedish strategy focused on measures that could be put in place over a longer period of time, based on the assumption that the virus would start spreading again after a shorter lockdown.[426][427] The New York Times said that, as of May 2020, the outbreak had been far deadlier there but the economic impact had been reduced as Swedes have continued to go to work, restaurants, and shopping.[425][428] On 19 May, it was reported that the country had in the week of 12–19 May the highest per capita deaths in Europe, 6.25 deaths per million per day.[429] In the end of June, Sweden no longer had excess mortality.[430]
United Kingdom

Devolution in the United Kingdom meant that each of the four countries of the UK had its own different response to COVID-19, and the UK government, on behalf of England, moved quicker to lift restrictions.[431] The UK government started enforcing social distancing and quarantine measures on 18 March 2020[432][433] and was criticised for a perceived lack of intensity in its response to concerns faced by the public.[434][435] On 16 March, Prime Minister Boris Johnson advised against non-essential travel and social contact, suggesting people work from home and avoid venues such as pubs, restaurants, and theatres.[436][437] On 20 March, the government ordered all leisure establishments to close as soon as possible,[438] and promised to prevent unemployment.[439] On 23 March, Johnson banned gatherings of multiple people and restricting non-essential travel and outdoor activity. Unlike previous measures, these restrictions were enforceable by police through fines and dispersal of gatherings. Most non-essential businesses were ordered to close.[440]
On 24 April, it was reported that a promising vaccine trial had begun in England; the government pledged more than £50 million towards research.[441] A number of temporary critical care hospitals were built.[442] The first operating was the 4,000-bed NHS Nightingale Hospital London, constructed for over nine days.[443] On 4 May, it was announced that it would be placed on standby and remaining patients transferred to other facilities;[444] 51 patients had been treated in the first three weeks.[445]
On 16 April, it was reported that the UK would have first access to the Oxford vaccine, due to a prior contract; should the trial be successful, some 30 million doses in the UK would be available.[446]
On 2 December, the UK became the first Western country to approve the Pfizer vaccine against the COVID-19 virus; 800,000 doses would be immediately available for use.[447] It was reported on 5 December, that the United Kingdom would begin vaccination against the virus on 8 December, less than a week after having been approved.[448] On 9 December, MHRA stated that any individual with a significant allergic reaction to a vaccine, such as an anaphylactoid reaction, should not take the Pfizer vaccine for COVID-19 protection.[449][450]
North America
The first cases in North America were reported in the United States on the 23 January 2020. Cases were reported in all North American countries after Saint Kitts and Nevis confirmed a case on 25 March, and in all North American territories after Bonaire confirmed a case on 16 April.[451]
As of 24 May 2021, Canada has reported 1,361,564 cases and 25,265 deaths,[452] while Mexico has reported 2,396,604 cases and 221,647 deaths.[453] The most cases by state is California with 3,778,711 cases and 62,945 deaths as of 24 May 2021.[454]United States
More than 33.4 million confirmed cases have been reported in the United States since January 2020, resulting in more than 599,000 deaths, the most of any country, and the twentieth-highest per capita worldwide.[455][456] As many infections go undetected, the Centers for Disease Control estimates that as of March 2021, there have been a total 114.6 million infections in the United States.[457] The U.S. has about one-fifth of the world's confirmed cases and deaths. COVID-19 became the third-leading cause of death in the U.S. in 2020, behind heart disease and cancer.[458] U.S. life expectancy dropped from 78.8 years in 2019 to 77.8 years in the first half of 2020.[459]
The first American case was reported on January 20, and President Donald Trump declared the U.S. outbreak a public health emergency on January 31. Restrictions were placed on flights arriving from China,[460][461] but the initial U.S. response to the pandemic was otherwise slow, in terms of preparing the healthcare system, stopping other travel, and testing.[462][463][464][b] Meanwhile, Trump remained optimistic and was accused by his critics of underestimating the severity of the virus.
The first known American deaths occurred in February.[466][c] On March 6, 2020, Trump signed the Coronavirus Preparedness and Response Supplemental Appropriations Act, which provided $8.3 billion in emergency funding for federal agencies to respond to the outbreak.[467] On March 13, President Trump declared a national emergency.[468] In mid-March, the Trump administration started to purchase large quantities of medical equipment,[469] and in late March, it invoked the Defense Production Act of 1950 to direct industries to produce medical equipment.[470] By April 17, the federal government approved disaster declarations for all states and territories. By mid-April, cases had been confirmed in all fifty U.S. states, and by November in all inhabited U.S. territories.South America
The pandemic was confirmed to have reached South America on 26 February 2020 when Brazil confirmed a case in São Paulo.[471] By 3 April, all countries and territories in South America had recorded at least one case.[472]
On 13 May 2020, it was reported that Latin America and the Caribbean had reported over 400,000 cases of COVID-19 infection with, 23,091 deaths. On 22 May 2020, citing the rapid increase of infections in Brazil, the WHO declared South America the epicentre of the pandemic.[473][474]
As of 19 May 2021, South America had recorded 27,018,922 confirmed cases and 735,683 deaths from COVID-19. Due to a shortage of testing and medical facilities, it is believed that the outbreak is far larger than the official numbers show.[475]Brazil

On 20 May, it was reported that Brazil had a record 1,179 deaths in a single day, for a total of almost 18,000 fatalities. With a total number of almost 272,000 cases, Brazil became the country with the third-highest number of cases, following Russia and the United States.[476] On 25 May, Brazil exceeded the number of reported cases in Russia when they reported that 11,687 new cases had been confirmed over the previous 24 hours, bringing the total number to over 374,800, with more than 23,400 deaths. President Jair Bolsonaro has created controversy by referring to the virus as a "little flu" and frequently speaking out against preventive measures such as lockdowns and quarantines. His attitude towards the outbreak has been likened to that of former U.S. President Trump, with Bolsonaro being called the "Trump of the Tropics".[477] Bolsonaro later tested positive for the virus.[478]
In June 2020, the government of Brazil attempted to conceal the actual figures of the COVID-19 active cases and deaths, as it stopped publishing the total number of infections and deaths. On 5 June, Brazil's health ministry took down the official website reflecting the total numbers of infections and deaths. The website was live on 6 June, with only the number of infections of the previous 24 hours. The last official numbers reported about 615,000 infections and over 34,000 deaths.[479] On 15 June, it was reported that the worldwide cases had jumped from seven to eight million in one week, citing Latin America, specifically Brazil as one of the countries where cases are surging, in this case, towards 1 million cases.[480] Brazil briefly paused Phase III trials for the Coronavac COVID-19 vaccine on 10 November after the suicide of a volunteer before resuming on 11 November.[481]
By early 2021, the death toll had climbed to 231,534. The total number of cases on 7 February exceeded 9.5 million. The only countries with worse outbreaks were India and the United States.[482]
Africa

The pandemic was confirmed to have spread to Africa on 14 February 2020, with the first confirmed case announced in Egypt.[483][484] The first confirmed case in sub-Saharan Africa was announced in Nigeria at the end of February.[485] Within three months, the virus had spread throughout the continent, as Lesotho, the last African sovereign state to have remained free of the virus, reported a case on 13 May 2020.[486][487] By 26 May, it appeared that most African countries were experiencing community transmission, although testing capacity was limited.[488] Most of the identified imported cases arrived from Europe and the United States rather than from China where the virus originated.[489]
In early June 2021, Africa faced a thrd wave of Covid infections with cases rising in 14 countries.[490]
It is believed that there is widespread under-reporting in many African countries with less developed healthcare systems.[491] According to the autumn 2020 seroprevalence study in Juba in South Sudan, less than 1% of infected were actually reported.[492]Oceania
Antarctica
International responses
The COVID-19 pandemic shook the world's economy, with especially severe economic damage in the United States, Europe, and Latin America.[503] A consensus report by American intelligence agencies in April 2021 concluded, "Efforts to contain and manage the virus have reinforced nationalist trends globally, as some states turned inward to protect their citizens and sometimes cast blame on marginalized groups." Furthermore, COVID-19 has inflamed partisanship and polarisation around the world as bitter arguments explode over whom to scapegoat and whom to help first. The risks include further disruption of international trade and the formation of no-entry enclaves.[504]
Travel restrictions
As a result of the pandemic, many countries and regions imposed quarantines, entry bans, or other restrictions, either for citizens, recent travellers to affected areas,[505] or for all travellers.[506] Together with a decreased willingness to travel, this had a negative economic and social impact on the travel sector. Concerns have been raised over the effectiveness of travel restrictions to contain the spread of COVID-19.[507] A study in Science found that travel restrictions had only modestly affected the initial spread of COVID-19, unless combined with infection prevention and control measures to considerably reduce transmissions.[508] Researchers concluded that "travel restrictions are most useful in the early and late phase of an epidemic" and "restrictions of travel from Wuhan unfortunately came too late".[509]
The European Union rejected the idea of suspending the Schengen free travel zone.[510][511]
Evacuation of foreign citizens

Owing to the effective lockdown of Wuhan and Hubei, several countries evacuated their citizens and diplomatic staff from the area, primarily through chartered flights of the home nation, with Chinese authorities providing clearance. Canada, the United States, Japan, India,[512] Sri Lanka, Australia, France, Argentina, Germany, and Thailand were among the first to plan the evacuation of their citizens.[513] Brazil and New Zealand also evacuated their own nationals and some other people.[514][515] On 14 March 2020, South Africa repatriated 112 South Africans who tested negative for the virus from Wuhan, while four who showed symptoms were left behind to mitigate risk.[516] Pakistan said it would not evacuate citizens from China.[517]
On 15 February 2020, the U.S. announced it would evacuate Americans aboard the cruise ship Diamond Princess,[518] and on 21 February, Canada evacuated 129 Canadian passengers from the ship.[519] In early March, the Indian government began evacuating its citizens from Iran.[520][521] On 20 March, the United States began to partially withdraw its troops from Iraq due to the pandemic.[522]
United Nations response measures
In June 2020, the Secretary-General of the United Nations launched the "UN Comprehensive Response to COVID-19".[523] The United Nations Conference on Trade and Development (UNSC) has been criticised for a slow coordinated response, especially regarding the UN's global ceasefire, which aims to open up humanitarian access to the world's most vulnerable in conflict zones.[524]
WHO response measures

The WHO is a leading organisation involved in the global coordination for mitigating the pandemic.
The WHO has spearheaded several initiatives like the COVID-19 Solidarity Response Fund to raise money for the pandemic response, the UN COVID-19 Supply Chain Task Force, and the solidarity trial for investigating potential treatment options for the disease. The WHO's COVAX vaccine-sharing program aims to distribute 2 billion doses of COVID-19 vaccine for free or at a reduced cost by the end of 2021,[525] and has begun distributing them.
The WHO's handling of the initial outbreak of the pandemic has required a "diplomatic balancing act" between member states, in particular between the United States and China.[526] On August 27, the WHO announced the setting up of an independent expert Review Committee to examine aspects of the international treaty that governs preparedness and response to health emergencies. A WHO-led international mission arrived in China in January 2021 to investigate the origins of the COVID-19 pandemic and released preliminary findings in February 2021.Protests against governmental measures
In several countries, protests have risen against governmental restrictive responses to the COVID-19 pandemic, such as lockdowns. A February 2021 study found that large protest rallies against COVID-19 measures are likely to directly increase the spread of viruses, including COVID-19.[527]
Impact
Economics
The outbreak is a major destabilising threat to the global economy. One estimate from an expert at Washington University in St. Louis gave a $300+ billion impact on the world's supply chain that could last up to two years.[528] Global stock markets fell on 24 February due to a significant rise in the number of COVID-19 cases outside China.[529][530] On 27 February, due to mounting worries about the COVID-19 outbreak, U.S. stock indexes posted their sharpest falls since 2008, with the Dow falling 1,191 points (the largest one-day drop since the financial crisis of 2007–08)[531] and all three major indexes ending the week down more than 10 per cent.[532] On 28 February, Scope Ratings GmbH affirmed China's sovereign credit rating but maintained a Negative Outlook.[533] Stocks plunged again due to coronavirus fears, the largest fall being on 16 March.[534]
Lloyd's of London estimated that the global insurance industry will absorb losses of US$204 billion, exceeding the losses from the 2017 Atlantic hurricane season and 11 September attacks, suggesting the COVID-19 pandemic will likely go down in history as the costliest disaster ever in human history.[535]

Tourism is one of the worst affected sectors due to travel bans, closing of public places including travel attractions, and advice of governments against travel. Numerous airlines have cancelled flights due to lower demand, and British regional airline Flybe collapsed.[536] The cruise line industry was hard hit,[537] and several train stations and ferry ports have also been closed.[538] International mail between some countries stopped or was delayed due to reduced transportation between them or suspension of domestic service.[539]
The retail sector has been impacted globally, with reductions in store hours or temporary closures.[540] Visits to retailers in Europe and Latin America declined by 40 per cent. North America and Middle East retailers saw a 50–60 per cent drop.[541] This also resulted in a 33–43 per cent drop in foot traffic to shopping centres in March compared to February. Shopping mall operators around the world imposed additional measures, such as increased sanitation, installation of thermal scanners to check the temperature of shoppers, and cancellation of events.[542]
Hundreds of millions of jobs could be lost globally.[543][544] More than 40 million Americans lost their jobs and filed unemployment insurance claims.[545] The economic impact and mass unemployment caused by the pandemic has raised fears of a mass eviction crisis,[546][547] with an analysis by the Aspen Institute indicating between 30 and 40 million Americans are at risk for eviction by the end of 2020.[548][549] According to a report by Yelp, about 60% of U.S. businesses that have closed since the start of the pandemic will stay shut permanently.[550]
According to a United Nations Economic Commission for Latin America estimate, the pandemic-induced recession could leave 14–22 million more people in extreme poverty in Latin America than would have been in that situation without the pandemic.[551] According to the World Bank, up to 100 million more people globally could fall into extreme poverty due to the shutdowns.[552][553] The International Labour Organization (ILO) informed that the income generated in the first nine months of 2020 from work across the world dropped by 10.7 per cent, or $3.5 trillion, amidst the COVID-19 outbreak.[554]
Supply shortages

The outbreak has been blamed for several instances of supply shortages, stemming from globally increased usage of equipment to fight outbreaks, panic buying (which in several places led to shelves being cleared of grocery essentials such as food, toilet paper, and bottled water), and disruption to factory and logistic operations.[555] The spread of panic buying has been found to stem from perceived threat, perceived scarcity, fear of the unknown, coping behaviour and social psychological factors (e.g. social influence and trust).[556] The technology industry, in particular, has warned of delays to shipments of electronic goods.[557] According to the WHO director-general Tedros Adhanom, demand for personal protection equipment has risen a hundredfold, leading to prices up to twenty times the normal price and also delays in the supply of medical items of four to six months.[558][559] It has also caused a shortage of personal protective equipment worldwide, with the WHO warning that this will endanger health workers.[560]
The impact of the COVID-19 outbreak was worldwide. The virus created a shortage of precursors (raw material) used in the manufacturing of fentanyl and methamphetamine.[561] Price increases and shortages in these illegal drugs have been noticed on the streets of the UK.[562]
The pandemic has disrupted global food supplies and threatens to trigger a new food crisis.[563][564] David Beasley, head of the World Food Programme (WFP), said "we could be facing multiple famines of biblical proportions within a short few months."[565] Senior officials at the United Nations estimated in April 2020 that an additional 130 million people could starve, for a total of 265 million by the end of 2020.[565][566][567]
Oil and other energy markets
In early February 2020, Organization of the Petroleum Exporting Countries (OPEC) "scrambled" after a steep decline in oil prices due to lower demand from China.[568] On Monday, 20 April, the price of West Texas Intermediate (WTI) went negative and fell to a record low (minus $37.63 a barrel) due to traders' offloading holdings so as not to take delivery and incur storage costs.[569] June prices were down but in the positive range, with a barrel of West Texas trading above $20.[569]
Culture
The performing arts and cultural heritage sectors have been profoundly affected by the pandemic, impacting organisations' operations as well as individuals—both employed and independent—globally. By March 2020, across the world and to varying degrees, museums, libraries, performance venues, and other cultural institutions had been indefinitely closed with their exhibitions, events and performances cancelled or postponed.[570] Some services continued through digital platforms,[571][572][573] such as live streaming concerts[574] or web-based arts festivals.[575]

Holy Week observances in Rome, which occur during the last week of the Christian penitential season of Lent, were cancelled.[572] Many dioceses have recommended older Christians stay home rather than attend Mass on Sundays; services have been made available via radio, online live streaming and television, though some congregations have made provisions for drive-in worship.[572][576][577] With the Roman Catholic Diocese of Rome closing its churches and chapels and St. Peter's Square emptied of Christian pilgrims,[572] other religious bodies also cancelled in-person services and limited public gatherings in churches, mosques, synagogues, temples and gurdwaras.[572] Iran's Health Ministry announced the cancellation of Friday prayers in areas affected by the outbreak and shrines were later closed,[318][325] while Saudi Arabia banned the entry of foreign pilgrims as well as its residents to holy sites in Mecca and Medina.[578][579] The 2020 Hajj was limited to around 1,000 selected pilgrims, in contrast to the usual number of over 2 million.[580]
The pandemic has caused the most significant disruption to the worldwide sporting calendar since the Second World War. Most major sporting events have been cancelled or postponed, including the 2019–20 UEFA Champions League,[581] 2019–20 Premier League,[582] UEFA Euro 2020, 2019–20 NBA season,[583] 2019–20 NHL season,[584] and 2020 Arctic Winter Games.[585] The outbreak disrupted plans for the 2020 Summer Olympics in Tokyo, Japan, which were originally scheduled to start at 24 July 2020, and were postponed by the International Olympic Committee to 23 July 2021.[586][587][588]
The entertainment industry has also been affected, with many music groups suspending or cancelling concert tours.[589][590] The Eurovision Song Contest, which was due to be held in Rotterdam, the Netherlands in May, was cancelled; however, the Netherlands was retained as host for 2021.[591][592] Many large theatres such as those on Broadway also suspended all performances.[593]
The large number of people working or learning from home via videoconferencing software led to several new terms and trends, including "Zoom fatigue",[594] a decline in demand for formal clothing, and increased fashion focus on masks and clothes for the upper body (the lower body generally not being visible on a videoconference).[595] The term "doomscrolling" became more widely used. Online, numerous COVID-19-themed Internet memes have spread as many turn to humour and distraction amid the uncertainty.[596]
Politics

The pandemic has affected the political systems of multiple countries, causing suspensions of legislative activities,[597] isolations or deaths of multiple politicians,[598] and rescheduling of elections due to fears of spreading the virus.[599]
Although they have broad support among epidemiologists, social distancing measures have been politically controversial in many countries. Intellectual opposition to social distancing has come primarily from writers of other fields, although there are a few heterodox epidemiologists.[600]
On 23 March 2020, United Nations Secretary-General António Manuel de Oliveira Guterres issued an appeal for a global ceasefire in response to the pandemic;[601][602] 172 UN Member States and Observers signed a non-binding statement in support of the appeal in June,[603] and the UN Security Council passed a resolution supporting it in July.[604][605]
China
The government of China has been criticised by the United States,[606] the UK Minister for the Cabinet Office Michael Gove,[607] and others[608] for its handling of the pandemic. A number of provincial-level administrators of the Communist Party of China were dismissed over their handling of the quarantine measures in China, a sign of discontent with their response to the outbreak. Some commentators believed this move was intended to protect CCP general secretary Xi Jinping from the controversy.[609] The U.S. intelligence community claims China intentionally under-reported its number of COVID-19 cases.[610] The Chinese government maintains it has acted swiftly and transparently.[611][612] However, journalists and activists who have reported on the pandemic have been detained by authorities,[613][614] such as Zhang Zhan, who was arrested and tortured for reporting on the pandemic and the detainment of other independent journalists.[615][616][617]
Italy
In early March, the Italian government criticised the EU's lack of solidarity with coronavirus-affected Italy[618][619]—Maurizio Massari, Italy's ambassador to the EU, said "only China responded bilaterally", not the EU.[620] On 22 March, after a phone call with Italian Prime Minister Giuseppe Conte, Russian president Vladimir Putin had the Russian army send military medics, disinfection vehicles, and other medical equipment to Italy.[621] President of Lombardy Attilio Fontana and Italian Foreign Minister Luigi Di Maio expressed their gratitude for the aid.[622] Russia also sent a cargo plane with medical aid to the United States.[623] Kremlin spokesman Dmitry Peskov said "when offering assistance to U.S. colleagues, [Putin] assumes that when U.S. manufacturers of medical equipment and materials gain momentum, they will also be able to reciprocate if necessary."[624] In early April, Norway and EU states like Romania and Austria started to offer help by sending medical personnel and disinfectant,[625] and Ursula von der Leyen offered an official apology to the country.[626]
United States
The outbreak prompted calls for the United States to adopt social policies common in other wealthy countries, including universal health care, universal child care, paid sick leave, and higher levels of funding for public health.[628][629][630] Political analysts believe it may have contributed to Donald Trump's loss in the 2020 presidential election.[631][632] Beginning in mid-April 2020, there were protests in several U.S. states against government-imposed business closures and restricted personal movement and association.[633] Simultaneously, protests ensued by essential workers in the form of a general strike.[634] In early October 2020, Donald Trump, his family members, and many other government officials were diagnosed with COVID-19, further disrupting the country's politics.[635]
Other countries
The planned NATO "Defender 2020" military exercise in Germany, Poland, and the Baltic states, the largest NATO war exercise since the end of the Cold War, was held on a reduced scale.[636][637] The Campaign for Nuclear Disarmament's general secretary Kate Hudson criticised the exercise, saying "it jeopardises the lives not only of the troops from the U.S. and the many European countries participating but the inhabitants of the countries in which they are operating."[638]
The Iranian government has been heavily affected by the virus, with about two dozen parliament members and fifteen current or former political figures infected.[328][639] Iran's President Hassan Rouhani wrote a public letter to world leaders asking for help on 14 March 2020, saying they were struggling to fight the outbreak due to a lack of access to international markets from the United States sanctions against Iran.[640] Saudi Arabia, which launched a military intervention in Yemen in March 2015, declared a ceasefire.[641]
Diplomatic relations between Japan and South Korea worsened due to the pandemic.[642] South Korea criticised Japan's "ambiguous and passive quarantine efforts" after Japan announced anyone coming from South Korea would be placed in quarantine for two weeks at government-designated sites.[643] South Korean society was initially polarised on President Moon Jae-in's response to the crisis; many Koreans signed petitions either calling for Moon's impeachment or praising his response.[352]
Some countries have passed emergency legislation in response to the pandemic. Some commentators have expressed concern that it could allow governments to strengthen their grip on power.[644][645] In the Philippines, lawmakers granted president Rodrigo Duterte temporary emergency powers during the pandemic.[646] In Hungary, the parliament voted to allow the prime minister, Viktor Orbán, to rule by decree indefinitely, suspend parliament as well as elections, and punish those deemed to have spread false information about the virus and the government's handling of the crisis.[647] In some countries, including Egypt,[648] Turkey,[649] and Thailand,[646] opposition activists and government critics have been arrested for allegedly spreading fake news about the COVID-19 pandemic.[650]
In India, journalists criticising the government's response were arrested or issued warnings by police and authorities.[651] Rates of imprisoned or detained journalists increased worldwide, with some being related to the pandemic.[652][653]
Agriculture and food systems
The COVID-19 pandemic has disrupted agricultural and food systems worldwide.[654] COVID-19 hit at a time when hunger or undernourishment was once again on the rise in the world, with an estimated 690 million people already going hungry in 2019.[655] Based on the latest UN estimates, the economic recession triggered by the pandemic may lead to another 83 million people, and possibly as many as 132 million, going hungry in 2020.[655][656][657][658] This is mainly due to a lack of access to food – linked to falling incomes, lost remittances and, in some cases, a rise in food prices. In countries that already suffer from high levels of acute food insecurity, it is no longer an issue of access to food alone, but increasingly also one of food production.[654][655]
The pandemic, alongside lockdowns and travel restrictions, has prevented movement of aid and greatly impacted food production. As a result, several famines are forecast, which the UN called a crisis "of biblical proportions,"[659] or "hunger pandemic."[660] It is estimated that without intervention 30 million people may die of hunger, with Oxfam reporting that "12,000 people per day could die from COVID-19 linked hunger" by the end of 2020.[661][659][662] This pandemic, in conjunction with the 2019–2021 locust infestations and several ongoing armed conflicts, is predicted to form the worst series of famines since the Great Chinese Famine, affecting between 10 and 20 per cent of the global population in some way.[663] 55 countries are reported to be at risk, with three dozen succumbing to crisis-level famines or above in the worst-case scenario.[664] 265 million people are forecast to be in famine conditions, an increase of 125 million due to the pandemic.[661]
Education

The pandemic has severely impacted educational systems globally. Most governments have temporarily closed educational institutions, with many switching to online education. As of September 2020, approximately 1.077 billion learners were affected due to school closures in response to the pandemic. According to UNICEF monitoring, as of March 2020, 53 countries had closed all schools and 27 some, impacting about 61.6 per cent of the world's student population.[665] School closures impact not only students, teachers, and families but have far-reaching economic and societal consequences. They shed light on social and economic issues, including student debt, digital learning, food insecurity, and homelessness, as well as access to childcare, health care, housing, internet, and disability services. The impact has been more severe for disadvantaged children and their families.[citation needed]
The Higher Education Policy Institute conducted a report which discovered that around 63% of students claimed that their mental health had been worsened as a result of the COVID-19 pandemic, and alongside this 38% demonstrated satisfaction with the accessibility of mental health services. Despite this, the director for policy and advocacy at the institute has explained that it is still unclear as to how and when normality will resume for students regarding their education and living situation.[666]
Other health issues
The pandemic has had many impacts on global health beyond those caused by the COVID-19 disease itself. It has led to a reduction in hospital visits for other reasons. There have been 38 per cent fewer hospital visits for heart attack symptoms in the United States and 40 per cent fewer in Spain.[667] The head of cardiology at the University of Arizona said, "My worry is some of these people are dying at home because they're too scared to go to the hospital."[668] There is also concern that people with strokes and appendicitis are not seeking timely treatment.[668] Shortages of medical supplies have impacted people with various conditions.[669]
In several countries there has been a marked reduction of spread of sexually transmitted infections, including HIV/AIDS, attributable to COVID-19 quarantines, social distancing measures, and recommendations to not engage in casual sex.[670][671] Similarly, in some places, rates of transmission of influenza and other respiratory viruses significantly decreased during the pandemic.[672][673][674]
The pandemic has also negatively impacted mental health globally, including increased loneliness resulting from social distancing[675] and depression and domestic violence from lockdowns.[676] As of June 2020, 40% of U.S. adults were experiencing adverse mental health symptoms, with 11% having seriously considered trying to kill themselves in the past month.[677]
Paying attention and taking measures to prevent mental health problems and post-traumatic stress syndrome, particularly in women, is already a need.[678]Environment and climate

The worldwide disruption caused by the pandemic has resulted in numerous positive effects to the environment and climate. The global reduction in modern human activity such as the considerable decline in planned travel was coined anthropause and has caused a large drop in air pollution and water pollution in many regions.[680][681][682][683] In China, lockdowns and other measures resulted in a 25 percent reduction in carbon emissions and 50 percent reduction in nitrogen oxides emissions, which one Earth systems scientist estimated may have saved at least 77,000 lives over two months.[684][685][686][687]
Other positive effects on the environment include governance-system-controlled investments towards a sustainable energy transition and other goals related to environmental protection such as the European Union's seven-year €1 trillion budget proposal and €750 billion recovery plan "Next Generation EU" which seeks to reserve 25% of EU spending for climate-friendly expenditure.[688][689][690]
However, due to humans the pandemic has also provided cover for illegal activities such as deforestation of the Amazon rainforest and increased poaching in Africa. The hindering of environmental diplomacy efforts in combination of late capitalism also created economic fallout that some predict will slow investment in green energy technologies.[691][692][693][694][695][696]
Discrimination and prejudice
Heightened prejudice, xenophobia, and racism have been documented around the world toward people of Chinese and East Asian descent.[697][698][699][700][701] Reports from February 2020 (when most confirmed cases were confined to China) documented racist sentiments expressed in groups worldwide about Chinese people 'deserving' the virus.[702][703][704] Chinese people and other Asian peoples in the United Kingdom and United States have reported increasing levels of racist abuse and assaults.[705][706][707] Former U.S. President Donald Trump was criticised for referring to the COVID-19 as the "Chinese Virus" and "Kung Flu", which has been condemned as racist and xenophobic.[708][709][710] On 14 March, an Asian family, including a two-year-old girl, was attacked at knifepoint in Texas in what the FBI has called a COVID-19 related hate crime.[711]
Following the progression of the outbreak to new hotspot countries, people from Italy (the first country in Europe to experience a serious outbreak of COVID-19) were also subjected to suspicion and xenophobia,[712][713] as were people from hotspots in other countries. Discrimination against Muslims in India escalated after public health authorities identified an Islamic missionary (Tablighi Jamaat) group's gathering in New Delhi in early March 2020 as a source of spread.[714] As of late April 2020, Paris had seen riots break out over police treatment of marginalised ethnic groups during the then in-place lockdown.[715] Racism and xenophobia towards southern and south east Asians increased in the Arab states of the Persian Gulf.[716][717][718] South Korea's LGBTQ community was blamed by some for the spread of COVID-19 in Seoul.[719][720] In China, some people of African descent were evicted from their homes and told to leave China within 24 hours, due to disinformation that they and other foreigners were spreading the virus.[721] This racism and xenophobia was criticised by some foreign governments, diplomatic corps, and the Chinese ambassador to Zimbabwe.[722]
Age-based discrimination against older adults, while already present before the pandemic, was more prevalent during the pandemic. This has been attributed to their perceived vulnerability to the virus and subsequent physical and social isolation measures, which, coupled with their already reduced social activity, has increased dependency on others. Similarly, limited digital literacy has left the elderly more vulnerable to the effects of isolation, depression, and loneliness.[723]
Lifestyle change adaptation during the pandemic
The pandemic has resulted in many people adapting to massive changes in life, from increased internet commerce activity to the job market. Social distancing has caused increased sales from large e-commerce companies such as Amazon, Alibaba, and Coupang. Online retailers in the US posted 791.70 billion dollars in sales in 2020, an increase of 32.4% from 598.02 billion dollars from the year before.[724] The trend of home delivery orders have increased due to the pandemic, with indoor dining restaurants shutting down due to lockdown orders or low sales.[725][726] Hackers and cybercriminals/scammers have started targeting people due to the massive changes, with some pretending to be part of the CDC, and others using different phishing schemes.[727] Education worldwide has increasingly shifted from physical attendance to video conferencing apps such as Zoom as lockdown measures have resulted in schools being forced to shut down.[728] Due to the pandemic, mass layoffs have occurred in the airline, travel, hospitality, and some other industries. (There were no signs of permanent recovery as of May 2021[update].)[729][730]
Information dissemination
Ongoing COVID-19 research is indexed and searchable in the NIH COVID-19 Portfolio.[731] Some newspaper agencies removed their online paywalls for some or all of their COVID-19-related articles and posts,[732] while scientific publishers made scientific papers related to the outbreak available with open access.[733][734] Some scientists chose to share their results quickly on preprint servers such as bioRxiv.[735]
Maps have played a key role in disseminating information concerning the spatial distribution of the disease, especially with the development of dashboards to present data in near real-time. Methods of data visualisation have drawn some criticism, however, in the over-simplification of geographical patterns indicated by choropleth maps that adopt national, rather than local, map scales.[736]
Misinformation
The COVID-19 pandemic has resulted in misinformation and conspiracy theories about the scale of the pandemic and the origin, prevention, diagnosis, and treatment of the disease. False information, including intentional disinformation, has been spread through social media, text messaging,[737] and mass media. Journalists have been arrested for allegedly spreading fake news about the pandemic. False information has also been propagated by celebrities, politicians, and other prominent public figures. The spread of COVID-19 misinformation by governments has also been significant.
Commercial scams have claimed to offer at-home tests, supposed preventives, and "miracle" cures.[738] Several religious groups have claimed their faith will protect them from the virus.[739] Without evidence, some people have claimed the virus is a bioweapon accidentally or deliberately leaked from a laboratory, a population control scheme, the result of a spy operation, or the side effect of 5G upgrades to cellular networks.[740]
The World Health Organization (WHO) declared an "infodemic" of incorrect information about the virus that poses risks to global health.[741] While belief in conspiracy theories is not a new phenomenon, in the context of the COVID-19 pandemic, this can lead to adverse health effects. Cognitive biases, such as jumping to conclusions and confirmation bias, may be linked to the occurrence of conspiracy beliefs.[742]See also
- Emerging infectious disease
- Globalisation and disease
- List of epidemics and pandemics
- Timeline of the COVID-19 pandemic
Notes
References
- ^ Zoumpourlis, Vassilios; Goulielmaki, Maria; Rizos, Emmanouil; Baliou, Stella; Spandidos, Demetrios A. (22 October 2020). "The COVID-19 pandemic as a scientific and social challenge in the 21st century". Molecular Medicine Reports. 22 (4): 3035–3048. doi:10.3892/mmr.2020.11393. ISSN 1791-2997. PMC 7453598. PMID 32945405.
- ^ "Novel Coronavirus – China". World Health Organization (WHO). Retrieved 9 April 2020.
- ^ a b c d e f g "COVID-19 Dashboard by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU)". ArcGIS. Johns Hopkins University. Retrieved 13 June 2021.
- ^ "WHO: 10% of world's people may have been infected with virus". AP NEWS. 5 October 2020. Retrieved 12 November 2020.
- ^ a b CDC (11 February 2020). "Coronavirus Disease 2019 (COVID-19)". Centers for Disease Control and Prevention. Retrieved 6 December 2020.
- ^ Clinical Questions about COVID-19: Questions and Answers Centers for Disease Control and Prevention
- ^ "Coronavirus (COVID-19): General advice". nhsinform.scot. Retrieved 17 February 2021.
- ^ "The Great Lockdown: Worst Economic Downturn Since the Great Depression". IMF Blog. Retrieved 23 April 2020.
- ^ To, Kelvin Kai-Wang; Sridhar, Siddharth; Chiu, Kelvin Hei-Yeung; Hung, Derek Ling-Lung; Li, Xin; Hung, Ivan Fan-Ngai; Tam, Anthony Raymond; Chung, Tom Wai-Hin; Chan, Jasper Fuk-Woo; Zhang, Anna Jian-Xia; Cheng, Vincent Chi-Chung; Yuen, Kwok-Yung (2021). "Lessons learned 1 year after SARS-CoV-2 emergence leading to COVID-19 pandemic". Emerging Microbes & Infections. 10 (1): 507–535. doi:10.1080/22221751.2021.1898291. ISSN 2222-1751. PMC 8006950. PMID 33666147.
- ^ Sun J, He W, Wang L, Lai A, Ji X, Zhai X, et al. (2020). "COVID-19: Epidemiology, Evolution, and Cross-Disciplinary Perspectives". Trends in Molecular Medicine. 26 (5): 483–495. doi:10.1016/j.molmed.2020.02.008. PMC 7118693. PMID 32359479.
- ^ "WHO Points To Wildlife Farms In Southern China As Likely Source Of Pandemic". NPR. 15 March 2021.
- ^ a b Maxmen, Amy (30 March 2021). "WHO report into COVID pandemic origins zeroes in on animal markets, not labs". Nature. 592 (7853): 173–174. Bibcode:2021Natur.592..173M. doi:10.1038/d41586-021-00865-8. PMID 33785930. S2CID 232429241.
- ^ a b Hu, Ben; Guo, Hua; Zhou, Peng; Shi, Zheng-Li (6 October 2020). "Characteristics of SARS-CoV-2 and COVID-19". Nature Reviews. Microbiology. 19 (3): 141–154. doi:10.1038/s41579-020-00459-7. ISSN 1740-1526. PMC 7537588. PMID 33024307.
- ^ a b Graham, Rachel L.; Baric, Ralph S. (19 May 2020). "SARS-CoV-2: Combating Coronavirus Emergence". Immunity. 52 (5): 734–736. doi:10.1016/j.immuni.2020.04.016. ISSN 1074-7613. PMC 7207110. PMID 32392464.
- ^ Adhanom, Tedros. "WHO Director-General's remarks at the media briefing on 2019-nCoV on 11 February 2020". World Health Organization (WHO). Retrieved 24 October 2020.
- ^ Lovelace Jr, Berkeley (11 February 2020). "World Health Organization names the new coronavirus: COVID-19". CNBC. Retrieved 23 October 2020.
- ^ Perlman S (February 2020). "Another Decade, Another Coronavirus". The New England Journal of Medicine. 382 (8): 760–762. doi:10.1056/NEJMe2001126. PMC 7121143. PMID 31978944.
- ^ Cyranoski D (March 2020). "Mystery deepens over animal source of coronavirus". Nature. 579 (7797): 18–19. Bibcode:2020Natur.579...18C. doi:10.1038/d41586-020-00548-w. PMID 32127703. S2CID 211836524.
- ^ Zhang T, Wu Q, Zhang Z (April 2020). "Probable Pangolin Origin of SARS‑CoV‑2 Associated with the COVID-19 Outbreak". Current Biology. 30 (7): 1346–1351.e2. doi:10.1016/j.cub.2020.03.022. PMC 7156161. PMID 32197085.
- ^ "Outbreak of severe acute respiratory syndrome coronavirus 2 (SARS‑CoV‑2): increased transmission beyond China – fourth update" (PDF). European Centre for Disease Prevention and Control. 14 February 2020. Retrieved 8 March 2020.
- ^ "The COVID-19 coronavirus epidemic has a natural origin, scientists say – Scripps Research's analysis of public genome sequence data from SARS‑CoV‑2 and related viruses found no evidence that the virus was made in a laboratory or otherwise engineered". EurekAlert!. Scripps Research Institute. 17 March 2020. Retrieved 15 April 2020.
- ^ Andersen KG, Rambaut A, Lipkin WI, Holmes EC, Garry RF (April 2020). "The proximal origin of SARS-CoV-2". Nature Medicine. 26 (4): 450–452. doi:10.1038/s41591-020-0820-9. PMC 7095063. PMID 32284615.
- ^ Latinne, Alice; Hu, Ben; Olival, Kevin J.; Zhu, Guangjian; Zhang, Libiao; Li, Hongying; Chmura, Aleksei A.; Field, Hume E.; Zambrana-Torrelio, Carlos; Epstein, Jonathan H.; Li, Bei; Zhang, Wei; Wang, Lin-Fa; Shi, Zheng-Li; Daszak, Peter (25 August 2020). "Origin and cross-species transmission of bat coronaviruses in China". Nature Communications. 11 (1): 4235. Bibcode:2020NatCo..11.4235L. doi:10.1038/s41467-020-17687-3. ISSN 2041-1723. PMC 7447761. PMID 32843626.
- ^ Hakim, Mohamad S. (14 February 2021). "SARS-CoV-2, Covid-19, and the debunking of conspiracy theories". Reviews in Medical Virology: e2222. doi:10.1002/rmv.2222. ISSN 1099-1654. PMC 7995093. PMID 33586302.
- ^ Qin, Amy; Wang, Vivian; Hakim, Danny (20 November 2020). "How Steve Bannon and a Chinese Billionaire Created a Right-Wing Coronavirus Media Sensation". The New York Times. Archived from the original on 30 April 2021.
- ^ Frutos, Roger; Gavotte, Laurent; Devaux, Christian A. (18 March 2021). "Understanding the origin of COVID-19 requires to change the paradigm on zoonotic emergence from the spillover model to the viral circulation model". Infection, Genetics and Evolution: 104812. doi:10.1016/j.meegid.2021.104812. ISSN 1567-1348. PMC 7969828. PMID 33744401.
The origin of SARS-Cov-2 is still passionately debated since it makes ground for geopolitical confrontations and conspiracy theories besides scientific ones.
- ^ Maxmen, Amy (27 May 2021). "Divisive COVID 'lab leak' debate prompts dire warnings from researchers". Nature. doi:10.1038/d41586-021-01383-3.
- ^ Ni, Vincent; Borger, Julian (27 May 2021). "Biden move to investigate Covid origins opens new rift in US-China relations". The Guardian.
- ^ Cohen J (January 2020). "Wuhan seafood market may not be source of novel virus spreading globally". Science. doi:10.1126/science.abb0611.
- ^ Wang C, Horby PW, Hayden FG, Gao GF (February 2020). "A novel coronavirus outbreak of global health concern". Lancet. 395 (10223): 470–473. doi:10.1016/S0140-6736(20)30185-9. PMC 7135038. PMID 31986257.
- ^ Ma J (13 March 2020). "Coronavirus: China's first confirmed Covid-19 case traced back to November 17". South China Morning Post. Archived from the original on 13 March 2020. Retrieved 16 March 2020.
- ^ a b Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. (24 January 2020). "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China". Lancet. 395 (10223): 497–506. doi:10.1016/S0140-6736(20)30183-5. PMC 7159299. PMID 31986264.
- ^ Joseph A (24 January 2020). "New coronavirus can cause infections with no symptoms and sicken otherwise healthy people, studies show". Stat. Archived from the original on 24 January 2020. Retrieved 27 January 2020.
- ^ Chan JF, Yuan S, Kok KH, To KK, Chu H, Yang J, et al. (February 2020). "A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster". Lancet. 395 (10223): 514–523. doi:10.1016/S0140-6736(20)30154-9. PMC 7159286. PMID 31986261.
- ^ Pekar, Jonathan; Worobey, Michael; Moshiri, Niema; Scheffler, Konrad; Wertheim, Joel O. (23 April 2021). "Timing the SARS-CoV-2 index case in Hubei province". Science. 372 (6540): 412–417. Bibcode:2021Sci...372..412P. doi:10.1126/science.abf8003. ISSN 1095-9203. PMC 8139421. PMID 33737402.
- ^ To, Kelvin Kai-Wang; Sridhar, Siddharth; Chiu, Kelvin Hei-Yeung; Hung, Derek Ling-Lung; Li, Xin; Hung, Ivan Fan-Ngai; Tam, Anthony Raymond; Chung, Tom Wai-Hin; Chan, Jasper Fuk-Woo; Zhang, Anna Jian-Xia; Cheng, Vincent Chi-Chung; Yuen, Kwok-Yung (22 March 2021). "Lessons learned 1 year after SARS-CoV-2 emergence leading to COVID-19 pandemic". Emerging Microbes & Infections. 10 (1): 507–535. doi:10.1080/22221751.2021.1898291. ISSN 2222-1751. PMC 8006950. PMID 33666147.
- ^ "Laboratory testing for 2019 novel coronavirus (2019-nCoV) in suspected human cases". World Health Organization (WHO). Retrieved 30 March 2020.
- ^ "Total tests for COVID-19 per 1,000 people". Our World in Data. Retrieved 16 April 2020.
- ^ Sevillano EG, Linde P, Vizoso S (23 March 2020). "640,000 rapid coronavirus tests arrive in Spain". El País. Retrieved 2 April 2020.
- ^ "Special Report: Italy and South Korea virus outbreaks reveal disparity in deaths and tactics". Reuters. 13 March 2020. Retrieved 30 March 2020.
- ^ Li R, Pei S, Chen B, Song Y, Zhang T, Yang W, Shaman J (March 2020). "Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus (SARS-CoV2)". Science. 368 (6490): 489–493. Bibcode:2020Sci...368..489L. doi:10.1126/science.abb3221. PMC 7164387. PMID 32179701.
- ^ "Report 13 – Estimating the number of infections and the impact of non-pharmaceutical interventions on COVID-19 in 11 European countries". Imperial College London. Retrieved 7 April 2020.
- ^ Lau H, Khosrawipour V, Kocbach P, Mikolajczyk A, Ichii H, Schubert J, et al. (March 2020). "Internationally lost COVID-19 cases". Journal of Microbiology, Immunology, and Infection = Wei Mian Yu Gan Ran Za Zhi. 53 (3): 454–458. doi:10.1016/j.jmii.2020.03.013. PMC 7102572. PMID 32205091.
- ^ Streeck H (9 April 2020). "Vorläufiges Ergebnis und Schlussfolgerungen der COVID-19 Case-Cluster-Study (Gemeinde Gangelt)" (PDF). Land NRW – State of North Rhine-Westphalia. Retrieved 13 April 2020.
- ^ Sutton D, Fuchs K, D'Alton M, Goffman D (April 2020). "Universal Screening for SARS-CoV-2 in Women Admitted for Delivery". The New England Journal of Medicine. 382 (22): 2163–2164. doi:10.1056/NEJMc2009316. PMC 7175422. PMID 32283004.
- ^ "Dutch study suggests 3% of population may have coronavirus antibodies". Reuters. 16 April 2020. Retrieved 20 April 2020.
- ^ "Interactive Serology Dashboard for Commercial Laboratory Surveys". Centres for Disease Control and Prevention. 21 July 2020. Retrieved 24 July 2020.
- ^ Vogel G (21 April 2020). "Antibody surveys suggesting vast undercount of coronavirus infections may be unreliable". Science. doi:10.1126/science.abc3831. S2CID 218794298.
- ^ "China: age distribution of novel coronavirus patients 2020". Statista. Retrieved 11 April 2020.
- ^ Scott D (23 March 2020). "The Covid-19 risks for different age groups, explained". Vox. Retrieved 12 April 2020.
- ^ Bi, Qifang; Wu, Yongsheng; Mei, Shujiang; Ye, Chenfei; Zou, Xuan; Zhang, Zhen; Liu, Xiaojian; Wei, Lan; Truelove, Shaun A; Zhang, Tong; Gao, Wei; Cheng, Cong; Tang, Xiujuan; Wu, Xiaoliang; Wu, Yu; Sun, Binbin; Huang, Suli; Sun, Yu; Zhang, Juncen; Ma, Ting; Lessler, Justin; Feng, Tiejian (August 2020). "Epidemiology and transmission of COVID-19 in 391 cases and 1286 of their close contacts in Shenzhen, China: a retrospective cohort study". The Lancet Infectious Diseases. 20 (8): 911–919. doi:10.1016/S1473-3099(20)30287-5. PMC 7185944. PMID 32353347.
- ^ "Statement on the meeting of the International Health Regulations (2005) Emergency Committee regarding the outbreak of novel coronavirus 2019 (n-CoV) on 23 January 2020". World Health Organization (WHO). Retrieved 9 April 2020.
- ^ Sanche S, Lin YT, Xu C, Romero-Severson E, Hengartner N, Ke R (April 2020). "High Contagiousness and Rapid Spread of Severe Acute Respiratory Syndrome Coronavirus 2". Emerging Infectious Diseases. 26 (7): 1470–1477. doi:10.3201/eid2607.200282. PMC 7323562. PMID 32255761. S2CID 215410037.
- ^ Roberts L (8 May 2020). "The importance of the coronavirus R rate in other countries across the globe". The Daily Telegraph. Retrieved 14 May 2020.
- ^ a b c "European Centre for Disease Prevention and Control". Retrieved 31 December 2020.
- ^ "Italy's coronavirus deaths could be underestimated in data: Official". Reuters. 31 March 2020.
- ^ "Coronavirus: Is Covid-19 really the cause of all the fatalities in Italy?". Stuff. 20 March 2020. Retrieved 16 April 2020.
- ^ Wu J, McCann A, Katz J, Peltier E. "28,000 Missing Deaths: Tracking the True Toll of the Coronavirus Crisis". The New York Times. ISSN 0362-4331. Retrieved 22 April 2020.
- ^ "Tracking covid-19 excess deaths across countries". The Economist. ISSN 0013-0613. Retrieved 22 April 2020.
- ^ "What 'Excess Deaths' Do and Don't Tell Us About COVID-19". Reason. 29 April 2020. Retrieved 4 May 2020.
- ^ "Coronavirus Death Toll Climbs in China, and a Lockdown Widens". The New York Times. 23 January 2020. Archived from the original on 6 February 2020. Retrieved 10 February 2020.
- ^ Ramzy A, May T (2 February 2020). "Philippines Reports First Coronavirus Death Outside China". The New York Times. Archived from the original on 3 February 2020. Retrieved 4 February 2020.
- ^ Fuller, Thomas; Baker, Mike (7 May 2020). "Coronavirus Death in California Came Weeks Before First Known U.S. Death". The New York Times. Retrieved 15 September 2020.
- ^ Rothan HA, Byrareddy SN (May 2020). "The epidemiology and pathogenesis of coronavirus disease (COVID-19) outbreak". Journal of Autoimmunity. 109: 102433. doi:10.1016/j.jaut.2020.102433. PMC 7127067. PMID 32113704.
- ^ Yanez, N. David; Weiss, Noel S.; Romand, Jacques-André; Treggiari, Miriam M. (December 2020). "COVID-19 mortality risk for older men and women". BMC Public Health. 20 (1): 1742. doi:10.1186/s12889-020-09826-8. PMC 7675386. PMID 33213391.
- ^ "People with Certain Medical Conditions". Centers for Disease Control and Prevention. 15 March 2021. Retrieved 19 March 2021.
- ^ "Principles of Epidemiology | Lesson 3 – Section 3". U.S. Centers for Disease Control and Prevention (CDC). 18 February 2019. Retrieved 28 March 2020.
- ^ "The Best Global Responses to the COVID-19 Pandemic". Time. Retrieved 18 August 2020.
- ^ Barrio PL (11 May 2020). "Portugal and Spain: same peninsula, very different coronavirus impact". El País. Retrieved 25 May 2020.
- ^ Johnson M (5 April 2020). "Fewer deaths in Veneto offer clues for fight against virus". Financial Times. Retrieved 25 May 2020.
- ^ Ritchie H, Roser M (25 March 2020). Chivers T (ed.). "What do we know about the risk of dying from COVID-19?". Our World in Data. Retrieved 28 March 2020.
- ^ "Why Belgium's Death Rate Is So High: It Counts Lots Of Suspected COVID-19 Cases". NPR. Retrieved 25 April 2020.
- ^ Lazzerini M, Putoto G (March 2020). "COVID-19 in Italy: momentous decisions and many uncertainties". The Lancet. Global Health. 8 (5): e641–e642. doi:10.1016/S2214-109X(20)30110-8. PMC 7104294. PMID 32199072.
- ^ a b "Tracking covid-19 excess deaths across countries". The Economist. Retrieved 17 May 2021.
- ^ "IHME | COVID-19 Projections". Institute for Health Metrics and Evaluation. Retrieved 17 May 2021.
- ^ a b "COVID–19 Alert No. 2" (PDF). CDC. 24 March 2020. Retrieved 30 September 2020.
- ^ "Emergency use ICD codes for COVID-19 disease outbreak". World Health Organization. Retrieved 23 November 2020.
- ^ "International Guidelines for Certification and Classification (Coding) of Covid-19 as Cause of Death" (PDF). World Health Organization (WHO). 16 April 2020. Retrieved 3 October 2020.
- ^ "International Statistical Classification of Diseases and Related Health Problems 10th Revision". World Health Organization (WHO). 16 April 2020. Retrieved 4 October 2020.
- ^ a b Hauser, Anthony; Counotte, Michel J.; Margossian, Charles C.; Konstantinoudis, Garyfallos; Low, Nicola; Althaus, Christian L.; Riou, Julien (28 July 2020). "Estimation of SARS-CoV-2 mortality during the early stages of an epidemic: A modeling study in Hubei, China, and six regions in Europe". PLOS Medicine. 17 (7): e1003189. doi:10.1371/journal.pmed.1003189. PMC 7386608. PMID 32722715.
- ^ Tate, Nick. "What Changing Death Rates Tell Us About COVID-19". WebMD. Retrieved 19 September 2020.
- ^ a b c "Estimating mortality from COVID-19". World Health Organization. 4 August 2020. Retrieved 21 September 2020.
- ^ CDC (11 February 2020). "Coronavirus Disease 2019 (COVID-19)". Centers for Disease Control and Prevention. Retrieved 19 September 2020.
- ^ Mallapaty S (16 June 2020). "How deadly is the coronavirus? Scientists are close to an answer". Nature. 582 (7813): 467–468. Bibcode:2020Natur.582..467M. doi:10.1038/d41586-020-01738-2. PMID 32546810. S2CID 219726496.
- ^ Alwan N, Burgess R, Ashworth S, Beale R, Bhadelia N, Bogaert D, Dowd J, Eckerle I, Goldman L, Greenhalgh T, Gurdasani D, Hamdy A, Hanage W, Hodcroft E, Hyde Z, Kellam P, Kelly-Irving M, Krammer F, Lipsitch M, McNally A, McKee M, Nouri A, Pimenta D, Priesemann V, Rutter H, Silver J, Sridhar D, Swanton C, Walensky R, Yamey G, Ziauddeen H (31 October 2020). "Scientific consensus on the COVID-19 pandemic: we need to act now". The Lancet. 396 (10260): E71–E72. doi:10.1016/S0140-6736(20)32153-X. PMC 7557300. PMID 33069277.
- ^ Meyerowitz-Katz G, Merone L (December 2020). "A systematic review and meta-analysis of published research data on COVID-19 infection fatality rates". International Journal of Infectious Diseases. 101: 138–148. doi:10.1016/j.ijid.2020.09.1464. PMC 7524446. PMID 33007452.
- ^ Yang W, Kandula S, Huynh M, Greene S, Van Wye G, Li W, Chan H, McGibbon E, Yeung A, Olson D, Fine A, Shaman J (19 October 2020). "Estimating the infection-fatality risk of SARS-CoV-2 in New York City during the spring 2020 pandemic wave: a model-based analysis". Lancet Infectious Diseases. 21 (2): 203–212. doi:10.1016/S1473-3099(20)30769-6. PMC 7572090. PMID 33091374.
- ^ Pastor-Barriuso R, Pérez-Gómez B, Hernán M, Pérez-Olmeda M, Yotti R, Oteo-Iglesias J, Sanmartín J, León-Gómez I, Fernández-García A, Fernández-Navarro P, Cruz I, Martín M, Delgado-Sanz C, Fernández N, León J, Muñoz-Montalvo J, Blanco F, Larrauri A, Pollán M (27 November 2020). "Infection fatality risk for SARS-CoV-2 in community dwelling population of Spain: nationwide seroepidemiological study". British Medical Journal. 371: m4509. doi:10.1136/bmj.m4509. PMC 7690290. PMID 33246972.
- ^ O'Driscoll, Megan; Ribeiro Dos Santos, Gabriel; Wang, Lin; Cummings, Derek A. T.; Azman, Andrew S.; Paireau, Juliette; Fontanet, Arnaud; Cauchemez, Simon; Salje, Henrik (2 November 2020). "Age-specific mortality and immunity patterns of SARS-CoV-2". Nature. 590 (7844): 140–145. doi:10.1038/s41586-020-2918-0. ISSN 1476-4687. PMID 33137809. S2CID 226244375.
- ^ a b c d Levin A, Hanage W, Owusu-Boaitey N, Cochran K, Walsh S, Meyerowitz-Katz G (December 2020). "Assessing the Age Specificity of Infection Fatality Rates for COVID-19: Systematic Review, Meta-Analysis, and Public Policy Implications". European Journal of Epidemiology. 35 (12): 1123–1138. doi:10.1007/s10654-020-00698-1. PMC 7721859. PMID 33289900.
- ^ Organization, World Health (22 December 2020). "Background paper on Covid-19 disease and vaccines: prepared by the Strategic Advisory Group of Experts (SAGE) on immunization working group on COVID-19 vaccines". World Health Organization. hdl:10665/338095.
- ^ "Symptoms of Coronavirus". U.S. Centers for Disease Control and Prevention (CDC). 22 February 2021. Archived from the original on 4 March 2021. Retrieved 4 March 2021.
- ^ Grant MC, Geoghegan L, Arbyn M, Mohammed Z, McGuinness L, Clarke EL, Wade RG (23 June 2020). "The prevalence of symptoms in 24,410 adults infected by the novel coronavirus (SARS-CoV-2; COVID-19): A systematic review and meta-analysis of 148 studies from 9 countries". PLOS ONE. 15 (6): e0234765. Bibcode:2020PLoSO..1534765G. doi:10.1371/journal.pone.0234765. PMC 7310678. PMID 32574165. S2CID 220046286.
- ^ Islam MA (November 2020). "Prevalence of Headache in Patients With Coronavirus Disease 2019 (COVID-19): A Systematic Review and Meta-Analysis of 14,275 Patients". Frontiers in Neurology. 11: 562634. doi:10.3389/fneur.2020.562634. PMC 7728918. PMID 33329305.
- ^ Saniasiaya J, Islam MA (April 2021). "Prevalence of Olfactory Dysfunction in Coronavirus Disease 2019 (COVID-19): A Meta-analysis of 27,492 Patients". The Laryngoscope. 131 (4): 865–878. doi:10.1002/lary.29286. PMC 7753439. PMID 33219539.
- ^ Saniasiaya J, Islam MA (November 2020). "Prevalence and Characteristics of Taste Disorders in Cases of COVID-19: A Meta-analysis of 29,349 Patients". Otolaryngology–Head and Neck Surgery: 1–10. doi:10.1177/0194599820981018. PMID 33320033.
- ^ Islam MA (April 2021). "Prevalence and characteristics of fever in adult and paediatric patients with coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis of 17515 patients". PLOS ONE. 16 (4): e0249788. doi:10.1371/journal.pone.0249788. PMC 8023501. PMID 33822812.
- ^ a b "Clinical characteristics of COVID-19". European Centre for Disease Prevention and Control. Retrieved 29 December 2020.
- ^ Niazkar HR, Zibaee B, Nasimi A, Bahri N (July 2020). "The neurological manifestations of COVID-19: a review article". Neurological Sciences. 41 (7): 1667–1671. doi:10.1007/s10072-020-04486-3. PMC 7262683. PMID 32483687.
- ^ "Interim Clinical Guidance for Management of Patients with Confirmed Coronavirus Disease (COVID-19)". U.S. Centers for Disease Control and Prevention (CDC). 6 April 2020. Archived from the original on 2 March 2020. Retrieved 19 April 2020.
- ^ Oran DP, Topol EJ (January 2021). "The Proportion of SARS-CoV-2 Infections That Are Asymptomatic : A Systematic Review". Annals of Internal Medicine. doi:10.7326/M20-6976. PMC 7839426. PMID 33481642.
- ^ "Transmission of COVID-19". European Centre for Disease Prevention and Control. Retrieved 6 December 2020.
- ^ Nogrady B (November 2020). "What the data say about asymptomatic COVID infections". Nature. 587 (7835): 534–535. Bibcode:2020Natur.587..534N. doi:10.1038/d41586-020-03141-3. PMID 33214725.
- ^ a b Gao Z, Xu Y, Sun C, Wang X, Guo Y, Qiu S, Ma K (February 2021). "A systematic review of asymptomatic infections with COVID-19". Journal of Microbiology, Immunology, and Infection = Wei Mian Yu Gan Ran Za Zhi. 54 (1): 12–16. doi:10.1016/j.jmii.2020.05.001. PMC 7227597. PMID 32425996.
- ^ Oran, Daniel P., and Eric J. Topol. “Prevalence of Asymptomatic SARS-CoV-2 Infection : A Narrative Review.” Annals of Internal Medicine. vol. 173,5 (2020): 362-367. doi:10.7326/M20-3012 PMID 32491919 Retrieved 14 January 2021.
- ^ Lai CC, Liu YH, Wang CY, Wang YH, Hsueh SC, Yen MY, et al. (June 2020). "Asymptomatic carrier state, acute respiratory disease, and pneumonia due to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2): Facts and myths". Journal of Microbiology, Immunology, and Infection = Wei Mian Yu Gan Ran Za Zhi. 53 (3): 404–412. doi:10.1016/j.jmii.2020.02.012. PMC 7128959. PMID 32173241.
- ^ a b Furukawa NW, Brooks JT, Sobel J (July 2020). "Evidence Supporting Transmission of Severe Acute Respiratory Syndrome Coronavirus 2 While Presymptomatic or Asymptomatic". Emerging Infectious Diseases. 26 (7). doi:10.3201/eid2607.201595. PMC 7323549. PMID 32364890.
- ^ a b Gandhi RT, Lynch JB, Del Rio C (October 2020). "Mild or Moderate Covid-19". The New England Journal of Medicine. 383 (18): 1757–1766. doi:10.1056/NEJMcp2009249. PMID 32329974.
- ^ Wiersinga WJ, Rhodes A, Cheng AC, Peacock SJ, Prescott HC (August 2020). "Pathophysiology, Transmission, Diagnosis, and Treatment of Coronavirus Disease 2019 (COVID-19): A Review". JAMA. 324 (8): 782–793. doi:10.1001/jama.2020.12839. PMID 32648899. S2CID 220465311.
- ^ CDC (11 February 2020). "COVID-19 and Your Health". Centers for Disease Control and Prevention. Retrieved 23 January 2021.
- ^ Worobey M, Pekar J, Larsen BB, Nelson MI, Hill V, Joy JB, et al. (October 2020). "The emergence of SARS-CoV-2 in Europe and North America". Science. 370 (6516): 564–570. doi:10.1126/science.abc8169. PMC 7810038. PMID 32912998.
- ^ a b Li C, Zhao C, Bao J, Tang B, Wang Y, Gu B (November 2020). "Laboratory diagnosis of coronavirus disease-2019 (COVID-19)". Clinica Chimica Acta; International Journal of Clinical Chemistry. 510: 35–46. doi:10.1016/j.cca.2020.06.045. PMC 7329657. PMID 32621814.
- ^ "2019 Novel Coronavirus (2019-nCoV) Situation Summary". U.S. Centers for Disease Control and Prevention (CDC). 30 January 2020. Archived from the original on 26 January 2020. Retrieved 30 January 2020.
- ^ "Coronavirus disease (COVID-19) technical guidance: Laboratory testing for 2019-nCoV in humans". World Health Organization (WHO). Archived from the original on 15 March 2020. Retrieved 14 March 2020.
- ^ Bullard J, Dust K, Funk D, Strong JE, Alexander D, Garnett L, et al. (December 2020). "Predicting Infectious Severe Acute Respiratory Syndrome Coronavirus 2 From Diagnostic Samples". Clinical Infectious Diseases. 71 (10): 2663–2666. doi:10.1093/cid/ciaa638. PMC 7314198. PMID 32442256.
- ^ "Interim Guidelines for Collecting, Handling, and Testing Clinical Specimens from Persons for Coronavirus Disease 2019 (COVID-19)". U.S. Centers for Disease Control and Prevention (CDC). 11 February 2020. Archived from the original on 4 March 2020. Retrieved 26 March 2020.
- ^ "Real-Time RT-PCR Panel for Detection 2019-nCoV". U.S. Centers for Disease Control and Prevention (CDC). 29 January 2020. Archived from the original on 30 January 2020. Retrieved 1 February 2020.
- ^ "Laboratory testing for 2019 novel coronavirus (2019-nCoV) in suspected human cases". World Health Organization (WHO). Archived from the original on 17 March 2020. Retrieved 13 March 2020.
- ^ a b c Salehi S, Abedi A, Balakrishnan S, Gholamrezanezhad A (July 2020). "Coronavirus Disease 2019 (COVID-19): A Systematic Review of Imaging Findings in 919 Patients". AJR. American Journal of Roentgenology. 215 (1): 87–93. doi:10.2214/AJR.20.23034. PMID 32174129.
- ^ "ACR Recommendations for the use of Chest Radiography and Computed Tomography (CT) for Suspected COVID-19 Infection". American College of Radiology. 22 March 2020. Archived from the original on 28 March 2020.
- ^ Pormohammad A, Ghorbani S, Khatami A, Razizadeh MH, Alborzi E, Zarei M, et al. (October 2020). "Comparison of influenza type A and B with COVID-19: A global systematic review and meta-analysis on clinical, laboratory and radiographic findings". Reviews in Medical Virology. 31 (3): e2179. doi:10.1002/rmv.2179. PMC 7646051. PMID 33035373. S2CID 222255245.
- ^ Lee EY, Ng MY, Khong PL (April 2020). "COVID-19 pneumonia: what has CT taught us?". The Lancet. Infectious Diseases. 20 (4): 384–385. doi:10.1016/S1473-3099(20)30134-1. PMC 7128449. PMID 32105641.
- ^ Li Y, Xia L (June 2020). "Coronavirus Disease 2019 (COVID-19): Role of Chest CT in Diagnosis and Management". AJR. American Journal of Roentgenology. 214 (6): 1280–1286. doi:10.2214/AJR.20.22954. PMID 32130038. S2CID 212416282.
- ^ Maier BF, Brockmann D (May 2020). "Effective containment explains subexponential growth in recent confirmed COVID-19 cases in China". Science. 368 (6492): 742–746. Bibcode:2020Sci...368..742M. doi:10.1126/science.abb4557. PMC 7164388. PMID 32269067. ("... initial exponential growth expected for an unconstrained outbreak.")
- ^ "Viral Load Exposure Factors". ReallyCorrect.com.
- ^ "Recommendation Regarding the Use of Cloth Face Coverings, Especially in Areas of Significant Community-Based Transmission". U.S. Centers for Disease Control and Prevention (CDC). 28 June 2020.
- ^ "Scientific Brief: SARS-CoV-2 and Potential Airborne Transmission". COVID-19 Published Science and Research. U.S. Centers for Disease Control and Prevention (CDC). 11 February 2020. Retrieved 30 October 2020.
- ^ Centers for Disease Control and Prevention (5 April 2020). "What to Do if You Are Sick". U.S. Centers for Disease Control and Prevention (CDC). Archived from the original on 14 February 2020. Retrieved 24 April 2020.
- ^ "Coronavirus Disease 2019 (COVID-19) – Prevention & Treatment". U.S. Centers for Disease Control and Prevention (CDC). 10 March 2020. Archived from the original on 11 March 2020. Retrieved 11 March 2020.
- ^ a b "COVID-19 vaccine development pipeline (Refresh URL to update)". Vaccine Centre, London School of Hygiene and Tropical Medicine. 1 March 2021. Retrieved 10 March 2021.
- ^ Beaumont P (18 November 2020). "Covid-19 vaccine: who are countries prioritising for first doses?". The Guardian. ISSN 0261-3077. Retrieved 26 December 2020.
- ^ Plotkin SA, Halsey N (January 2021). "Accelerate COVID-19 Vaccine Rollout by Delaying the Second Dose of mRNA Vaccines". Clinical Infectious Diseases. doi:10.1093/cid/ciab068. PMC 7929065. PMID 33502467.
- ^ Epperly, David (January 2021). "Evidence For COVID-19 Vaccine Deferred Dose 2 Boost Timing". SSRN 3760833.
- ^ Wang X (February 2021). "Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine". N Engl J Med (letter). 384 (11): 1576–78. doi:10.1056/NEJMc2036242. PMID 33596350.
- ^ "More Evidence: Evidence For COVID-19 Vaccine Deferred Dose 2 Boost Timing". ReallyCorrect.com.
- ^ "COVID-19: ricerca e vaccini" (in Italian). Europa (web portal). Retrieved 15 February 2021.
- ^ Azar A (4 February 2020). "Notice of Declaration under the Public Readiness and Emergency Preparedness Act for medical countermeasures against COVID-19". Archived from the original on 25 April 2020. Retrieved 22 April 2020.
- ^ "Fourth Amendment to the Declaration Under the Public Readiness and Emergency Preparedness Act for Medical Countermeasures Against COVID–19 and Republication of the Declaration". phe.gov. Retrieved 12 December 2020.
- ^ "AstraZeneca coronavirus vaccine safe, 70% effective, study suggests". Associated Press. 8 December 2020. Retrieved 8 December 2020.
- ^ a b c d Siemieniuk, Reed AC; Bartoszko, Jessica J; Ge, Long; Zeraatkar, Dena; Izcovich, Ariel; Kum, Elena; Pardo-Hernandez, Hector; Rochwerg, Bram; Lamontagne, Francois; Han, Mi Ah; Liu, Qin; Agarwal, Arnav; Agoritsas, Thomas; Chu, Derek K; Couban, Rachel; Darzi, Andrea; Devji, Tahira; Fang, Bo; Fang, Carmen; Flottorp, Signe Agnes; Foroutan, Farid; Ghadimi, Maryam; Heels-Ansdell, Diane; Honarmand, Kimia; Hou, Liangying; Hou, Xiaorong; Ibrahim, Quazi; Khamis, Assem; Lam, Bonnie; Loeb, Mark; Marcucci, Maura; McLeod, Shelley L; Motaghi, Sharhzad; Murthy, Srinivas; Mustafa, Reem A; Neary, John D; Qasim, Anila; Rada, Gabriel; Riaz, Irbaz Bin; Sadeghirad, Behnam; Sekercioglu, Nigar; Sheng, Lulu; Sreekanta, Ashwini; Switzer, Charlotte; Tendal, Britta; Thabane, Lehana; Tomlinson, George; Turner, Tari; Vandvik, Per O; Vernooij, Robin WM; Viteri-García, Andrés; Wang, Ying; Yao, Liang; Ye, Zhikang; Guyatt, Gordon H; Brignardello-Petersen, Romina (30 July 2020). "Drug treatments for covid-19: living systematic review and network meta-analysis". BMJ. 370: m2980. doi:10.1136/bmj.m2980. ISSN 1756-1833. PMC 7390912. PMID 32732190.
- ^ a b "Coronavirus". WebMD. Archived from the original on 1 February 2020. Retrieved 1 February 2020.
- ^ Fisher D, Heymann D (February 2020). "Q&A: The novel coronavirus outbreak causing COVID-19". BMC Medicine. 18 (1): 57. doi:10.1186/s12916-020-01533-w. PMC 7047369. PMID 32106852.
- ^ Liu K, Fang YY, Deng Y, Liu W, Wang MF, Ma JP, et al. (May 2020). "Clinical characteristics of novel coronavirus cases in tertiary hospitals in Hubei Province". Chinese Medical Journal. 133 (9): 1025–1031. doi:10.1097/CM9.0000000000000744. PMC 7147277. PMID 32044814.
- ^ Wang T, Du Z, Zhu F, Cao Z, An Y, Gao Y, Jiang B (March 2020). "Comorbidities and multi-organ injuries in the treatment of COVID-19". Lancet. Elsevier BV. 395 (10228): e52. doi:10.1016/s0140-6736(20)30558-4. PMC 7270177. PMID 32171074.
- ^ Islam, Md Asiful (6 April 2021). "Prevalence and characteristics of fever in adult and paediatric patients with coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis of 17515 patients". PLOS ONE. 16 (4): e0249788. Bibcode:2021PLoSO..1649788I. doi:10.1371/journal.pone.0249788. PMC 8023501. PMID 33822812. S2CID 233173405 – via PLOS.
- ^ Wang Y, Wang Y, Chen Y, Qin Q (March 2020). "Unique epidemiological and clinical features of the emerging 2019 novel coronavirus pneumonia (COVID-19) implicate special control measures". Journal of Medical Virology. 92 (6): 568–576. doi:10.1002/jmv.25748. PMC 7228347. PMID 32134116.
- ^ Martel J, Ko YF, Young JD, Ojcius DM (May 2020). "Could nasal nitric oxide help to mitigate the severity of COVID-19?". Microbes and Infection. 22 (4–5): 168–171. doi:10.1016/j.micinf.2020.05.002. PMC 7200356. PMID 32387333.
- ^ "Coronavirus recovery: breathing exercises". hopkinsmedicine.org. Johns Hopkins Medicine. Retrieved 30 July 2020.
- ^ Wang L, Wang Y, Ye D, Liu Q (March 2020). "Review of the 2019 novel coronavirus (SARS-CoV-2) based on current evidence". International Journal of Antimicrobial Agents. 55 (6): 105948. doi:10.1016/j.ijantimicag.2020.105948. PMC 7156162. PMID 32201353.
- ^ "What to Do if You Are Sick". Centers for Disease Control and Prevention (CDC). 5 April 2020. Archived from the original on 14 February 2020. Retrieved 24 April 2020.
- ^ "Update to living WHO guideline on drugs for covid-19". BMJ. 371: m4475. 19 November 2020. doi:10.1136/bmj.m4475. PMID 33214213. S2CID 227059995.
- ^ "Q&A: Dexamethasone and COVID-19". World Health Organization. Retrieved 11 July 2020.
- ^ "Home". National COVID-19 Clinical Evidence Taskforce. Retrieved 11 July 2020.
- ^ "COVID-19 Treatment Guidelines". nih.gov. National Institutes of Health. Retrieved 18 January 2021.
- ^ Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, et al. (April 2020). "Clinical Characteristics of Coronavirus Disease 2019 in China". The New England Journal of Medicine. Massachusetts Medical Society. 382 (18): 1708–1720. doi:10.1056/nejmoa2002032. PMC 7092819. PMID 32109013.
- ^ Henry BM (April 2020). "COVID-19, ECMO, and lymphopenia: a word of caution". The Lancet. Respiratory Medicine. Elsevier BV. 8 (4): e24. doi:10.1016/s2213-2600(20)30119-3. PMC 7118650. PMID 32178774.
- ^ a b Kim, Peter S.; Read, Sarah W.; Fauci, Anthony S. (1 December 2020). "Therapy for Early COVID-19". JAMA. American Medical Association (AMA). 324 (21): 2149–2150. doi:10.1001/jama.2020.22813. ISSN 0098-7484. PMID 33175121. S2CID 226301949.
- ^ a b c "COVID-19 Treatment Guidelines". nih.gov. National Institutes of Health. Retrieved 18 January 2021./
- ^ Hsu, Jeremy (19 November 2020). "Covid-19: What now for remdesivir?". BMJ. 371: m4457. doi:10.1136/bmj.m4457. ISSN 1756-1833. PMID 33214186. S2CID 227060756.
- ^ "Cases, Data, and Surveillance". Centers for Disease Control and Prevention. 11 February 2020. Retrieved 11 February 2021.
- ^ "Infographic: Mutation of SARS-CoV-2 – current variants of concern". European Centre for Disease Prevention and Control. 19 April 2021. Retrieved 3 May 2021.
- ^ Roser M, Ritchie H, Ortiz-Ospina E (4 March 2020). "Coronavirus Disease (COVID-19)". Our World in Data. Archived from the original on 19 March 2020. Retrieved 12 March 2020.
- ^ Doshi P (October 2020). "Will covid-19 vaccines save lives? Current trials aren't designed to tell us". BMJ. 371: m4037. doi:10.1136/bmj.m4037. PMID 33087398. S2CID 224817161.
- ^ Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19) (PDF) (Report). World Health Organization (WHO). February 2020. Archived (PDF) from the original on 29 February 2020. Retrieved 21 March 2020. Lay summary.
- ^ Palmieri L, Andrianou X, Barbariol P, Bella A, Bellino S, Benelli E, et al. (22 July 2020). Characteristics of SARS-CoV-2 patients dying in Italy Report based on available data on July 22nd, 2020 (PDF) (Report). Istituto Superiore di Sanità. Retrieved 4 October 2020.
- ^ Baranovskii DS, Klabukov ID, Krasilnikova OA, Nikogosov DA, Polekhina NV, Baranovskaia DR, et al. (December 1975). "Letter: Acid secretion by gastric mucous membrane". The American Journal of Physiology. 229 (6): 21–25. doi:10.1080/03007995.2020.1853510. PMC 7738209. PMID 33210948. S2CID 227065216.
- ^ Christensen B, Favaloro EJ, Lippi G, Van Cott EM (October 2020). "Hematology Laboratory Abnormalities in Patients with Coronavirus Disease 2019 (COVID-19)". Seminars in Thrombosis and Hemostasis. 46 (7): 845–849. doi:10.1055/s-0040-1715458. PMC 7645834. PMID 32877961.
- ^ Cirillo, Pasquale and Nassim Nicholas Taleb (2020). "Tail Risk of Contagious Diseases". Nature Physics. 16 (6): 606–613. arXiv:2004.08658. Bibcode:2020NatPh..16..606C. doi:10.1038/s41567-020-0921-x. S2CID 215828381.
- ^ a b c Anderson RM, Heesterbeek H, Klinkenberg D, Hollingsworth TD (March 2020). "How will country-based mitigation measures influence the course of the COVID-19 epidemic?". Lancet. 395 (10228): 931–934. doi:10.1016/S0140-6736(20)30567-5. PMC 7158572. PMID 32164834.
A key issue for epidemiologists is helping policy makers decide the main objectives of mitigation—e.g. minimising morbidity and associated mortality, avoiding an epidemic peak that overwhelms health-care services, keeping the effects on the economy within manageable levels, and flattening the epidemic curve to wait for vaccine development and manufacture on scale and antiviral drug therapies.
- ^ Qualls N, Levitt A, Kanade N, Wright-Jegede N, Dopson S, Biggerstaff M, et al. (April 2017). "Community Mitigation Guidelines to Prevent Pandemic Influenza – United States, 2017". MMWR. Recommendations and Reports. 66 (1): 1–34. doi:10.15585/mmwr.rr6601a1. PMC 5837128. PMID 28426646.
- ^ Barclay E, Scott D, Animashaun A (7 April 2020). "The US doesn't just need to flatten the curve. It needs to "raise the line."". Vox. Archived from the original on 7 April 2020.
- ^ "Fever Screening | IntelliSEC | Durban, Johannesburg, Cape Town". IntelliSEC.
- ^ Baird RP (11 March 2020). "What It Means to Contain and Mitigate the Coronavirus". The New Yorker.
- ^ a b "Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand" (PDF). Imperial College COVID-19 Response Team. 16 March 2020.
- ^ "Community Mitigation Guidelines to Prevent Pandemic Influenza – United States, 2017". Recommendations and Reports. 66 (1). 12 April 2017.
- ^ Thompson, Derek (27 July 2020). "Hygiene Theater Is a Huge Waste of Time". The Atlantic. Archived from the original on 26 April 2021. Retrieved 22 February 2021.
- ^ Qin, Amy (7 March 2020). "China May Be Beating the Coronavirus, at a Painful Cost". The New York Times.
- ^ McCurry J, Ratcliffe R, Davidson H (11 March 2020). "Mass testing, alerts and big fines: the strategies used in Asia to slow coronavirus". The Guardian.
- ^ "Expert interview: What is contact tracing?". Blog: Public Health Matters. Public Health England, Government of the United Kingdom. Retrieved 28 February 2020.
- ^ a b c Ingram D, Ward J (7 April 2020). "Behind the global efforts to make a privacy-first coronavirus tracking app". NBC News. Retrieved 10 April 2020.
- ^ "Apple and Google are launching a joint COVID-19 tracing tool for iOS and Android". TechCrunch. Retrieved 10 April 2020.
- ^ "Privacy-Preserving Contact Tracing". Apple. 10 April 2020.
- ^ "Apple and Google partner on COVID-19 contact tracing technology". 10 April 2020. Retrieved 10 April 2020.
- ^ "Palantir provides COVID-19 tracking software to CDC and NHS, pitches European health agencies". TechCrunch. Retrieved 22 April 2020.
- ^ a b "Hospital readiness checklist for COVID-19". World Health Organization. 25 March 2020. Retrieved 27 March 2020.
- ^ Checklist for hospitals preparing for the reception and care of coronavirus 2019 (COVID-19) patients (Report). European Centre for Disease Prevention and Control. 26 February 2020. Retrieved 27 March 2020.
- ^ Smith, Anthony C; Thomas, Emma; Snoswell, Centaine L; Haydon, Helen; Mehrotra, Ateev; Clemensen, Jane; Caffery, Liam J (20 March 2020). "Telehealth for global emergencies: Implications for coronavirus disease 2019 (COVID-19)". Journal of Telemedicine and Telecare. 26 (5): 309–313. doi:10.1177/1357633x20916567. PMC 7140977. PMID 32196391.
- ^ Ohannessian, R; Duong, TA; Odone, A (2 April 2020). "Global Telemedicine Implementation and Integration Within Health Systems to Fight the COVID-19 Pandemic: A Call to Action". JMIR Public Health and Surveillance. 6 (2): e18810. doi:10.2196/18810. PMC 7124951. PMID 32238336.
- ^ Keshvardoost, Sareh; Bahaadinbeigy, Kambiz; Fatehi, Farhad (23 April 2020). "Role of Telehealth in the Management of COVID-19: Lessons Learned from Previous SARS, MERS, and Ebola Outbreaks". Telemedicine and E-Health. 26 (7): 850–852. doi:10.1089/tmj.2020.0105. PMID 32329659. S2CID 216111135.
- ^ Temple J. "How 3D printing could save lives in the coronavirus outbreak". MIT Technology Review. Retrieved 5 April 2020.
- ^ Tibken S. "3D printing may help supply more essential coronavirus medical gear". CNET. Retrieved 5 April 2020.
- ^ "[Updating] Italian hospital saves Covid-19 patients lives by 3D printing valves for reanimation devices". 3D Printing Media Network. 14 March 2020. Retrieved 20 March 2020.
- ^ Peters J (17 March 2020). "Volunteers produce 3D-printed valves for life-saving coronavirus treatments". The Verge. Retrieved 20 March 2020.
- ^ "Engineers 3D-print patented valves for free to save coronavirus patients in Italy". Global News.
- ^ Good A, Greicius T (23 April 2020). "NASA Develops COVID-19 Prototype Ventilator in 37 Days". NASA. Retrieved 24 April 2020.
- ^ Wall M (24 April 2020). "NASA engineers build new COVID-19 ventilator in 37 days". Space.com. Retrieved 24 April 2020.
- ^ Ma J (13 March 2020). "China's first confirmed Covid-19 case traced back to November 17". South China Morning Post. Archived from the original on 13 March 2020.
- ^ Gao, Yu (高昱) (26 February 2020). 独家 | 新冠病毒基因测序溯源:警报是何时拉响的 [Exclusive | Tracing the New Coronavirus gene sequencing: when did the alarm sound]. Caixin (in Chinese). Archived from the original on 27 February 2020. Retrieved 1 March 2020.
- ^ "China delayed releasing coronavirus info, frustrating WHO". AP NEWS. 2 June 2020.
- ^ Lu, Zikang (路子康). 最早上报疫情的她,怎样发现这种不一样的肺炎. 中国网新闻 (in Chinese). Beijing. Archived from the original on 2 March 2020. Retrieved 11 February 2020.
- ^ "'Hero who told the truth': Chinese rage over coronavirus death of whistleblower doctor". The Guardian. 7 February 2020.
- ^ Kuo L (11 March 2020). "Coronavirus: Wuhan doctor speaks out against authorities". The Guardian. London.
- ^ "Undiagnosed pneumonia – China (HU): RFI". ProMED Mail. ProMED. Retrieved 7 May 2020.
- ^ a b "Novel Coronavirus". World Health Organization (WHO). Archived from the original on 22 January 2020. Retrieved 6 February 2020.
"COVID-19 timeline in the Western Pacific". WHO. 18 May 2020. Archived from the original on 23 May 2020. Retrieved 6 July 2020. - ^ 武汉现不明原因肺炎 官方确认属实:已经做好隔离. Xinhua News. 31 December 2019. Retrieved 31 March 2020 – via 163.com.
- ^ 武汉市卫健委关于当前我市肺炎疫情的情况通报. WJW.Wuhan.gov.cn (in Chinese). Wuhan Municipal Health Commission. 31 December 2019. Archived from the original on 9 January 2020. Retrieved 8 February 2020.
- ^ a b "Mystery pneumonia virus probed in China". BBC News. 3 January 2020. Archived from the original on 5 January 2020. Retrieved 29 January 2020.
- ^ a b "Novel Coronavirus (2019-nCoV) SITUATION REPORT – 1" (PDF). World Health Organization. 20 January 2020. Retrieved 7 June 2021.
- ^ Novel Coronavirus Pneumonia Emergency Response Epidemiology Team (February 2020). "[The epidemiological characteristics of an outbreak of 2019 novel coronavirus diseases (COVID-19) in China]". Zhonghua Liu Xing Bing Xue Za Zhi – Zhonghua Liuxingbingxue Zazhi (in Chinese). 41 (2): 145–151. doi:10.3760/cma.j.issn.0254-6450.2020.02.003. PMID 32064853. S2CID 211133882.
- ^ Areddy, James T. (26 May 2020). "China Rules Out Animal Market and Lab as Coronavirus Origin". The Wall Street Journal. Retrieved 29 May 2020.
- ^ "WHO-convened global study of origins of SARS-CoV-2: China Part". World Health Organization. Retrieved 31 March 2021.
- ^ Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. (March 2020). "Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia". The New England Journal of Medicine. 382 (13): 1199–1207. doi:10.1056/NEJMoa2001316. PMC 7121484. PMID 31995857.
- ^ WHO–China Joint Mission (24 February 2020). "Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19)" (PDF). World Health Organization (WHO). Retrieved 8 March 2020.
- ^ Padilla, Teodoro (24 February 2021). "No one is safe unless everyone is safe". BusinessWorld. Retrieved 24 February 2021.
- ^ "China confirms sharp rise in cases of SARS-like virus across the country". 20 January 2020. Archived from the original on 20 January 2020. Retrieved 20 January 2020.
- ^ The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team (17 February 2020). "The Epidemiological Characteristics of an Outbreak of 2019 Novel Coronavirus Diseases (COVID-19) – China, 2020". China CDC Weekly. 2 (8): 113–122. doi:10.46234/ccdcw2020.032. Retrieved 18 March 2020.
- ^ "Flattery and foot dragging: China's influence over the WHO under scrutiny". The Globe and Mail. 25 April 2020.
- ^ Horton, Richard (18 March 2020). "Scientists have been sounding the alarm on coronavirus for months. Why did Britain fail to act?". The Guardian. Retrieved 23 April 2020.
- ^ Wu JT, Leung K, Leung GM (2020). "Nowcasting and forecasting the potential domestic and international spread of the 2019-nCoV outbreak originating in Wuhan, China: a modelling study". Lancet. 395 (10225): 689–697. doi:10.1016/S0140-6736(20)30260-9. PMC 7159271. PMID 32014114.
- ^ "Novel Coronavirus(2019-nCoV): Situation Report – 10" (PDF). World Health Organization (WHO). 30 January 2020. Retrieved 14 October 2020.
- ^ "Statement on the second meeting of the International Health Regulations (2005) Emergency Committee regarding the outbreak of novel coronavirus (2019-nCoV)". World Health Organization (WHO). 30 January 2020. Archived from the original on 31 January 2020. Retrieved 30 January 2020.
- ^ "Coronavirus disease 2019 (COVID-19): Situation Report – 51" (PDF). World Health Organization (WHO). 11 March 2020. Retrieved 14 October 2020.
- ^ "WHO Director-General's opening remarks at the media briefing on COVID-19". World Health Organization (WHO). 11 March 2020. Retrieved 11 March 2020.
- ^ a b "Coronavirus: Primi due casi in Italia" [Coronavirus: First two cases in Italy]. Corriere della sera (in Italian). 31 January 2020. Retrieved 31 January 2020.
- ^ "Coronavirus: Number of COVID-19 deaths in Italy surpasses China as total reaches 3,405". Sky News. Retrieved 7 May 2020.
- ^ McNeil Jr DG (26 March 2020). "The U.S. Now Leads the World in Confirmed Coronavirus Cases". The New York Times. Retrieved 27 March 2020.
- ^ "Studies Show N.Y. Outbreak Originated in Europe". The New York Times. 8 April 2020.
- ^ a b Irish J (4 May 2020). Lough R, Graff P (eds.). "After retesting samples, French hospital discovers COVID-19 case from December". Reuters. Retrieved 4 May 2020.
- ^ a b Deslandes A, Berti V, Tandjaoui-Lambotte Y, Alloui C, Carbonnelle E, Zahar JR, Brichler S, Cohen Y (3 May 2020). "SARS-COV-2 was already spreading in France in late December 2019". International Journal of Antimicrobial Agents. 55 (6): 106006. doi:10.1016/j.ijantimicag.2020.106006. PMC 7196402. PMID 32371096.
- ^ "2 died with coronavirus weeks before 1st U.S. virus death". PBS NewsHour. 22 April 2020. Retrieved 23 April 2020.
- ^ a b "Beijing Covid-19 outbreak puts food markets back in infection focus". South China Morning Post. 16 June 2020. Archived from the original on 16 June 2020. Retrieved 17 June 2020.
- ^ "北京连续确诊3例新冠患者 新发地批发市场暂停营业". Caixin. Archived from the original on 13 June 2020. Retrieved 17 June 2020.
- ^ Gan, Nectar (15 June 2020). "China's new coronavirus outbreak sees Beijing adopt 'wartime' measures". CNN. Archived from the original on 16 June 2020. Retrieved 17 June 2020.
- ^ "Beijing logs record 36 COVID-19 cases, linked to market cluster". CNA. Retrieved 17 June 2020.
- ^ Kim, Will Feuer, Jasmine (29 June 2020). "WHO warns coronavirus pandemic is speeding up as countries ease lockdown rules: 'The worst is yet to come'". CNBC. Retrieved 5 July 2020.
- ^ "More cases of COVID-19 linked to employee at Dalian seafood processor". Undercurrent News. Retrieved 4 August 2020.
- ^ "One in 10 worldwide may have had Covid – WHO". BBC. 5 October 2020. Retrieved 14 October 2020.
- ^ "WHO | SARS-CoV-2 mink-associated variant strain – Denmark". WHO.
- ^ "Denmark to cull up to 17 million mink amid coronavirus fears". BBC News. 5 November 2020.
- ^ Boseley, Sarah; Oltermann, and Philip (9 November 2020). "Covid-19 vaccine candidate is 90% effective, says Pfizer". The Guardian. ISSN 0261-3077. Retrieved 9 November 2020.
- ^ Linnane, Ciara. "Novavax wins FDA fast track designation for COVID-19 vaccine candidate". MarketWatch. Retrieved 9 November 2020.
- ^ "Pfizer says COVID-19 vaccine is looking 90% effective". AP NEWS. 9 November 2020. Retrieved 9 November 2020.
- ^ Rosenberg, Benjamin (8 November 2020). "50 million world Covid-19 cases: The biggest outbreaks, explained". Vox. Retrieved 11 November 2020.
- ^ Reese, Heather; Iuliano, A. Danielle; Patel, Neha N.; Garg, Shikha; Kim, Lindsay; Silk, Benjamin J.; Hall, Aron J.; Fry, Alicia; Reed, Carrie (2020). "Estimated incidence of COVID-19 illness and hospitalization – United States, February–September, 2020". Clinical Infectious Diseases. doi:10.1093/cid/ciaa1780. PMC 7717219. PMID 33237993. S2CID 227176624.
- ^ "Government Model Suggests U.S. COVID-19 Cases Could Be Approaching 100 Million". NPR. Retrieved 27 November 2020.
- ^ "PHE investigating a novel strain of COVID-19". GOV.UK. 14 December 2020. Retrieved 15 December 2020.
- ^ "Covid: Flights shut down as EU discusses UK virus threat". BBC News. 21 December 2020.
- ^ "Covid-19: Drivers urged to avoid ports as France shuts border". BBC News. 21 December 2020.
- ^ Hauck, Grace. "More contagious COVID-19 strain identified in 3 states and 33 countries: What to know". USA Today. Retrieved 2 January 2021.
- ^ "Genomic characterisation of an emergent SARS-CoV-2 lineage in Manaus: preliminary findings". Virological. 12 January 2021. Retrieved 6 May 2021.
- ^ "WHO's Covid mission to Wuhan: 'It's not about finding China guilty'". The Guardian. 12 January 2021. Retrieved 14 January 2021.
- ^ Kuo, Lily. "China bars two members of WHO coronavirus mission as depleted team reaches Wuhan". The Washington Post. Retrieved 15 January 2021.
- ^ Nedelman, Michael. "South Carolina detects first US cases of coronavirus strain first seen in South Africa". CNN. Retrieved 29 January 2021.
- ^ Johnson, Carolyn Y. "Novavax vaccine protects against coronavirus in variant hot spots but proved less effective against strain in South Africa". The Washington Post. Retrieved 29 January 2021.
- ^ "COVID variants test immunity, NIH chief and China's mixed vaccine data". Nature. 589 (7843): 497. 27 January 2021. Bibcode:2021Natur.589..497.. doi:10.1038/d41586-021-00186-w. Retrieved 29 January 2021.
- ^ "AstraZeneca defends COVID vaccine as handful of nations pause use over fear of blood clots". CBS News. Retrieved 14 March 2021.
- ^ "WHO renews backing for AstraZeneca's COVID-19 jab as European countries resume vaccinations". SBS News. 20 March 2021. Retrieved 21 March 2021.
- ^ Diamond, Dan; Sun, Lena H.; Stanley-Becker, Isaac. "'Vaccine passports' are on the way, but developing them won't be easy". The Washington Post. Retrieved 29 March 2021.
- ^ "Schengen Area Crisis: EU States Close Borders as Coronavirus Outbreak Grips Bloc". Schengen Visa Information. 13 March 2020. Retrieved 16 March 2020.
- ^ "Coronavirus: 7 dead, 229 infected in Italy as Europe braces for COVID-19". NBC News. Retrieved 29 February 2020.
- ^ Doyle, Michael (11 October 2020). "WHO doctor says lockdowns should not be main coronavirus defence". ABC. Retrieved 25 October 2020.
- ^ Jones S, Kassam A (26 March 2020). "Spain defends response to coronavirus as global cases exceed 500,000". The Guardian. Retrieved 29 March 2020.
- ^ "Coronavirus: Half of humanity now on lockdown as 90 countries call for confinement". Euronews. 3 April 2020.
- ^ "A third of the global population is on coronavirus lockdown – here's our constantly updated list of countries and restrictions". Business Insider. 28 March 2020.
- ^ a b "What Share of the World Population Is Already on COVID-19 Lockdown?". Statista. 23 April 2020. Retrieved 26 April 2020.
- ^ "About 90% of Americans have been ordered to stay at home. This map shows which cities and states are under lockdown". Business Insider. 2 April 2020.
- ^ Chutel L, Dahir AL (27 March 2020). "With Most Coronavirus Cases in Africa, South Africa Locks Down". The New York Times. Retrieved 2 April 2020.
- ^ Nair S (29 March 2020). "For a billion Indians, lockdown has not prevented tragedy". The Guardian.
- ^ "Chaos and hunger amid India coronavirus lockdown". Al Jazeera. 27 March 2020.
- ^ Pirnazarov, Nazarali (30 April 2020). "UPDATE 1-Tajikistan confirms first coronavirus cases". Reuters. Retrieved 29 October 2020.
- ^ Abdurasulov A (7 April 2020). "Coronavirus: Why has Turkmenistan reported no cases?". BBC News.
- ^ Tan Y (3 April 2020). "Scepticism over N Korea's claim to be virus free". BBC News.
- ^ Drexler, Madeline. "The Unlikeliest Pandemic Success Story". The Atlantic. ISSN 1072-7825. Retrieved 13 February 2021.
- ^ "Why is Singapore's COVID-19 death rate the world's lowest". Reuters. Archived from the original on 3 October 2020. Retrieved 21 May 2021.
- ^ "Singapore Is Now the World's Best Place to Be During Covid". Bloomberg. Retrieved 21 May 2021.
- ^ Chan, Wilfred (3 April 2020). "The WHO Ignores Taiwan. The World Pays the Price". The Nation. Retrieved 24 May 2020.
- ^ Humphrey, Chris; Pham, Bac (14 April 2020). "Vietnam's response to coronavirus crisis earns praise from WHO". 7News. Retrieved 17 April 2020.
- ^ a b Burki, Talha (1 November 2020). "China's successful control of COVID-19". The Lancet Infectious Diseases. 20 (11): 1240–1241. doi:10.1016/S1473-3099(20)30800-8. ISSN 1473-3099. PMC 7544475. PMID 33038941.
- ^ Hessler, Peter. "How China Controlled the Coronavirus". The New Yorker. Retrieved 4 January 2021.
- ^ "China's response shows how bold decision-making can contain coronavirus". World Economic Forum. Retrieved 4 January 2021.
- ^ Kupferschmidt, Kai; Cohen, Jon (2 March 2020). "China's aggressive measures have slowed the coronavirus. They may not work in other countries". Science | AAAS. Retrieved 4 January 2021.
- ^ Rambaran, Vandana (28 November 2020). "More people died of suicide in Japan in one month than the entire coronavirus pandemic". Fox News. Retrieved 29 November 2020.
- ^ 截至6月14日24时新型冠状病毒肺炎疫情最新情况 (in Chinese). National Health Commission. 26 June 2020. Retrieved 5 September 2020.
31个省(自治区、直辖市)和新疆生产建设兵团报告新增无症状感染者18例(境外输入11例);当日无转为确诊病例;当日解除医学观察9例(境外输入2例);尚在医学观察无症状感染者112例(境外输入62例)。
- ^ 新型肺炎疫情地圖 實時更新 [New pneumonia epidemic map updated in real time]. 163.com news (in Chinese). 29 January 2020. Archived from the original on 30 January 2020. Retrieved 2 February 2020.
- ^ migration (13 October 2020). "Minor outbreak sparks mass testing in city". The Straits Times. Retrieved 4 January 2021.
- ^ Pike, Lili (25 November 2020). "In China, nearly 1 million people have reportedly already gotten a coronavirus vaccine". Vox. Retrieved 26 November 2020.
- ^ Gettleman, Jeffrey; Schultz, Kai (24 March 2020). "Modi Orders 3-Week Total Lockdown for All 1.3 Billion Indians". The New York Times. ISSN 0362-4331. Retrieved 2 August 2020.
- ^ "Infections over 1 lakh, five cities with half the cases: India's coronavirus story so far". The Week. Retrieved 20 May 2020.
- ^ "Covid-19: Number of recoveries exceed active cases for first time". Hindustan Times. 10 June 2020. Retrieved 2 August 2020.
- ^ "Coronavirus: India surpasses US for highest single-day rise in Covid-19 cases". BBC News. 30 August 2020. Retrieved 29 September 2020.
- ^ Hollingsworth, Julia; Renton, Adam; Wagner, Meg; Rahim, Zamira; Upright, Ed (17 September 2020). "India reports nearly 98,000 new Covid-19 cases in highest worldwide daily spike". CNN. Retrieved 12 December 2020.
- ^ "Another grim milestone: India No.3 in total coronavirus cases". Hindustan Times. 6 July 2020. Retrieved 6 July 2020.
- ^ "India most infected by Covid-19 among Asian countries, leaves Turkey behind". Hindustan Times. 29 May 2020. Retrieved 30 May 2020.
- ^ "One in four Indians could have been infected with the coronavirus, lab head says". MSN. 19 August 2020. Retrieved 19 August 2020.
- ^ Kashyap, Simran (6 September 2020). "COVID-19: With over 4 million cases, India overtakes Brazil to become second worst-hit nation". Oneindia. Retrieved 23 September 2020.
- ^ "India's case count crosses 100,000, Delhi eases restrictions: Covid-19 news today". Hindustan Times. 19 May 2020. Retrieved 20 May 2020.
- ^ "India Coronavirus Cases Surge Past One Million". The New York Times. 16 July 2020. Retrieved 29 September 2020.
- ^ "India's coronavirus infections top five million mark". BBC News. 16 September 2020. Retrieved 29 September 2020.
- ^ Jamkhandikar, Shilpa (19 December 2020). "India hits 10 million coronavirus cases but pace slows". Reuters. Retrieved 21 February 2021.
- ^ Agrawal M, Kanitkar M, Vidyasagar M (October 2020). "Modelling the spread of SARS-CoV-2 pandemic – Impact of lockdowns & interventions". Indian Journal of Medical Research. 153 (1 & 2): 175–18. doi:10.4103/ijmr.IJMR_4051_20 (inactive 6 May 2021). PMID 33146155.CS1 maint: DOI inactive as of May 2021 (link)
- ^ National Supermodel Committee. "Indian Supermodel for Covid-19 Pandemic" (PDF).
- ^ Super Model Committee. "National Supermodel of COVID-19 with Projections" (PDF).
- ^ "DST initiates COVID-19 India National Supermodel for monitoring infection transmission & aid decision-making by policymakers". Government of India, Ministry of Science and Technology.
- ^ Jessie Yeung and Vedika Sud. "India's second Covid wave hits like a 'tsunami' as hospitals buckle under weight". CNN. Retrieved 26 April 2021.
- ^ Gettleman, Jeffrey; Yasir, Sameer; Kumar, Hari; Raj, Suhasini; Loke, Atul (24 April 2021). "As Covid-19 Devastates India, Deaths Go Undercounted". The New York Times. Retrieved 26 April 2021.
- ^ "Realizan jornada de limpieza en vagones del Metro de Panamá". Tvn-2.com. 12 March 2020. Retrieved 23 April 2020.
- ^ "Coronavirus Arrives in Iran: Two People Test Positive in Qom". IranGov.ir. Government of Iran. 19 February 2020. Retrieved 6 March 2020.
- ^ "Iran Confirms 3 New Coronavirus Cases". IranGov.ir. Government of Iran. 20 February 2020. Retrieved 6 March 2020.
- ^ "Iranian Doctors Call For 'Long Holiday' To Contain Coronavirus, As Sixth Victim Dies". Radio Farda. Radio Free Europe/Radio Liberty. 22 February 2020. Retrieved 8 March 2020.
- ^ لغو همه مسابقات ورزشی به مدت ۱۰ روز. Varzesh3.com (in Persian). Retrieved 23 February 2020.
- ^ a b Gambrell J. "Iran news agencies report Friday prayers canceled in Tehran". The Washington Post. Associated Press.
- ^ "Iran Announces Closure Of Universities, Schools As Coronavirus Death Toll Rises". Radio Farda. Radio Free Europe/Radio Liberty. 23 February 2020. Retrieved 8 March 2020.
- ^ اختصاص 530 میلیارد تومان به وزارت بهداشت برای مقابله با کرونا. پایگاه خبری جماران—امام خمینی—انقلاب اسلامی (in Persian). Retrieved 23 February 2020.
- ^ "Coronavirus: Iran has no plans to quarantine cities, Rouhani says". BBC News. 26 February 2020.
- ^ Jones S, Wintour P (6 March 2020). "Iran threatens use of force to restrict spread of coronavirus". The Guardian.
- ^ "Coronavirus: Iran is facing a major challenge controlling the outbreak". BBC News. 24 March 2020.
- ^ Mostaghim R, Salem M, Qiblawi T (26 February 2020). "Iran was already struggling with one crisis. Now it has the worst coronavirus outbreak in the Middle East". CNN.
- ^ a b Gambrell A J (17 March 2020). "Shiite Hardliners in Iran Storm 2 Shrines That Were Closed to Stop Coronavirus Spread". Time. Associated Press.
- ^ Kirkpatrick, David D.; Fassihi, Farnaz; Mashal, Mujib (24 February 2020). "'Recipe for a Massive Viral Outbreak': Iran Emerges as a Worldwide Threat". The New York Times.
- ^ a b Wright R (24 February 2020). "How Iran Became A New Epicenter of the Coronavirus Outbreak". The New Yorker.
- ^ a b Cunningham E, Bennett D (4 March 2020). "Coronavirus pummels Iran leadership as data show spread is far worse than reported". The Washington Post.
- ^ Haltiwanger J (3 March 2020). "8% of Iran's parliament has the coronavirus, and it released 54,000 prisoners as the country descends into chaos". Business Insider. Retrieved 4 March 2020.
- ^ Sorace S (15 March 2020). "Iran reports biggest single-day jump of coronavirus deaths as president rules out quarantine". Fox News. Retrieved 16 March 2020.
- ^ "Coronavirus pandemic 'could kill millions' in Iran". Al Jazeera. 17 March 2020.
- ^ Lauras, Didier (23 March 2020). "How serious is the coronavirus crisis in Iran?". Yahoo! News. Agence France-Presse. Retrieved 23 March 2020.
- ^ "As coronavirus cases explode in Iran, U.S. sanctions hinder its access to drugs and medical equipment". The Washington Post. Retrieved 29 March 2020.
- ^ "Iran opens up as economic woes trump virus infection fears". Yahoo! News. Retrieved 21 April 2020.
- ^ "Coronavirus: Iran fears the second wave after surge in cases". BBC. 4 June 2020.
- ^ "Rouhani warns 25 million infected as Iran reimposes restrictions". Reuters. 18 July 2020.
- ^ "Coronavirus: Iran cover-up of deaths revealed by data leak". BBC. 3 August 2020.
- ^ a b Shin H, Cha S (20 February 2020). "'Like a zombie apocalypse': Residents on edge as coronavirus cases surge in South Korea". Archived from the original on 20 February 2020. Retrieved 20 February 2020.
- ^ 신천지 관련 확진자 76명으로 늘어 ... 대구 교인 의심자만 544명 [The number of Shincheonji related doctors will increase to 74 ... Daegu members only 544]. Chosun.com (in Korean). 21 February 2020.
- ^ a b "42 Shincheonji followers came to S. Korea from virus-hit Wuhan over 8 months: gov't". Yonhap News Agency. 29 February 2020.
- ^ Lee H (21 February 2020). "COVID-19 patients soar to 204 in Korea". Korea Biomedical Review. Retrieved 21 February 2020.
- ^ 코로나바이러스감염증-19 국내 발생 현황 (2월 22일 09시). 22 February 2020.
- ^ "Coronavirus: South Korea declares highest alert as infections surge". BBC News. 23 February 2020.
- ^ Hoffmann E (29 February 2020). "South Korea reports a record jump in coronavirus cases". SeekingAlpha.com. Retrieved 1 March 2020.
- ^ "Airlines to suspend more flights over coronavirus". The Korea Herald. Yonhap. 21 February 2020. Retrieved 21 February 2020.
- ^ Song S (21 February 2020). "Foreign artists delay concerts in Korea due to spread of COVID-19". The Korea Herald. Retrieved 21 February 2020.
- ^ a b Normile D (17 March 2020). "Coronavirus cases have dropped sharply in South Korea. What's the secret to its success?". Science. doi:10.1126/science.abb7566. S2CID 216427938.
- ^ Bicker L (12 March 2020). "Coronavirus in South Korea: How 'trace, test and treat' may be saving lives". BBC News.
- ^ Moon G. "This is how South Korea flattened its coronavirus curve". NBC News. Retrieved 31 March 2020.
- ^ "South Korea's Drive-Through Testing For Coronavirus Is Fast – And Free". NPR. Retrieved 16 March 2020.
- ^ a b "South Korea reports lowest number of new cases". BBC News Online. 23 March 2020. Retrieved 23 March 2020.
- ^ a b Kim S (4 March 2020). "How South Korea Lost Control of Its Coronavirus Outbreak". The New Yorker.
- ^ Kasulis K (19 March 2020). "South Korea's coronavirus lessons: Quick, easy tests; monitoring". Al Jazeera.
- ^ 'K방역 극찬' 빌 게이츠, KT 손잡고 제2 코로나 막을 연구에 60억 투자. 중앙일보 (in Korean). 17 May 2020. Retrieved 17 May 2020.
- ^ "South Korea to impose mandatory coronavirus quarantine on all arrivals". Yahoo! News. Retrieved 29 March 2020.
- ^ "Over 100 Countries Ask South Korea for Coronavirus Testing Help". US News and World Report. Retrieved 1 April 2020.
- ^ "Coronavirus: South Korea confirms second wave of infections". BBC. 22 June 2020.
- ^ "South Korea says it is in the middle of a coronavirus second wave – and it arrived earlier than predicted". ABC News. 22 June 2020.
- ^ Nebehay, Stephanie (13 March 2020). "Europe is epicenter of coronavirus pandemic: WHO". Reuters. Retrieved 8 May 2021.
- ^ "Coronavirus: Europe now epicentre of the pandemic, says WHO". BBC. 13 March 2020. Retrieved 8 May 2021.
- ^ Feuer, Will (22 May 2020). "South America is a 'new epicenter' of the coronavirus pandemic, WHO says".
- ^ @MeGovernment (17 March 2020). "Two COVID-19 cases confirmed in Montenegro" (Tweet). Retrieved 17 March 2020 – via Twitter.
- ^ Henley, Jon (18 March 2020). "More than 250m in lockdown in EU as Belgium and Germany adopt measures". The Guardian. ISSN 0261-3077. Archived from the original on 1 April 2020. Retrieved 4 April 2020.
- ^ Institute for Public Health of Montenegro [@ijzcg] (24 May 2020). "IT'S OFFICIAL: CURRENTLY THERE ARE NO ACTIVE CASES OF #COVID19 IN MONTENEGRO" (Tweet). Retrieved 24 May 2020 – via Twitter.
- ^ Government of Montenegro [@MeGovernment] (24 May 2020). "Montenegro is Corona-Free" (Tweet). Retrieved 24 May 2020 – via Twitter.
- ^ "New imported case discovered". Institute of Public Health of Montenegro IJZCG. Retrieved 21 June 2020 – via Twitter.[non-primary source needed]
- ^ "COVID-19 Map". Johns Hopkins Coronavirus Resource Center.
- ^ Farzan, Antonia Noori; Hassan, Jennifer; Noack, Rick; Beachum, Lateshia; Hawkins, Derek; Bellware, Kim; O'Grady, Siobhán; Shaban, Hamza. "Live updates: Coronavirus cases rise in young people in Europe as U.S. colleges try to crack down on parties". The Washington Post. Retrieved 21 August 2020.
- ^ "Europe Coronavirus Cases Exceed 15 Million | Voice of America – English". Voice of America. Retrieved 25 November 2020.
- ^ "Coronavirus : la " bombe atomique " du rassemblement évangélique de Mulhouse". Le Point. 28 March 2020.
- ^ "Enquette Franceinfo. "La majorité des personnes étaient contaminées" : de la Corse à l'outre-mer, comment le rassemblement évangélique de Mulhouse a diffusé le coronavirus dans toute la France". Franceinfo. 28 March 2020.
- ^ "Coronavirus: Spain and France announce sweeping restrictions". BBC News. 15 March 2020. Retrieved 15 March 2020.
- ^ "France imposes 15-day lockdown as part of emergency coronavirus response". The Independent. 16 March 2020.
- ^ "Coronavirus : prolongation du confinement jusqu'au 11 mai". France Info. 13 April 2020. Retrieved 13 April 2020.
- ^ Macron: coronavirus is Europe's 'moment of truth' 16 April 2020, Financial Times. Retrieved 18 April 2020
- ^ "COVID-19 en France" (in French). Santé Publique France. Retrieved 9 April 2020.
- ^ "Coronavirus Map: Tracking the Global Outbreak". The New York Times. Retrieved 4 April 2020.
- ^ "Violent protests in Paris suburbs reflect tensions under lockdown". The Washington Post. Retrieved 25 April 2020.
- ^ "Coronavirus flare-ups force France to re-close some schools". CBS News. Retrieved 18 May 2020.
- ^ Welle (www.dw.com), Deutsche. "Coronavirus digest: WHO says best way to protest lockdowns is to take other measures seriously | DW | 12 November 2020". Deutsche Welle. Retrieved 13 November 2020.
- ^ "Italy suspends all China flights as coronavirus cases confirmed in Rome". TheLocal.it. 31 January 2020. Retrieved 26 February 2020.
- ^ Anzolin E, Amante A (21 February 2020). "Coronavirus outbreak grows in northern Italy, 16 cases reported in one day". Archived from the original on 21 February 2020. Retrieved 21 February 2020.
- ^ "Coronavirus, in dieci comuni lombardi: 50 mila persone costrette a restare in casa. Quarantena all'ospedale milanese di Baggio". La Repubblica (in Italian). 21 February 2020. Retrieved 23 February 2020.
- ^ "Coronavirus, decreto del governo: nei comuni focolaio stop ad ingressi ed uscite. Conte: "Non trasformeremo l'Italia in un lazzaretto"". la Repubblica (in Italian). 22 February 2020. Retrieved 22 February 2020.
- ^ "Coronavirus: Inter Milan v Sampdoria among Serie A games postponed". BBC Sport. 22 February 2020. Retrieved 23 February 2020.
- ^ Giuffrida A, Tondo L, Beaumont P (4 March 2020). "Italy orders closure of all schools and universities due to coronavirus". The Guardian. Retrieved 4 March 2020.
- ^ "Coronavirus: All sport in Italy suspended because of outbreak". BBC Sport. 9 March 2020.
- ^ Harlan C, Morris L. "Italy ramps up coronavirus lockdown, Merkel warns virus could infect two-thirds of Germany". The Washington Post. Retrieved 12 March 2020.
- ^ Sylvers E, Legorano G (11 March 2020). "Italy Hardens Nationwide Quarantine". The Wall Street Journal. Retrieved 12 March 2020.
- ^ Raccomandazioni di etica clinica per l'ammissione a trattamenti intensivi e per la loro sospensione, in condizioni eccezionali di squilibrio tra necessità e risorse disponibili (PDF) (Technical report) (in Italian). Italian College of Anesthesia, Analgesia, Resuscitation and Intensive Care (SIAARTI). 6 March 2020. Archived from the original (PDF) on 12 March 2020. Retrieved 12 March 2020.
- ^ Mounk Y (11 March 2020). "The Extraordinary Decisions Facing Italian Doctors". The Atlantic. Archived from the original on 12 March 2020. Retrieved 12 March 2020.
Now the Italian College of Anesthesia, Analgesia, Resuscitation and Intensive Care (SIAARTI) has published guidelines for the criteria doctors and nurses should follow in these extraordinary circumstances. The document begins by likening the moral choices facing Italian doctors to the wartime triage of 'catastrophe medicine'.
- ^ Privitera G (11 March 2020). "Italian doctors on coronavirus frontline face tough calls on whom to save". Politico. Archived from the original on 12 March 2020. Retrieved 12 March 2020.
... the Italian Society of Anesthesia, Analgesia, Resuscitation and Intensive Care, who co-authored new guidelines on how to prioritize treatment of coronavirus cases in hospitals ...
- ^ "Italy coronavirus death toll overtakes China". The Independent. 19 March 2020.
- ^ "Coronavirus: sono 33.190 i positivi – Comunicato Stampa". Dipartimento della Protezione Civile.
- ^ "'From Russia with Love': Putin sends aid to Italy to fight virus". 23 March 2020.
- ^ "Italy's coronavirus death toll passes 10,000. Many are asking why the fatality rate is so high". CNN. Retrieved 29 March 2020.
- ^ Coleman J (19 April 2020). "Italy sees fewest coronavirus deaths in a week". The Hill. Retrieved 20 April 2020.
- ^ "Conte firma il dpcm: stop a movida e gite, niente didattica a distanza". ansa.it. 13 October 2020. Retrieved 13 October 2020.
- ^ Rome, Wanted in (11 November 2020). "Covid-19: Doctors call for red zone across Italy". Wanted in Rome. Retrieved 13 November 2020.
- ^ "Italy passes 1 million Covid-19 cases, France overtakes Russia". South China Morning Post. 12 November 2020. Retrieved 13 November 2020.
- ^ Welle (www.dw.com), Deutsche. "Coronavirus: Clinics in Naples, Italy, on the brink of collapse | DW | 23 November 2020". Deutsche Welle. Retrieved 25 November 2020.
- ^ "Sanidad confirma en La Gomera el primer caso de coronavirus en España". El Pais (in Spanish). 31 January 2020. Archived from the original on 31 January 2020. Retrieved 31 January 2020.
- ^ Ansede, Manuel (22 April 2020). "El análisis genético sugiere que el coronavirus ya circulaba por España a mediados de febrero". EL PAÍS (in Spanish). Retrieved 23 April 2020.
- ^ "Estado de alarma por crisis sanitaria COVID-19—Atención e informacion—Punto de Acceso General". administracion.gob.es.
- ^ "Spain poised to tighten coronavirus lockdown after record daily toll". MSN. Retrieved 29 March 2020.
- ^ Hedgecoe, Guy (26 March 2020). "'Top of the curve'? Spain hopes Covid-19 peak reached as deaths pass 4,000". The Irish Times. Retrieved 28 March 2020.
- ^ "Coronavirus latest: Britain's Prince Charles tests positive for Covid-19". South China Morning Post. 25 March 2020. Retrieved 25 March 2020.
'Spain's coronavirus death toll overtook that of China on Wednesday, rising to 3,434 after 738 people died over the past 24 hours,' the government said.
- ^ Collman, Ashley. "Spain recorded 950 coronavirus deaths in a day, the highest single-day toll of any country". Business Insider. Retrieved 2 April 2020.
- ^ White House: CDC 'let country down' on testing – COVID-19 updates 17 May 2020 Al Jazeera. Retrieved 30 May 2020
- ^ "Por qué nadie celebra el primer día sin muertos por coronavirus en España". El Español (in Spanish). 2 June 2020. Retrieved 22 June 2020.
- ^ "Así fue el día 1 de la nueva normalidad". EL PAIS (in Spanish). 22 June 2020. Retrieved 22 June 2020.
- ^ "Coronavirus: Spain drives fears of European 'second wave'". BBC. 25 July 2020.
- ^ "Spain's Basque region admits to second wave of Covid-19". El País. 6 August 2020.
- ^ Badcock, James (14 August 2020). "Spain shuts down nightlife amid fears of major second wave of coronavirus". The Telegraph.
- ^ "Spain won't declare another national state of alarm, allows regions to lockdown if necessary". Euroactiv. 26 August 2020.
- ^ Lau H, Khosrawipour V, Kocbach P, Mikolajczyk A, Ichii H, Schubert J, et al. (March 2020). "Internationally lost COVID-19 cases". Journal of Microbiology, Immunology, and Infection = Wei Mian Yu Gan Ran Za Zhi. 53 (3): 454–458. doi:10.1016/j.jmii.2020.03.013. PMC 7102572. PMID 32205091.
- ^ Linde, Oriol Güell, Elena Sevillano, Pablo (18 March 2020). "Lack of testing hampering Spain's efforts to slow coronavirus outbreak". EL PAÍS. Retrieved 31 March 2020.
- ^ "El 5% de la población española ha superado el Covid-19". Europa Press (in Spanish). 13 May 2020. Retrieved 13 May 2020.
- ^ "Estudio de seroprevalencia: sólo el 5% de los españoles tiene anticuerpos frente al coronavirus". El Mundo (in Spanish). 13 May 2020. Retrieved 13 May 2020.
- ^ "Afloran 12.000 nuevas muertes en los registros civiles: el exceso en la crisis del coronavirus se eleva hasta los 43.000 muertos". El País (in Spanish). 3 June 2020. Retrieved 4 June 2020.
- ^ "El estudio nacional de seroprevalencia concluye que solo un 5,2% de la población española tiene anticuerposs". RTVE (in Spanish). 6 July 2020. Retrieved 15 July 2020.
- ^ Vardar, Serdar (13 May 2020). "Dos millones de españoles han estado en contacto con el nuevo coronavirus". ABC (in Spanish). Retrieved 13 May 2020.
- ^ Sam Jones; Kim Willsher; Natalie Grover (7 September 2020). "Spain is first country in western Europe to record half a million Covid cases". The Guardian.
- ^ "ARCHIVED – Spain passes the 1 million coronavirus cases mark on October 21st". murciatoday.com. Retrieved 11 December 2020.
- ^ a b Leatherby, Lauren (15 May 2020). "Sweden Stayed Open. A Deadly Month Shows the Risks". The New York Times. Retrieved 18 May 2020.
- ^ Milne, Richard (8 May 2020). "Architect of Sweden's no-lockdown strategy insists it will pay off". Financial Times. Retrieved 16 August 2020.
- ^ "Sverige diskuterar inte exitstrategier: "Vår strategi är hållbar, vi kan ligga kvar med den en väldigt lång tid"". svenska.yle.fi (in Swedish). Retrieved 16 August 2020.
- ^ Coy, Peter (14 May 2020). "The Swedish Model Trades More Disease for Less Economic Damage". Bloomberg. Retrieved 18 May 2020.
- ^ "Coronavirus: Sweden records highest weekly deaths per capita in Europe". Yahoo!. Retrieved 19 May 2020.
- ^ "Inte längre någon överdödlighet i Sverige". Dagens Medicin (in Swedish). Retrieved 16 August 2020.
- ^ "Ignore the squabbling Devolution has become less dysfunctional during the pandemic". The Economist. 6 June 2020. Retrieved 22 July 2020.
- ^ "The U.K. is aiming for deliberate 'herd immunity'". Fortune. Retrieved 14 March 2020.
- ^ "60% of UK population need to get coronavirus so country can build 'herd immunity', chief scientist says". The Independent. 13 March 2020. Retrieved 14 March 2020.
- ^ McGee L (17 March 2020). "Boris Johnson ramps up UK's coronavirus response after criticism". CNN.
- ^ "Scottish health secretary criticises virus messaging". BBC News Online. 15 March 2020.
- ^ Triggle N (16 March 2020). "What is the UK advice on coronavirus?". BBC News Online. Retrieved 17 March 2020.
- ^ Boseley S (16 March 2020). "New data, new policy: why UK's coronavirus strategy changed". The Guardian. Retrieved 17 March 2020.
- ^ Meredith S (20 March 2020). "UK PM Boris Johnson announces nationwide lockdown measures, telling cafes, pubs and restaurants to close". CNBC. Retrieved 20 March 2020.
- ^ "Coronavirus: Government to pay up to 80% of workers' wages". BBC News Online. Retrieved 20 March 2020.
- ^ "Coronavirus: Strict new curbs on life in UK announced by PM". BBC News. 24 March 2020. Retrieved 24 March 2020.
- ^ "Large-scale human trial of potential COVID-19 vaccine kicks off at Oxford". CBS News. Retrieved 24 April 2020.
- ^ Gilror R (30 March 2020). "More temporary hospitals announced ready for coronavirus peak". Nursing Times.
- ^ Davies C (3 April 2020). "Prince Charles to open NHS Nightingale to treat Covid-19 patients". The Guardian.
- ^ "Nightingale Hospital in London placed on standby". BBC News. 4 May 2020.
- ^ "Coronavirus: London's NHS Nightingale 'treated 51 patients'". BBC News. 27 April 2020.
- ^ "Coronavirus updates: Texas reports single highest daily rate increase of infections". MSN. Retrieved 17 May 2020.
- ^ Mueller, Benjamin (2 December 2020). "U.K. Approves Pfizer Coronavirus Vaccine, a First in the West". The New York Times. Retrieved 2 December 2020.
- ^ "U.K. Will Start Immunizing People Against COVID-19 On Tuesday, Officials Say". NPR. Retrieved 5 December 2020.
- ^ Clarke, Devin Scillian, Kayla (9 December 2020). "UK issues new guidance after 2 health care workers have allergic reaction to Pfizer's COVID-19 vaccine". WDIV. Retrieved 9 December 2020.
- ^ Reynolds, Emma; Braithwaite, Sharon; Cassidy, Amy. "Allergy warning for Pfizer/BioNTech vaccine after UK health workers with allergy history suffer reaction". CNN. Retrieved 9 December 2020.
- ^ "Update on Coronavirus (COVID-19) by Bonaire's Lt. Governor InfoBonaire". The Bonaire Information Site. 16 April 2020. Retrieved 17 April 2020.
- ^ "Canada Coronavirus: 834,182 Cases and 21,435 Deaths – Worldometer". worldometers.info. Retrieved 18 February 2021.
- ^ "Mexico Coronavirus: 2,013,563 Cases and 218,007 Deaths – Worldometer". worldometers.info. Retrieved 18 February 2021.
- ^ "California Coronavirus: 3,492,045 Cases and 47,916 Deaths (COVID-19 ) – Worldometer". worldometers.info. Retrieved 18 February 2021.
- ^ "Coronavirus COVID-19 (2019-nCoV)" (ArcGIS). Johns Hopkins CSSE. Frequently updated.
- ^ "Mortality Analyses". Johns Hopkins University. Retrieved 17 December 2020.
- ^ "Estimated COVID-19 Infections, Symptomatic Illnesses, and Hospitalizations—United States CDC estimates that from February 2020–March 2021". Centers for Disease Control. 14 April 2021. Retrieved 12 May 2021.
- ^ Stobbe, Mike (21 December 2020). "US deaths in 2020 top 3 million, by far most ever counted". Associated Press. Retrieved 22 December 2020.
- ^ Marchione, Marilynn (18 February 2021). "U.S. Life Expectancy Drops A Year In Pandemic, Most Since WWII". HuffPost. Retrieved 18 February 2021.
- ^ Aubrey, Allison (31 January 2020). "Trump Declares Coronavirus A Public Health Emergency And Restricts Travel From China". NPR. Retrieved 18 March 2020.
'Foreign nationals other than immediate family of U.S. citizens and permanent residents who have traveled in China in the last 14 days will be denied entry into United States,' Azar said.
- ^ Robertson, Lori (15 April 2020). "Trump's Snowballing China Travel Claim". FactCheck.org. Retrieved 29 April 2020.
... effective February 2.
- ^ Lemire, Jonathan; Miller, Zeke; Colvin, Jill; Alonso-Zaldivar, Ricardo (12 April 2020). "Signs missed and steps slowed in Trump's pandemic response". Associated Press. Retrieved 28 April 2020.
- ^ Pilkington, Ed; McCarthy, Tom (28 March 2020). "The missing six weeks: how Trump failed the biggest test of his life". The Guardian. ISSN 0261-3077. Retrieved 28 March 2020.
- ^ Ollstein, Alice Miranda (14 April 2020). "Trump halts funding to World Health Organization". Politico. ISSN 2381-1595. Wikidata Q104180080. Retrieved 28 April 2020.
- ^ Whoriskey, Peter; Satija, Neena (16 March 2020). "How U.S. coronavirus testing stalled: Flawed tests, red tape and resistance to using the millions of tests produced by the WHO". The Washington Post. Retrieved 18 March 2020.
- ^ Moon, Sarah (24 April 2020). "A seemingly healthy woman's sudden death is now the first known US coronavirus-related fatality". CNN. Retrieved 25 May 2020.
- ^ "Trump signs emergency coronavirus package, injecting $8.3 billion into efforts to fight the outbreak". Business Insider. 6 March 2020.
- ^ Liptak, Kevin (13 March 2020). "Trump declares national emergency – and denies responsibility for coronavirus testing failures". CNN. Retrieved 18 April 2020.
- ^ Biesecker, Michael (7 April 2020). "US 'wasted' months before preparing for coronavirus pandemic". Associated Press. Retrieved 24 April 2020.
- ^ Watson, Kathryn (27 March 2020). "Trump invokes Defense Production Act to require GM to produce ventilators". CBS News. Retrieved 24 April 2020.
- ^ Horwitz L, Nagovitch P, Sonnel HK, Zissis C. "Where Is the Coronavirus in Latin America?". AS/COA. Archived from the original on 22 March 2020. Retrieved 22 March 2020.
- ^ "Uncollected bodies lie for days in the streets of Ecuador the emerging epicentre of the coronavirus in Latin America". Stuff/Fairfax. 4 April 2020.
- ^ "WHO declares that South America is the new coronavirus epicenter". The Washington Post. Retrieved 23 May 2020.
- ^ Ward, Alex. "How South America became a coronavirus epicenter". Vox. Retrieved 28 May 2020.
- ^ "How Brazil went from carnival floats to mass graves. Photos show what it's like in the world's latest coronavirus hotspot". Business Insider. Retrieved 28 May 2020.
- ^ "Brazil suffers record coronavirus deaths, Trump mulls travel ban". Reuters. 20 May 2020. Retrieved 20 May 2020.
- ^ "Brazil faces dark week as Covid-19 toll rises". CNN. Retrieved 26 May 2020.
- ^ "Brazilian President Jair Bolsonaro Tests Positive For Coronavirus". NPR. Retrieved 30 July 2020.
- ^ "Global report: Bolsonaro hides Brazil's coronavirus death toll and case totals". The Guardian. 7 June 2020. Retrieved 7 June 2020.
- ^ "Coronavirus cases jump by a million in 1 week to reach 8 million worldwide". Global News. Retrieved 16 June 2020.
- ^ "Brazil Clears Sinovac Trial to Resume Two Days After Halting It". Bloomberg L.P. 11 November 2020. Retrieved 11 November 2020.
- ^ "Brazil COVID-19 cases exceed 9.5 million, death toll at 231,534". Reuters. 7 February 2021.
- ^ "Beijing orders 14-day quarantine for all returnees". BBC News. 15 February 2020. Archived from the original on 14 February 2020. Retrieved 24 March 2020.
- ^ "Egypt announces first Coronavirus infection". Egypt Today. Archived from the original on 15 February 2020. Retrieved 24 March 2020.
- ^ "Nigeria confirms first coronavirus case". BBC News. 28 February 2020. Archived from the original on 2 March 2020. Retrieved 24 March 2020.
- ^ "Remote Lesotho becomes last country in Africa to record COVID-19 case". Reuters. 13 May 2020. Archived from the original on 14 May 2020. Retrieved 13 May 2020.
- ^ "Coronavirus live updates: Lesotho becomes last African nation to report a coronavirus case". Los Angeles Times. Archived from the original on 13 May 2020. Retrieved 13 May 2020.
- ^ Akinwotu, Emmanuel (26 May 2020). "Experts sound alarm over lack of Covid-19 test kits in Africa". The Guardian. Archived from the original on 29 May 2020. Retrieved 29 May 2020.
- ^ Maclean, Ruth (17 March 2020). "Africa Braces for Coronavirus, but Slowly". The New York Times. Archived from the original on 25 March 2020. Retrieved 25 March 2020.
- ^ "Third wave sweeps across Africa as Covid vaccine imports dry up". The Guardian. 7 June 2021. Retrieved 9 June 2021.
- ^ Jason Burke; Abdalle Ahmed Mumin (2 May 2020). "Somali medics report rapid rise in deaths as Covid-19 fears grow". The Guardian. Archived from the original on 19 May 2020. Retrieved 2 May 2020.
- ^ Wiens, Kirsten E.; Mawien, Pinyi Nyimol; Rumunu, John; Slater, Damien; Jones, Forrest K.; Moheed, Serina; Caflisch, Andrea; Bior, Bior K.; Jacob, Iboyi Amanya; Lako, Richard Lino; Guyo, Argata Guracha (June 2021). "Seroprevalence of Severe Acute Respiratory Syndrome Coronavirus 2 IgG in Juba, South Sudan, 20201". Emerging Infectious Diseases. 27 (6): 1598–1606. doi:10.3201/eid2706.210568. ISSN 1080-6040. PMC 8153877. PMID 34013872.
- ^ "First confirmed case of novel coronavirus in Australia". Australian Government Department of Health. 25 January 2020. Archived from the original on 15 February 2020. Retrieved 3 March 2020.
- ^ "WHO COVID-19 Dashboard". 24 April 2020. Archived from the original on 16 April 2020. Retrieved 24 April 2020.
- ^ "Australia records 10th day of no local COVID-19 cases | Reuters".
- ^ "Covid-19 in Australia: Tasmania Defeats Virus, But Pays High Cost - Bloomberg".
- ^ Cave, Damien (1 February 2021). "One Case, Total Lockdown: Australia's Lessons for a Pandemic World". The New York Times. Archived from the original on 31 March 2021. Retrieved 15 April 2021.
- ^ "Cook Islands detects first positive Covid-19 case". Cook Islands News. 6 June 2021. Retrieved 7 June 2021.
- ^ Taylor, Adam; Pitrelli, Stefano (24 March 2020). "One continent remains untouched by the coronavirus: Antarctica". The Washington Post. Archived from the original on 1 April 2020. Retrieved 3 April 2020.
- ^ Torres, Elle (20 March 2020). "What life is like on Antarctica, the only continent without a case of coronavirus". ABC News. Archived from the original on 1 April 2020. Retrieved 3 April 2020.
- ^ Agence France-Presse (31 March 2020). "Pacific islands, Antarctic bases: coronavirus-free living in some of Earth's most isolated places". South China Morning Post. Archived from the original on 3 April 2020. Retrieved 3 April 2020.
- ^ "Reportan brote de coronavirus en base chilena en la Antártida". infobae (in Spanish). 21 December 2020. Archived from the original on 23 December 2020. Retrieved 21 December 2020.
- ^ IMF. "The IMF's Response to COVID-19".
- ^ Barnes, Julian E. (8 April 2021). "U.S. Intelligence Report Warns of Global Consequences of Social Fragmentation". The New York Times. Retrieved 8 May 2021.
- ^ "Coronavirus Travel Restrictions, Across the Globe". The New York Times. 26 March 2020.
- ^ "Coronavirus (COVID-19) – information for Australian travellers". Australian Government. 9 April 2020.
- ^ Nsikan, Akpan (24 February 2020). "Coronavirus spikes outside China show travel bans aren't working". National Geographic. Retrieved 2 April 2020.
- ^ Chinazzi M, Davis JT, Ajelli M, Gioannini C, Litvinova M, Merler S, et al. (April 2020). "The effect of travel restrictions on the spread of the 2019 novel coronavirus (COVID-19) outbreak". Science. 368 (6489): 395–400. Bibcode:2020Sci...368..395C. doi:10.1126/science.aba9757. PMC 7164386. PMID 32144116.
- ^ "COVID-19: Study shows that travel restrictions are most useful in the early and late phase of an epidemic". Oxford Martin School, University of Oxford. 25 March 2020.
- ^ "Coronavirus: EU rules out Schengen border closures amid Italy outbreak". Deutsche Welle. 24 February 2020.
- ^ "Commission chief warns against unilateral virus travel bans". EURACTIV. 13 March 2020.
- ^ "Coronavirus in India: Latest Map and Case Count". covid19india.org. Retrieved 11 June 2020.
- ^ "Countries Evaluate Evacuation of Citizens Amid Wuhan Coronavirus Panic". Associated Press. Retrieved 31 January 2020 – via The Diplomat.
- Press, ANI. "Coronavirus: Second plane carrying 323 Indians from Wuhan to reach Delhi today". India Today. Retrieved 2 February 2020.
- NWS, VRT (27 January 2020). "België haalt landgenoten terug uit Chinese provincie Hubei na uitbraak coronavirus". VRT Nws. Vlaamse Radio- en Televisieomroeporganisatie.
- Nathalia T (30 January 2020). "Last-Minute Preparations Underway to Evacuate Indonesian Citizens From Coronavirus-Ravaged Wuhan". Jakarta Globe.
- "C130 aircraft on standby for Wuhan evacuation". Bangkok Post. 26 January 2020. Retrieved 26 January 2020.
- Jiang S, Stracqualursi V (25 January 2020). "US arranging charter flight to evacuate American diplomats and citizens out of China amid coronavirus outbreak, official says". CNN. Archived from the original on 26 January 2020. Retrieved 27 January 2020.
- "PH sending special flights to get Pinoys from Wuhan, Hubei in China". Tempo: News in a Flash. Manila, Philippines. 29 January 2020. Retrieved 29 January 2020.
- ^ "Aviões decolam de Wuhan, na China, com 40 passageiros repatriados ao Brasil e à Polônia". G1 (in Portuguese). 7 February 2020. Retrieved 9 February 2020.
- ^ "Air New Zealand flight with kiwi evacuees departs Wuhan". Stuff (company). 5 February 2020.
- ^ "Repatriated citizens to be reunited with families". SANews.gov.zanews24.com. 29 March 2020. Retrieved 31 March 2020.
- ^ "Pakistan cancels flights to China as fears of coronavirus spread". Dialogue Pakistan. 31 January 2020. Retrieved 5 April 2020.
- ^ Wang V, Rich M, Bradsher K (15 February 2020). "Shifting Ground in Coronavirus Fight: U.S. Will Evacuate Americans From Cruise Ship". The New York Times. Retrieved 15 February 2020.
- ^ "Cruise ship passengers begin 14-day quarantine in Cornwall, Ont". CBC News. 21 February 2020.
- ^ Roche E (9 March 2020). "Coronavirus: India sending IAF aircraft to evacuate its nationals from Iran". LiveMint.com. Retrieved 9 March 2020.
- ^ "4th batch of 53 Indians evacuated from Iran: S Jaishankar". The Economic Times. 16 March 2020. Retrieved 28 March 2020.
- ^ Kheel, Rebecca (20 March 2020). "US-led coalition in Iraq drawing down over coronavirus concerns". The Hill. Retrieved 7 April 2020.
- ^ "UN tallies action so far to fight COVID-19, and roadmap out of the pandemic". UN News. 25 June 2020. Retrieved 4 August 2020.
- ^ "Global Ceasefire Call Deserves UN Security Council's Full Support". Crisis Group. 9 April 2020. Retrieved 1 August 2020.
- ^ Dempsey, Harry; Wilson, Tom (18 January 2021). "WHO warns of global 'moral failure' on vaccines". Financial Times. Retrieved 18 January 2021.
- ^ Borger, Julian (18 April 2020). "Caught in a superpower struggle: the inside story of the WHO's response to coronavirus". The Guardian. Retrieved 19 April 2020.
- ^ "German anti-lockdown protests led to more coronavirus cases, study finds". Politico. 9 February 2021. Retrieved 17 February 2021.
- ^ Miller JY (7 February 2020). "WashU Expert: Coronavirus far greater threat than SARS to global supply chain". The Source. Retrieved 13 February 2020.
- ^ McLean R, He L, Tappe A (24 February 2020). "Dow plunges 1,000 points as coronavirus cases surge in South Korea and Italy". CNN.
- ^ "FTSE 100 plunges 3.7 per cent as Italy confirms sixth coronavirus death". City A.M. London. 24 February 2020.
- ^ Tappe A. "Dow falls 1,191 points – the most in history". CNN. Retrieved 28 February 2020.
- ^ Oh S (28 February 2020). "Stocks record worst week since financial crisis as coronavirus concerns heat up". Market Watch. Retrieved 28 February 2020.
- ^ "Scope affirms China's sovereign rating at A+ and maintains the Outlook at Negative". Scope Ratings GmbH. 28 February 2020. Retrieved 11 March 2020.
- ^ "Stocks Plummet as Grim Economic Outlook Grips Markets: Live Updates". The New York Times. 16 March 2020. Retrieved 16 March 2020.
- ^ Keown, Callum (14 May 2020). "Global insurers face losses of $204 billion from Coronavirus, more than 9/11 and 2017 hurricanes, says Lloyd's of London". MarketWatch. Retrieved 28 May 2020.
- ^ "Collapsed Flybe: 'Do not travel to the airport'". BBC News. 5 March 2020.
- ^ Turner B (4 April 2020). "'Most significant crisis in the history of travel': where to now for tourism?". The Sydney Morning Herald. Retrieved 5 April 2020.
- ^ "Coronavirus scare: Complete list of airlines suspending flights". India Today. Reuters. 27 February 2020. Retrieved 7 March 2020.
- ^ Cherney, Mike; Craymer, Lucy (5 May 2020). "You've Got Mail ... Finally: The Pandemic Is Jamming Up the World's Post". The Wall Street Journal. Retrieved 15 May 2020.
- ^ National Retail Federation (21 March 2020), Coronavirus Resources for Retailers, retrieved 23 March 2020
- ^ Aislelabs Inc (2 April 2020), How Retailers Globally are Responding to Coronavirus by Aislelabs, retrieved 3 April 2020
- ^ Aislelabs (23 March 2020), How Shopping Centres Globally are Responding to Coronavirus by Aislelabs, retrieved 23 March 2020
- ^ "Half the world's workers face losing their jobs, says ILO". Al Jazeera. 29 April 2020.
- ^ "No jobs, so what future? Half the world's workforce on the edge". The Monitor. 6 May 2020.
- ^ Romm, Tony (28 May 2020). "Americans have filed more than 40 million jobless claims in past 10 weeks, as another 2.1 million filed for benefits last week". The Washington Post.
- ^ "43 million Americans at risk of eviction as relief programs and moratorium expire: "It's a nightmare"". CBS News. 31 July 2020.
- ^ "32% of Americans had outstanding housing payments at the beginning of August". CNBC. 6 August 2020.
- ^ "Millions of Americans at risk of eviction after moratorium expired". Fox News. 12 August 2020.
- ^ "As Stimulus Talks Stalemate, New Report Finds 40 Million Americans Could Be At Risk Of Eviction". Forbes. 7 August 2020.
- ^ "Yelp data shows 60% of business closures due to the coronavirus pandemic are now permanent". CNBC. 16 September 2020.
- ^ Fariza I (3 April 2020). "La pandemia amenaza con dejar entre 14 y 22 millones de personas más en pobreza extrema en Latinoamérica". El País (in Spanish). Retrieved 3 April 2020.
- ^ "Updated estimates of the impact of COVID-19 on global poverty". World Bank. 8 June 2020.
- ^ "Extreme poverty rises and a generation sees future slip away". AP News. 10 August 2020.
- ^ Nebehay, Stephanie (23 September 2020). "Pandemic slashes worldwide income from work by a tenth: ILO". Reuters. Retrieved 23 September 2020.
- ^ Tyko K (29 February 2020). "Coronavirus fears empty store shelves of toilet paper, bottled water, masks as shoppers stock up". USA Today.
- ^ Yuen, Kum Fai; Wang, Xueqin; Ma, Fei; Li, Kevin X. (2020). "The psychological causes of panic buying following a health crisis". International Journal of Environmental Research and Public Health. 17 (10): 3513. doi:10.3390/ijerph17103513. PMC 7277661. PMID 32443427. S2CID 218856048.
- ^ Strumpf D (31 January 2020). "Tech Sector Fears Supply Delays as Effects of Virus Ripple Through China". The Wall Street Journal. Retrieved 26 February 2020.
- ^ Nebehay S (7 February 2020). "Procura por máscaras aumenta 100 vezes e prejudica luta contra o coronavírus" (in Portuguese). Reuters Brasil. Retrieved 20 May 2021.
- ^ Boseley S (7 February 2020). "WHO warns of global shortage of face masks and protective suits". The Guardian. Retrieved 12 February 2020.
- ^ "Shortage of personal protective equipment endangering health workers worldwide". World Health Organization (WHO). Retrieved 5 March 2020.
- ^ "Corona snijdt ook in het vlees van de drugsmaffia". DS Standaard. 11 April 2020. Retrieved 20 April 2020.
- ^ Grierson, Jamie (12 April 2020). "Coronavirus triggers UK shortage of illicit drugs". The Guardian. Retrieved 20 April 2020.
- ^ Torero, Maximo (14 April 2020). "How to Stop a Looming Food Crisis". Foreign Policy.
- ^ "Global hunger could double due to coronavirus pandemic: UN". Al Jazeera. 21 April 2020.
- ^ a b "Coronavirus: World risks 'biblical' famines due to pandemic – UN". BBC News. 21 April 2020.
- ^ "Senior Officials Sound Alarm over Food Insecurity, Warning of Potentially 'Biblical' Famine, in Briefings to Security Council". United Nations. 21 April 2020.
- ^ "'Instead of Coronavirus, the Hunger Will Kill Us.' A Global Food Crisis Looms". The New York Times. 22 April 2020.
- ^ Reed S (3 February 2020). "OPEC Scrambles to React to Falling Oil Demand From China". The New York Times. Retrieved 14 February 2020.
- ^ a b US oil prices turn negative as demand dries up, BBC, 21 April 2020.
- ^ "Here are the museums that have closed (so far) due to coronavirus". theartnewspaper.com. Retrieved 29 March 2020.
- ^ "The Ultimate Guide to Virtual Museum Resources". MCN. 15 March 2020. Retrieved 29 March 2020.
- ^ a b c d e Burke D (14 March 2020). "What churches, mosques and temples are doing to fight the spread of coronavirus". CNN. Retrieved 16 March 2020.
- ^ Hadden J (2 March 2020). "Over 20,000 people have signed a petition to cancel SXSW over coronavirus worries. Here's a list of all the major event cancellations due to the outbreak so far". Business Insider. Retrieved 3 March 2020.
- ^ Fadroski KS (15 March 2020). "Coronavirus canceled their concerts, so artists like Yungblud are looking to live stream shows to fans". Daily Breeze.
- ^ Brenner, Wayne Alan (15 March 2020). "The Social Distancing Festival Is Live Online". The Austin Chronicle.
- ^ Parke, Caleb (13 March 2020). "Churches cancel Sunday service, move online amid coronavirus outbreak". Fox News. Retrieved 16 March 2020.
- ^ "Westerville church offering 'drive in' service". WBNS-TV. 22 March 2020. Archived from the original on 22 March 2020. Retrieved 22 March 2020.
- ^ Al Omran A, Kerr S (27 February 2020). "Saudi Arabia bans Mecca pilgrimages over coronavirus fears". Financial Times.
- ^ "Coronavirus: Saudi Arabia bans all Umrah pilgrimage to Mecca". Middle East Eyes. 4 March 2020.
- ^ "'Unprecedented' Hajj begins – with 1,000 pilgrims, rather than the usual 2 million". CNN. 29 July 2020.
- ^ "All of next week's UEFA matches postponed". UEFA. 13 March 2020.
- ^ Edwards, Harry (13 March 2020). "Premier League 2019/20 season suspended after coronavirus cases at Chelsea, Arsenal and more". squawka.com.
- ^ Close D, Jackson A. "NBA suspends its season after player tests positive for coronavirus". CNN. Archived from the original on 12 March 2020. Retrieved 12 March 2020.
- ^ "NHL statement on coronavirus". National Hockey League. 12 March 2020. Archived from the original on 14 March 2020. Retrieved 13 March 2020.
- ^ Silva, Steve; d'Entremont, Danielle (7 March 2020). "'Shocked and disappointed': Arctic Winter Games cancelled due to coronavirus concerns". CBC News.
- ^ "Tokyo 2020: Olympic Games organisers 'agree postponement'". BBC Sport. 24 March 2020. Retrieved 24 March 2020.
- ^ McCurry, Justin; Ingle, Sean (24 March 2020). "Tokyo Olympics postponed to 2021 due to coronavirus pandemic". The Guardian. Retrieved 24 March 2020.
- ^ "IOC, IPC, Tokyo 2020 Organising Committee and Tokyo Metropolitan Government Announce New Dates for the Olympic and Paralympic Games Tokyo 2020". International Olympic Committee. 30 March 2020. Archived from the original on 30 March 2020. Retrieved 30 March 2020.
- ^ "How the coronavirus outbreak is roiling the film and entertainment industries". Vox. 13 March 2020.
- ^ "Coronavirus brings entertainment world to a standstill". Associated Press. 13 March 2020.
- ^ Savage, Mark (18 March 2020). "Eurovision Song Contest cancelled over coronavirus". BBC News. Retrieved 25 May 2020.
- ^ "Rotterdam returns as Eurovision Song Contest Host City in 2021". European Broadcasting Union. 16 May 2020. Retrieved 15 June 2020.
- ^ "Broadway theaters to suspend all performances because of coronavirus". CNN. 12 March 2020. Archived from the original on 13 March 2020. Retrieved 13 March 2020.
- ^ "How to Combat Zoom Fatigue". Harvard Business Review. 29 April 2020 – via hbr.org.
- ^ "Walmart Reports Increased Sales In Tops, Not Bottoms, As More People Telework". NPR.
- ^ Harris M. "Coronavirus memes are spreading as the disease travels across the world – here's what they look like and why creators say they're important". Insider. Retrieved 8 April 2020.
- ^ Tumilty, Ryan (13 March 2020). "Federal government announces aggressive measures to battle COVID-19 as parliament suspended until April". National Post. Retrieved 30 April 2020.
- ^ Mackinnon A, Palder D (18 March 2020). "Coronavirus in the Corridors of Power". Foreign Policy. Retrieved 30 April 2020.
- ^ Corasaniti N, Saul S (27 April 2020). "15 States Have Postponed Primaries During the Pandemic. One Has Canceled". The New York Times. ISSN 0362-4331. Retrieved 30 April 2020.
- ^ The Economist, 4 April 2020, page 14.
- ^ "Transcript of the Secretary-General's virtual press encounter on the appeal for global ceasefire". United Nations Secretary-General. 23 March 2020. Retrieved 1 August 2020.
- ^ "COVID-19: UN chief calls for global ceasefire to focus on 'the true fight of our lives'". UN News. 23 March 2020. Retrieved 1 August 2020.
- ^ "170 signatories endorse UN ceasefire appeal during COVID crisis". UN News. 24 June 2020. Retrieved 1 August 2020.
- ^ "S/RES/2532(2020) – E – S/RES/2532(2020)". undocs.org. Retrieved 1 August 2020.
- ^ "Stalled Security Council resolution adopted, backing UN's global humanitarian ceasefire call". UN News. 1 July 2020. Retrieved 1 August 2020.
- ^ "U.S. and China Turn Coronavirus into a Geopolitical Football". Foreign policy. 11 March 2020.
- ^ "Michael Gove appears to blame China over lack of UK coronavirus testing". The Guardian. 29 March 2020.
- ^ "China Outraged as Bolsonaro's Son Blames Virus on Beijing". Bloomberg. 19 March 2020.
- ^ Bostock B (13 February 2020). "China sacked a brace of top officials in Hubei province, likely in a move to protect Xi Jinping from people's anger over the coronavirus outbreak". Business Insider. Retrieved 26 February 2020.
- ^ "C.I.A. Hunts for Authentic Virus Totals in China, Dismissing Government Tallies". The New York Times. 2 April 2020.
- ^ "China Denies Cover-Up, Rejects 'Politicization' of Coronavirus". Bloomberg. Retrieved 7 June 2020.
- ^ "China CDC informs U.S. of COVID-19 on Jan. 4: white paper". Xinhua News Agency. Retrieved 7 June 2020.
- ^ "Chen Qiushi: Chinese journalist missing since February 'under state supervision'". BBC News. 24 September 2020. Retrieved 16 February 2021.
- ^ "Li Zehua: Journalist who 'disappeared' after Wuhan chase reappears". BBC News. 23 April 2020. Retrieved 16 February 2021.
- ^ "Covid-19 journalist tortured for exposing truth". amnesty.org.uk. Retrieved 16 February 2021.
- ^ "Zhang Zhan: China jails citizen journalist for Wuhan reports". BBC News. 28 December 2020. Retrieved 16 February 2021.
- ^ "Citizen journalist detained over Wuhan reporting 'restrained and fed by tube'". The Guardian. 10 December 2020. Retrieved 16 February 2021.
- ^ "Italy criticises EU for being slow to help over coronavirus epidemic". The Guardian. 11 March 2020.
- ^ "The EU Is Abandoning Italy in Its Hour of Need". Foreign Policy. 14 March 2020.
- ^ "China is winning the coronavirus propaganda war". Politico. 18 March 2020.
- ^ "Russian army to send coronavirus help to Italy after Putin phone call". Reuters. 22 March 2020.
- ^ Vivaldelli R (28 March 2020). "Quelle polemiche infondate sugli aiuti russi all'Italia". Il Giornale.
- ^ "Where Has Russia Sent Coronavirus Aid Around the World?". The Moscow Times. 1 April 2020.
- ^ "Russian plane takes off for US with coronavirus help on board". Al Jazeera. 1 April 2020.
- ^ "Coronavirus: EU Medical Teams deployed to Italy". Europa (web portal). 1 July 2020.
- ^ "EU offers 'heartfelt apology' to Italy over coronavirus response". The Guardian. 1 July 2020.
- ^ Rouan, Rick (20 April 2020). "Protesters at Statehouse demand state reopen as DeWine announces schools to remain closed". The Columbus Dispatch. Retrieved 3 May 2020.
- ^ Miller, Claire Cain (10 April 2020). "Could the Pandemic Wind Up Fixing What's Broken About Work in America?". The New York Times. Retrieved 3 May 2020.
- ^ Swanson, Ian (2 May 2020). "Five ways the coronavirus could change American politics". The Hill. Retrieved 3 May 2020.
- ^ "America's botched response to the coronavirus is a problem bigger than Donald Trump". The Boston Globe.
- ^ Haberman M, Martin J (12 March 2020). "Trump's Re-election Chances Suddenly Look Shakier". The New York Times. ISSN 0362-4331. Retrieved 15 March 2020.
- ^ Lowrey, Annie (3 April 2020). "The Economy Is Collapsing. So Are Trump's Reelection Chances". The Atlantic. Retrieved 3 May 2020.
- ^ "Coronavirus: Anti-Lockdown Protests Grow Across US". BBC News. 17 April 2020. Archived from the original on 17 April 2020. Retrieved 17 April 2020.
- ^ Russ, Hilary (30 March 2020). "Instacart, Amazon workers strike as labor unrest grows during coronavirus crisis". Reuters. Retrieved 24 July 2020.
- ^ Baker, Peter; Haberman, Maggie (3 October 2020). "Trump Tests Positive for the Coronavirus". The New York Times. ISSN 0362-4331. Retrieved 3 October 2020.
- ^ "How coronavirus derailed the largest Nato exercise in 25 years". The Spectator. 20 March 2020.
- ^ Emmott, Robin (19 March 2020). "NATO scales down exercises due to coronavirus". Reuters. Retrieved 21 October 2020.
- ^ "Nato must end 'dangerous and irresponsible' military exercise on Russia's border, campaigners say". Morning Star. 18 March 2020.
- ^ "Will Iran's Regime Survive Coronavirus?". National Review. 12 March 2020. Retrieved 15 March 2020.
- ^ "U.S. sanctions 'severely hamper' Iran coronavirus fight, Rouhani says". Reuters. 14 March 2020.
- ^ Haverty, Dan; Gramer, Robbie; Detsch, Jack (9 April 2020). "Coronavirus Pandemic Forces a Cease-Fire in Yemen". Foreign Policy. Retrieved 21 October 2020.
- ^ "Japan and Korea Won't Let A Pandemic Stop Them Fighting". Foreign Policy. 12 March 2020.
- ^ Farrer, Justin; McCurry, Martin (6 March 2020). "Coronavirus quarantine plans ignite row between South Korea and Japan". The Guardian. Retrieved 21 October 2020.
- ^ "Authoritarian leaders may use Covid-19 crisis to tighten their grip". The Guardian. 31 March 2020.
- ^ "For Autocrats, and Others, Coronavirus Is a Chance to Grab Even More Power". The New York Times. 30 March 2020.
- ^ a b "Some leaders use pandemic to sharpen tools against critics". ABC News. 16 April 2020.
- ^ "Hungarian parliament votes to let Viktor Orban rule by decree in wake of coronavirus pandemic". CNN. 30 March 2020.
- ^ "Reporting on the coronavirus: Egypt muzzles critical journalists". Deutsche Welle. 3 April 2020.
- ^ "Coronavirus Has Started a Censorship Pandemic". The Foreign Policy. 1 April 2020.
- ^ "Asia cracks down on coronavirus 'fake news'". The Straits Times. 10 April 2020.
- ^ "As COVID-19 spreads, India tries to control the narrative by targeting journalists". Los Angeles Times. 4 October 2020. Retrieved 16 February 2021.
- ^ "Record number of journalists imprisoned in 2020 – report". Reuters. 15 December 2020. Retrieved 16 February 2021.
- ^ "Press freedom: Journalists end up in jail for reporting on coronavirus crisis". Deutsche Welle. 14 December 2020. Retrieved 16 February 2021.
- ^ a b "Q&A: COVID-19 pandemic – impact on food and agriculture". Food and Agriculture Organization of the United Nations. Retrieved 16 October 2020.
- ^ a b c The State of Food Security and Nutrition in the World 2020 | FAO | Food and Agriculture Organization of the United Nations. www.fao.org. 2020. doi:10.4060/CA9692EN. ISBN 978-92-5-132901-6. Retrieved 16 October 2020.
- ^ Daventry, Michael (14 July 2020). "World hunger rising and COVID-19 threatens to make it worse, says UN". euronews. Retrieved 16 October 2020.
- ^ "Coronavirus crisis could double number of people suffering acute hunger – UN". The Guardian. 21 April 2020. Retrieved 16 October 2020.
- ^ "2020 Global report on food crises: Joint analysis for better decisions". ifpri.org. Food Security Information Network (FSIN). Retrieved 16 October 2020.
- ^ a b Harvey, Fiona (21 April 2020). "Coronavirus pandemic 'will cause famine of biblical proportions'". The Guardian. ISSN 0261-3077. Retrieved 19 June 2020.
- ^ "UN food agency chief: World on brink of 'a hunger pandemic'". ABC News. Retrieved 19 June 2020.
- ^ a b "12,000 people per day could die from Covid-19 linked hunger by end of year, potentially more than the disease, warns Oxfam". Oxfam International. 9 July 2020. Retrieved 9 July 2020.
- ^ Harvey, Fiona (21 April 2020). "Coronavirus crisis could double number of people suffering acute hunger – UN". The Guardian. ISSN 0261-3077. Retrieved 19 June 2020.
- ^ "COVID 19 Today and China's Great Famine". The Globalist. 16 May 2020. Retrieved 19 June 2020.
- ^ "2020 Global Report On Food Crises". WFP. 22 April 2020.
- ^ "Education: From disruption to recovery". UNESCO. 4 March 2020. Retrieved 12 October 2020.
- ^ "Covid: Many students say their mental health is worse due to pandemic". BBC News. 31 March 2021. Retrieved 6 April 2021.
- ^ Garcia S, Albaghdadi MS, Meraj PM, Schmidt C, Garberich R, Jaffer FA, et al. (June 2020). "Reduction in ST-Segment Elevation Cardiac Catheterization Laboratory Activations in the United States During COVID-19 Pandemic". Journal of the American College of Cardiology. 75 (22): 2871–2872. doi:10.1016/j.jacc.2020.04.011. PMC 7151384. PMID 32283124.
- ^ a b 'Where are all our patients?': Covid phobia is keeping people with serious heart symptoms away from ERs, Stat News, Usha Lee McFarling, 23 April 2020.
- ^ Faust JS (28 April 2020). "Medication Shortages Are the Next Crisis". The Atlantic. Retrieved 17 May 2020.
- ^ "Sexually transmitted infections surveillance reports - Reports". www.health.nsw.gov.au. Retrieved 9 May 2020.
- ^ Wareham J. "U.K. Lockdown Has 'Broken HIV Chain' With Huge Reduction In New STI Cases". Forbes. Retrieved 9 May 2020.
- ^ Cowling BJ, Ali ST, Ng TW, Tsang TK, Li JC, Fong MW, et al. (May 2020). "Impact assessment of non-pharmaceutical interventions against coronavirus disease 2019 and influenza in Hong Kong: an observational study". The Lancet. Public Health. 5 (5): e279–e288. doi:10.1016/S2468-2667(20)30090-6. PMC 7164922. PMID 32311320.
- ^ Klein A. "Australia sees huge decrease in flu cases due to coronavirus measures". New Scientist. Retrieved 9 May 2020.
- ^ "Weekly U.S. Influenza Surveillance Report (FluView)". U.S. Centers for Disease Control and Prevention (CDC). 8 May 2020. Retrieved 9 May 2020.
- ^ Brooks SK, Webster RK, Smith LE, Woodland L, Wessely S, Greenberg N, Rubin GJ (March 2020). "The psychological impact of quarantine and how to reduce it: rapid review of the evidence". Lancet. 395 (10227): 912–920. doi:10.1016/S0140-6736(20)30460-8. PMC 7158942. PMID 32112714.
- ^ Surkova E, Nikolayevskyy V, Drobniewski F (September 2020). "False-positive COVID-19 results: hidden problems and costs". The Lancet. Respiratory Medicine. 8 (12): 1167–1168. doi:10.1016/S2213-2600(20)30453-7. PMC 7524437. PMID 33007240.
- ^ Czeisler MÉ, Lane RI, Petrosky E, Wiley JF, Christensen A, Njai R, et al. (August 2020). "Mental Health, Substance Use, and Suicidal Ideation During the COVID-19 Pandemic - United States, June 24-30, 2020". MMWR. Morbidity and Mortality Weekly Report. 69 (32): 1049–1057. doi:10.15585/mmwr.mm6932a1. PMC 7440121. PMID 32790653.
- ^ Castellanos-Torres, Esther; Mateos, José Tomás; Chilet-Rosell, Elisa (3 March 2021). "COVID-19 en clave de género". Gaceta Sanitaria (in Spanish). 34 (5): 419–421. doi:10.1016/j.gaceta.2020.04.007. ISSN 0213-9111. PMC 7190475. PMID 32423661.
- ^ "Earth Observatory". Archived from the original on 2 April 2020. Retrieved 9 April 2020.
- ^ Bauwens, M.; Compernolle, S.; Stavrakou, T.; Müller, J.‐F.; Gent, J.; Eskes, H.; Levelt, P. F.; A, R.; Veefkind, J. P.; Vlietinck, J.; Yu, H. (5 June 2020). "Impact of Coronavirus Outbreak on NO 2 Pollution Assessed Using TROPOMI and OMI Observations". Geophysical Research Letters. 47 (11). doi:10.1029/2020gl087978. ISSN 0094-8276.
- ^ Rutz, Christian; Loretto, Matthias-Claudio; Bates, Amanda E.; Davidson, Sarah C.; Duarte, Carlos M.; Jetz, Walter; Johnson, Mark; Kato, Akiko; Kays, Roland; Mueller, Thomas; Primack, Richard B. (September 2020). "COVID-19 lockdown allows researchers to quantify the effects of human activity on wildlife". Nature Ecology & Evolution. 4 (9): 1156–1159. doi:10.1038/s41559-020-1237-z. ISSN 2397-334X. PMID 32572222.
- ^ Team, The Visual and Data Journalism (28 March 2020). "Coronavirus: A visual guide to the pandemic". BBC News. Archived from the original on 27 March 2020.
- ^ Venter, Zander S.; Aunan, Kristin; Chowdhury, Sourangsu; Lelieveld, Jos (11 August 2020). "COVID-19 lockdowns cause global air pollution declines". Proceedings of the National Academy of Sciences. 117 (32): 18984–18990. Bibcode:2020PNAS..11718984V. doi:10.1073/pnas.2006853117. ISSN 0027-8424. PMC 7430997. PMID 32723816. S2CID 220850924.
- ^ Zhang, Ruixiong; Zhang, Yuzhong; Lin, Haipeng; Feng, Xu; Fu, Tzung-May; Wang, Yuhang (April 2020). "NOx Emission Reduction and Recovery during COVID-19 in East China". Atmosphere. 11 (4): 433. Bibcode:2020Atmos..11..433Z. doi:10.3390/atmos11040433. S2CID 219002558. Retrieved 6 May 2020.
- ^ Myllyvirta, Lauri (19 February 2020). "Analysis: Coronavirus has temporarily reduced China's CO2 emissions by a quarter". CarbonBrief. Archived from the original on 4 March 2020. Retrieved 16 March 2020.
- ^ Burke, Marshall. "COVID-19 reduces economic activity, which reduces pollution, which saves lives". Global Food, Environment and Economic Dynamics. Retrieved 16 May 2020.
- ^ McMahon, Jeff (16 March 2020). "Study: Coronavirus Lockdown Likely Saved 77,000 Lives In China Just By Reducing Pollution". Forbes. Archived from the original on 17 March 2020. Retrieved 16 March 2020.
- ^ Simon, Frédéric (27 May 2020). "'Do no harm': EU recovery fund has green strings attached". www.euractiv.com. Retrieved 4 June 2020.
- ^ Carpenter, Scott. "As Europe Unveils 'Green' Recovery Package, Trans-Atlantic Rift On Climate Policy Widens". Forbes. Retrieved 4 June 2020.
- ^ "France and Germany Bring European Recovery Fund Proposal to Table". South EU Summit. 4 June 2020. Retrieved 4 June 2020.
- ^ "Conservationists fear African animal poaching will increase during COVID-19 pandemic". ABC News. 14 April 2020.
- ^ "'Filthy bloody business:' Poachers kill more animals as coronavirus crushes tourism to Africa". CNBC. 24 April 2020.
- ^ "Cop26 climate talks postponed to 2021 amid coronavirus pandemic". Climate Home News. 1 April 2020. Archived from the original on 4 April 2020. Retrieved 2 April 2020.
- ^ "Deforestation of Amazon rainforest accelerates amid COVID-19 pandemic". ABC News. 6 May 2020.
- ^ "Deforestation of the Amazon has soared under cover of the coronavirus". NBC News. 11 May 2020.
- ^ Newburger, Emma (13 March 2020). "Coronavirus could weaken climate change action and hit clean energy investment, researchers warn". CNBC. Archived from the original on 15 March 2020. Retrieved 16 March 2020.
- ^ Burton N (7 February 2020). "The coronavirus exposes the history of racism and "cleanliness"". Vox. Archived from the original on 7 February 2020. Retrieved 9 February 2020.
- ^ "Fears of new virus trigger anti-China sentiment worldwide". The Korea Times. 2 February 2020.
- ^ "Coronavirus fuels anti-Chinese discrimination in Africa". Deutsche Welle. 19 February 2020.
- ^ Miao, Hannah (12 February 2021). "VP Harris responds to surge in violent attacks against Asian Americans". CNBC. Retrieved 14 February 2021.
- ^ "COVID-19: NHS staff fall victim to anti-Chinese hate crimes – amid fears violence will rise when lockdown ends". Sky News. Retrieved 14 February 2021.
- ^ Wangkiat, Paritta (10 February 2020). "Virus-induced racism does no one any good". Bangkok Post.
- ^ Bartholomew, Robert (6 February 2020). "The Coronavirus and the Search for Scapegoats". Psychology Today.
- ^ Smith N (1 February 2020). "Anti-Chinese racism spikes as virus spreads globally". The Daily Telegraph.
'Some Muslims were claiming the disease was "divine retribution" for China's oppression of the Uighur minority. The problem lay in confusing the Chinese population with the actions of an authoritarian government known for its lack of transparency,' he said.
- ^ Tavernise S, Oppel Jr RA (23 March 2020). "Spit On, Yelled At, Attacked: Chinese-Americans Fear for Their Safety". The New York Times. Retrieved 23 March 2020.
- ^ "London Racially Motivated Assault due to Coronavirus". ITV News. 4 March 2020. Retrieved 4 March 2020.
- ^ La Gorce, Tammy (5 April 2020). "Chinese-Americans, Facing Abuse, Unite to Aid Hospitals in Coronavirus Battle". The New York Times. Retrieved 29 April 2020.
- ^ Rogers K, Jakes L, Swanson A (18 March 2020). "Trump Defends Using 'Chinese Virus' Label, Ignoring Growing Criticism". The New York Times. Archived from the original on 20 March 2020. Retrieved 20 March 2020.
- ^ "Republicans are using racism against China to try to distract from Trump's disastrous coronavirus response". Business Insider. 20 March 2020.
- ^ Lee, Bruce Y. "Trump Once Again Calls Covid-19 Coronavirus The 'Kung Flu'". Forbes. Retrieved 9 July 2020.
- ^ Wray, Meaghan. "Stabbing attack on Asian family deemed coronavirus hate crime, FBI says". Global News. Retrieved 7 September 2020.
- ^ "Italy Shows Just How Crazy Coronavirus Panic Can Get". The Daily Beast. 29 February 2020.
- ^ "Italians Are Being Treated as a Risk Abroad Over Coronavirus". The Wall Street Journal. 28 February 2020.
- ^ Kolachalam N (9 April 2020). "Indian Muslims Are Being Scapegoated for the Coronavirus". Slate. Retrieved 10 April 2020.
- ^ "Violence flares in tense Paris suburbs as heavy-handed lockdown stirs 'explosive cocktail'". France 24. 21 April 2020.
- ^ "Covid-19 Fueling Anti-Asian Racism and Xenophobia Worldwide". Human Rights Watch. 12 May 2020.
- ^ "Gulf coronavirus racism scandals shine light on conditions for migrants". TRT World. 17 April 2020. Retrieved 17 May 2020.
- ^ "The COVID-19 crisis is fueling more racist discourse towards migrant workers in the Gulf". Migrant Rights. 5 April 2020.
- ^ Thoreson, Ryan (13 May 2020). "Covid-19 Backlash Targets LGBT People in South Korea". Human Rights Watch.
- ^ Banka, Neha (21 May 2020). "Explained: Why South Korea's new Covid-19 outbreak has the LGBTQ community worried". The Indian Express.
- ^ Asiedu KG. "After enduring months of lockdown, Africans in China are being targeted and evicted from apartments". Quartz Africa. Retrieved 13 April 2020.
- ^ Marsh J. "Beijing faces a diplomatic crisis after reports of mistreatment of Africans in China causes outrage". CNN. Retrieved 14 April 2020.
- ^ Silva, Marcela Fernandes; da Silva, Diego Salvador Muniz; Bacurau, Aldiane Gomes de Macedo; Francisco, Priscila Maria Stolses Bergamo; de Assumpção, Daniela; Neri, Anita Liberalesso; Borim, Flávia Silva Arbex (2021). "Ageism against older adults in the context of the COVID-19 pandemic: an integrative review". Revista de Saúde Pública. 55: 4. doi:10.11606/s1518-8787.2021055003082. ISSN 0034-8910. PMC 8023321. PMID 33886953.
- ^ "Data dive: How COVID-19 impacted ecommerce in 2020". Digital Commerce 360. Retrieved 27 March 2021.
- ^ "More Consumers Are Turning to Food Delivery Apps amid Indoor Dining Restrictions". eMarketer.com. Retrieved 28 March 2021.
- ^ "NYC Indoor Dining To Shut Down Monday, Cuomo Announces". Spectrum News NY1. Retrieved 28 March 2021.
- ^ "The future of hacking: COVID-19 shifting the way hackers work and who they target". SECURITY magazine. Retrieved 28 March 2021.
- ^ "The COVID-19 pandemic has changed education forever. This is how". World Economic Forum. Retrieved 28 March 2021.
- ^ "Pandemic Threatens Long-Term Job Security After Hospitality Industry Layoffs". NPR. Retrieved 28 March 2021.
- ^ "Travel industry layoffs begin as Congress fails to come up with new relief package". USA Today. Retrieved 28 March 2021.
- ^ "NIH COVID-19 Portfolio". Retrieved 9 August 2020.
- ^ Jerde S (12 March 2020). "Major Publishers Take Down Paywalls for Coronavirus Coverage". Adweek. Retrieved 25 March 2020.
- ^ "Sharing research data and findings relevant to the novel coronavirus (COVID-19) outbreak". wellcome.ac.uk (Press release). 31 January 2020. Retrieved 13 February 2020.
- ^ Aristovnik A, Ravšelj D, Umek L (November 2020). "A Bibliometric Analysis of COVID-19 across Science and Social Science Research Landscape". Sustainability. 12 (21): 9132. doi:10.3390/su12219132.
- ^ Rogers A (31 January 2020). "Coronavirus Research Is Moving at Top Speed – With a Catch". Wired. ISSN 1059-1028. Retrieved 13 February 2020.
- ^ Kent, Alexander James (August 2020). "Mapping and Counter-mapping COVID-19: From Crisis to Cartocracy". The Cartographic Journal. 57 (3): 187–195. doi:10.1080/00087041.2020.1855001. S2CID 230794926.
- ^ Hannah Murphy, Mark Di Stefano & Katrina Manson (20 March 2020). "Huge text message campaigns spread coronavirus fake news". Financial Times.
- ^ Affairs, Office of Regulatory (4 January 2021). "Fraudulent Coronavirus Disease 2019 (COVID-19) Products". FDA.
- ^ Kowalczyk, Oliwia; Roszkowski, Krzysztof; Montane, Xavier; Pawliszak, Wojciech; Tylkowski, Bartosz; Bajek, Anna (1 December 2020). "Religion and Faith Perception in a Pandemic of COVID-19". Journal of Religion and Health. 59 (6): 2671–2677. doi:10.1007/s10943-020-01088-3. ISSN 1573-6571. PMC 7549332. PMID 33044598.
- ^ "COVID: Top 10 current conspiracy theories". Alliance for Science. Retrieved 5 January 2021.
- ^ Kassam N (25 March 2020). "Disinformation and coronavirus". The Interpreter. Lowy Institute.
- ^ Kuhn, Sarah Anne Kezia; Lieb, Roselind; Freeman, Daniel; Andreou, Christina; Zander-Schellenberg, Thea (16 March 2021). "Coronavirus conspiracy beliefs in the German-speaking general population: endorsement rates and links to reasoning biases and paranoia". Psychological Medicine: 1–15. doi:10.1017/S0033291721001124. PMC 8027560. PMID 33722315. Retrieved 25 April 2021.
Further reading
- "Progress report on the coronavirus pandemic". Nature. 584 (7821): 325. 20 August 2020. doi:10.1038/d41586-020-02414-1. PMID 32814893.
- Tay MZ, Poh CM, Rénia L, MacAry PA, Ng LF (June 2020). "The trinity of COVID-19: immunity, inflammation and intervention". Nat. Rev. Immunol. 20 (6): 363–374. doi:10.1038/s41577-020-0311-8. PMC 7187672. PMID 32346093.
- COVID-19 infection prevention and control measures for primary care, including general practitioner practices, dental clinics and pharmacy settings: first update. European Centre for Disease Prevention and Control (ECDC) (Report). October 2020.
- Bar-On YM, Flamholz A, Phillips R, Milo R (31 March 2020). "SARS-CoV-2 (COVID-19) by the numbers". eLife. 9. arXiv:2003.12886. Bibcode:2020arXiv200312886B. doi:10.7554/eLife.57309. PMC 7224694. PMID 32228860.
- Brüssow H (March 2020). "The Novel Coronavirus – A Snapshot of Current Knowledge". Microbial Biotechnology. 2020 (3): 607–612. doi:10.1111/1751-7915.13557. PMC 7111068. PMID 32144890.
- Cascella, Marco; Rajnik, Michael; Cuomo, Arturo; Dulebohn, Scott C.; Di Napoli, Raffaela (2020). "Features, Evaluation, and Treatment of Coronavirus". StatPearls. StatPearls Publishing.
- Funk CD, Laferrière C, Ardakani A (2020). "A Snapshot of the Global Race for Vaccines Targeting SARS-CoV-2 and the COVID-19 Pandemic". Front Pharmacol. 11: 937. doi:10.3389/fphar.2020.00937. PMC 7317023. PMID 32636754.
- "Development and Licensure of Vaccines to Prevent COVID-19" (PDF). U.S. Food and Drug Administration (FDA). June 2020. Lay summary.
External links
| Scholia has a profile for COVID-19 pandemic (Q81068910). |
Health agencies
- COVID-19 (Questions & Answers, instructional videos; Facts/MythBusters) by the World Health Organization
- COVID-19 by the Government of Canada
- COVID-19 by the National Health Commission, China
- COVID-19 (Q&A) by the European Centre for Disease Prevention and Control
- COVID-19 (Q&A) by the Ministry of Health, Singapore
- COVID-19 (Q&A) by the U.S. Centers for Disease Control
- Coronavirus Disease 2019 (Q&A) by the U.S. National Institute for Occupational Safety and Health
Directories
- COVID-19 Directory on Curlie
- COVID-19 Resource Directory on OpenMD
- Coronavirus Resource Center at the Center for Inquiry
Data and graphs
- Coronavirus disease (COVID-2019) situation reports and map by the World Health Organization
- Coronavirus Resource Center, map, and historical data by Johns Hopkins University
- COVID-19 data sets published by the European Centre for Disease Prevention and Control (ECDC)
- Coronavirus Observer based on Johns Hopkins University data
- COVID-19 Statistics and Research published by Our World in Data
- COVID-19 Tracker from Stat News
- COVID-19 Projections for many countries published by Institute for Health Metrics and Evaluation
- Spreadsheets: Country comparisons
- Epidemic Calculator
- World Travel Restrictions based on WFP data
Medical journals
- Coronavirus: News and Resources by BMJ Publishing Group
- Novel Coronavirus Information Center by Elsevier
- Coronavirus Disease 2019 (COVID-19) by JAMA
- COVID-19 Resource Centre by The Lancet
- COVID-19 Research Highlights by Springer Nature
- Coronavirus (COVID-19) by The New England Journal of Medicine
- COVID-19 pandemic (2019–20) Collection by PLOS
- COVID-19: Novel Coronavirus by Wiley Publishing
- COVID-19 Portfolio, a curated collection of publications and preprints by NIH
Research foundations
- "COVID-19 Daily Dispatch & news HUB". tctMD.com. Cardiovascular Research Foundation.
Information
Article COVID-19 pandemic in English Wikipedia took following places in local popularity ranking:
- 4 place in 2020-06-08
About the page
Presented content of the Wikipedia article was extracted in 2021-06-13 based on https://en.wikipedia.org/?curid=62750956